Dermatome overlap and clinical implications — MCQs

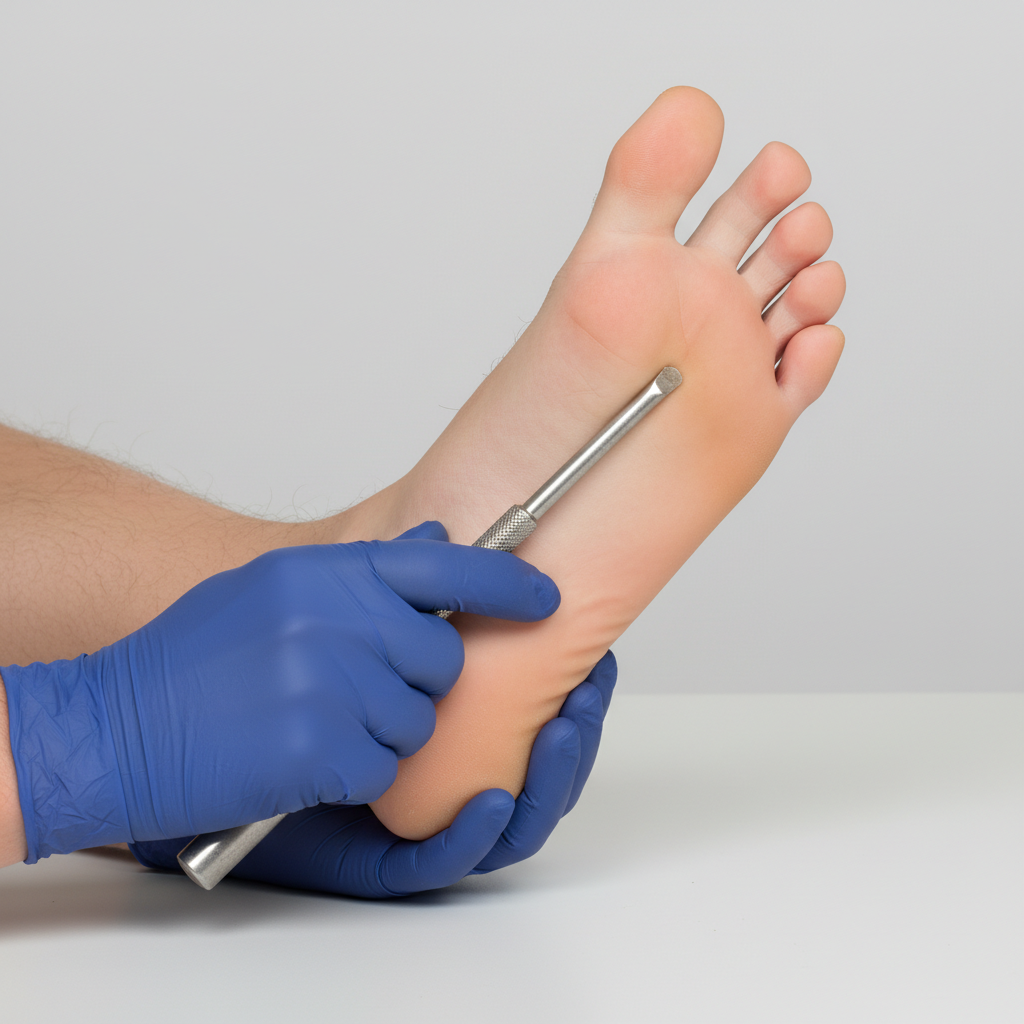
You are seeing a patient in clinic who presents with complaints of weakness. Her physical exam is notable for right sided hyperreflexia, as well as the reflex finding shown in the image below. Where is the most likely location of this patient's lesion?
A 50-year-old male is brought to the dermatologist's office with complaints of a pigmented lesion. The lesion is uniformly dark with clean borders and no asymmetry and has been increasing in size over the past two weeks. He works in construction and spends large portions of his day outside. The dermatologist believes that this mole should be biopsied. To prepare the patient for the biopsy, the dermatologist injects a small amount of lidocaine into the skin around the lesion. Which of the following nerve functions would be the last to be blocked by the lidocaine?
A 65-year-old man presents to a clinic after 2 days of pain just below the right nipple. The pain radiates to the scapula. The rash was preceded by a burning and tingling pain in the affected region. His medical history is relevant for hypertension and hypercholesterolemia. He does not recall his vaccination status or childhood illnesses. A physical examination reveals stable vital signs and a vesicular rash distributed along the T4 dermatome. Which of the following is most appropriate for treating his condition and preventing further complications?
A 63-year-old man comes to the physician because of a 2-day history of a painful rash on his right flank. Two years ago, he underwent cadaveric renal transplantation. Current medications include tacrolimus, mycophenolate mofetil, and prednisone. Examination shows an erythematous rash with grouped vesicles in a band-like distribution over the patient's right flank. This patient is at greatest risk for which of the following complications?
A 23-year-old man presents to the emergency department with a severe headache. The patient states he gets sudden, severe pain over his face whenever anything touches it, including shaving or putting lotion on his skin. He describes the pain as electric and states it is only exacerbated by touch. He is currently pain free. His temperature is 98.1°F (36.7°C), blood pressure is 127/81 mmHg, pulse is 87/min, respirations are 15/min, and oxygen saturation is 98% on room air. Neurological exam is within normal limits, except severe pain is elicited with light palpation of the patient’s face. The patient is requesting morphine for his pain. Which of the following is the most likely diagnosis?
A 37-year-old man presents to his primary care provider complaining of bilateral arm numbness. He was involved in a motor vehicle accident 3 months ago. His past medical history is notable for obesity and psoriatic arthritis. He takes adalimumab. His temperature is 99.3°F (37.4°C), blood pressure is 130/85 mmHg, pulse is 90/min, and respirations are 18/min. On exam, superficial skin ulcerations are found on his fingers bilaterally. His strength is 5/5 bilaterally in shoulder abduction, arm flexion, arm extension, wrist extension, finger abduction, and thumb flexion. He demonstrates loss of light touch and pinprick response in the distal tips of his 2nd and 5th fingertips and over the first dorsal web space. Vibratory sense is intact in the bilateral upper and lower extremities. Which of the following nervous system structures is most likely affected in this patient?
A 59-year-old woman presents to the emergency room with severe low back pain. She reports pain radiating down her left leg into her left foot. She also reports intermittent severe lower back spasms. The pain started after lifting multiple heavy boxes at her work as a grocery store clerk. She denies bowel or bladder dysfunction. Her past medical history is notable for osteoporosis and endometrial cancer. She underwent a hysterectomy 20 years earlier. She takes alendronate. Her temperature is 99°F (37.2°C), blood pressure is 135/85 mmHg, pulse is 85/min, and respirations are 22/min. Her BMI is 21 kg/m^2. On exam, she is unable to bend over due to pain. Her movements are slowed to prevent exacerbating her muscle spasms. A straight leg raise elicits severe radiating pain into her left lower extremity. The patient reports that the pain is worst along the posterior thigh and posterolateral leg into the fourth and fifth toes. Palpation along the lumbar vertebral spines demonstrates mild tenderness. Patellar reflexes are 2+ bilaterally. The Achilles reflex is decreased on the left. Which nerve root is most likely affected in this patient?
A 57-year-old man presents to the ED complaining of back and left leg pain. He was lifting heavy furniture while helping his daughter move into college when all of sudden he felt a sharp pain at his back. The pain is described as severe, worse with movement, and shoots down his lateral thigh. The patient denies any bowel/urinary incontinence, saddle anesthesia, weight loss, or weakness. He denies any past medical history but endorses a family history of osteoporosis. He has been smoking 1 pack per day for the past 20 years. Physical examination demonstrated decreased sensation at the left knee, decreased patellar reflex, and a positive straight leg test. There is diffuse tenderness to palpation at the lower back but no vertebral step-offs were detected. What is the most likely etiology for this patient’s pain?
A 54-year-old woman comes to the physician because of a 1-day history of fever, chills, and double vision. She also has a 2-week history of headache and foul-smelling nasal discharge. Her temperature is 39.4°C (103°F). Examination shows mild swelling around the left eye. Her left eye does not move past midline on far left gaze but moves normally when looking to the right. Without treatment, which of the following findings is most likely to occur in this patient?
A 28-year-old man comes to the physician because of a 3-month history of pain in his left shoulder. He is physically active and plays baseball twice a week. The pain is reproduced when the shoulder is externally rotated against resistance. Injury of which of the following tendons is most likely in this patient?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
