Upper limb cross-sections — MCQs

A 43-year-old woman comes to the physician because of tingling and weakness in her left arm for the past 2 days. An image of the brachial plexus is shown. Nerve conduction study shows decreased transmission of electrical impulses in the labeled structure. Physical examination is most likely to show impairment of which of the following movements?
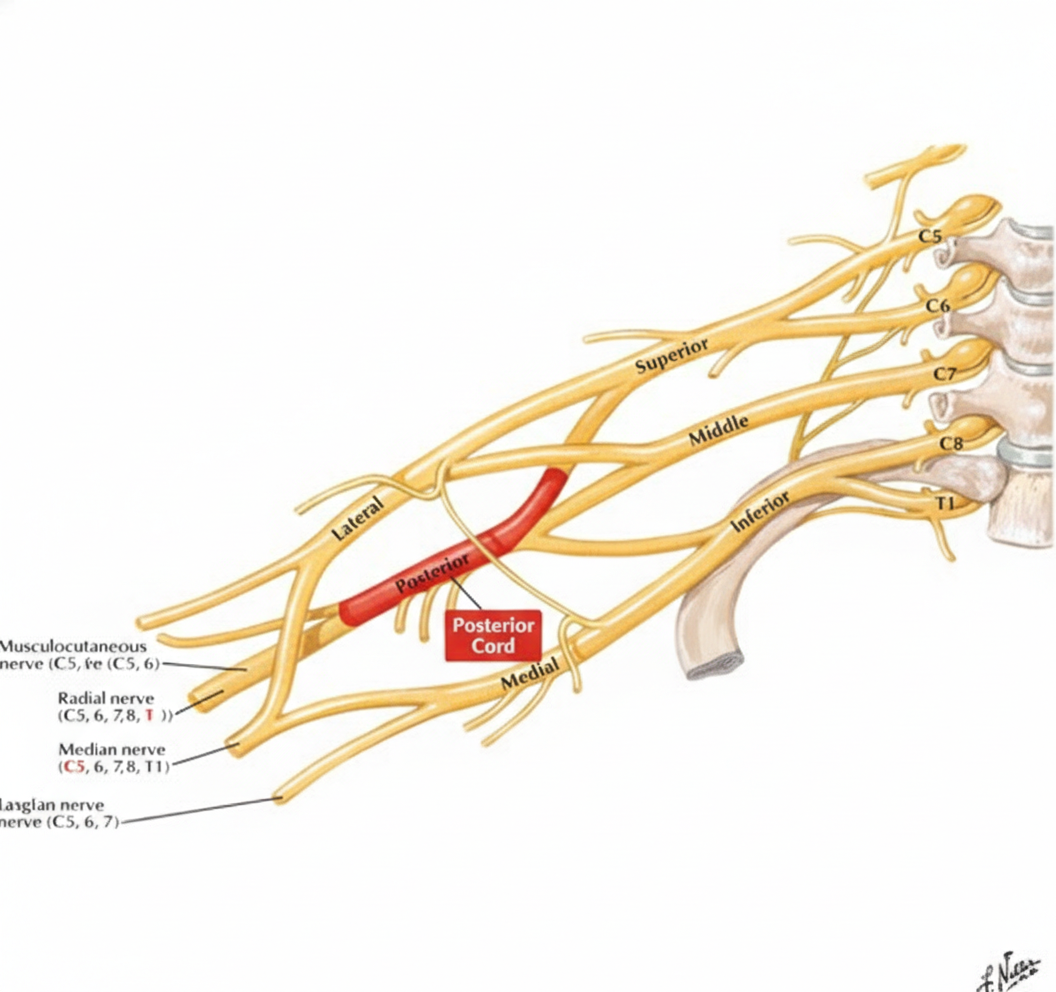
A 53-year-old woman comes to the physician because of a 3-month history of intermittent severe left neck, shoulder, and arm pain and paresthesias of the left hand. The pain radiates to the radial aspect of her left forearm, thumb, and index finger. She first noticed her symptoms after helping a friend set up a canopy tent. There is no family history of serious illness. She appears healthy. Vital signs are within normal limits. When the patient extends and rotates her head to the left and downward pressure is applied, she reports paresthesias along the radial aspect of her left forearm and thumb. There is weakness when extending the left wrist against resistance. The brachioradialis reflex is 1+ on the left and 2+ on the right. The radial pulse is palpable bilaterally. The remainder of the examination shows no abnormalities. Which of the following is the most likely diagnosis?
A 25-year-old woman comes to the physician because of pain and weakness in her right forearm and hand for several months. Two years ago, she sustained a fracture of her ulnar shaft with dislocation of the radial head that was treated surgically. Physical examination shows mild tenderness a few centimeters distal to the lateral epicondyle. She has marked weakness when attempting to extend her right middle finger. There is radial deviation on extension of the wrist. Sensation is not impaired. Which of the following nerves is most likely affected in this patient?
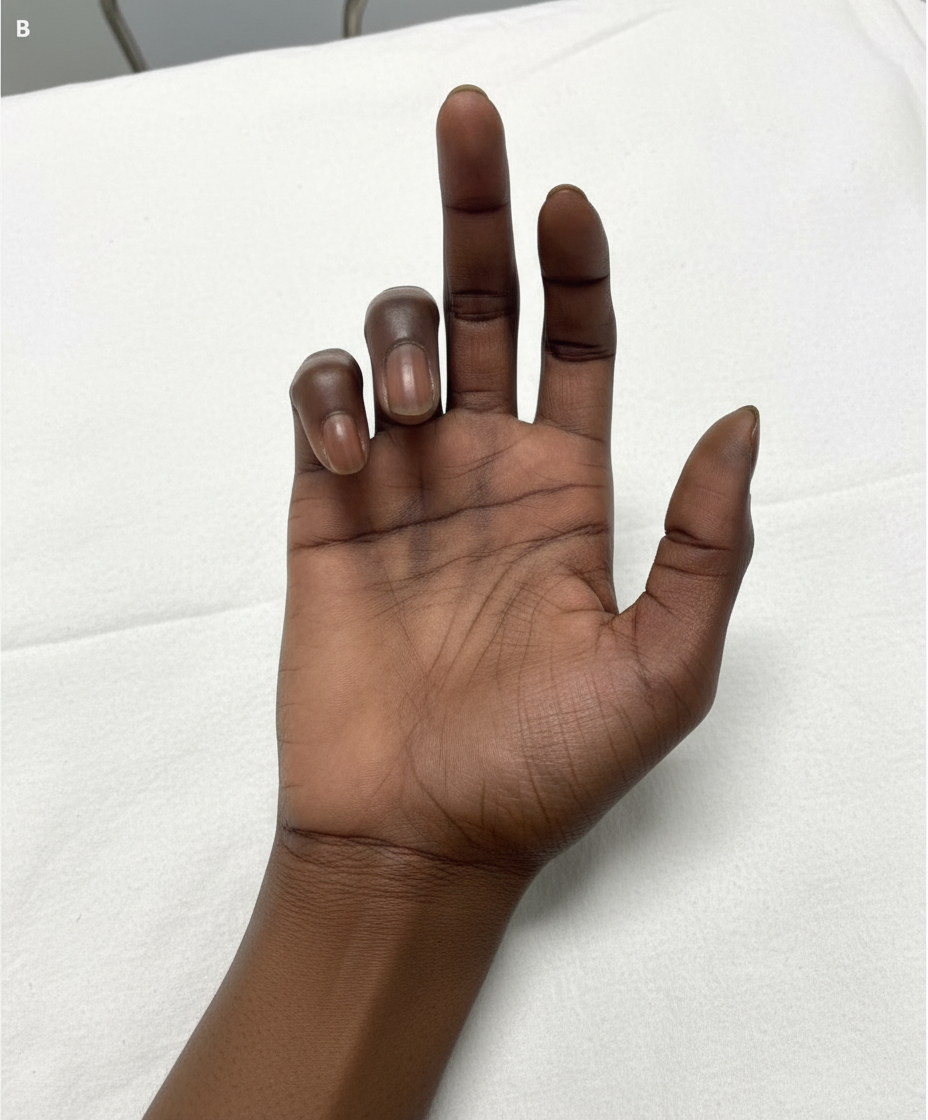
A 30-year-old man presents with weakness in his right hand. He says he has been an avid cyclist since the age of 20. He denies any recent trauma. Physical examination reveals decreased sensations over the 4th and 5th digits with difficulty extending the 4th and 5th digits. Strength is 4 out of 5 in the extensor muscles of the right hand and wrist. When the patient is asked to extend his fingers, the result is shown in the image. Which of the following nerves is most likely damaged in this patient?
A 61-year-old woman comes to the physician for a follow-up examination 1 week after undergoing right-sided radical mastectomy and axillary lymph node dissection for breast cancer. She says that she has been unable to comb her hair with her right hand since the surgery. Physical examination shows shoulder asymmetry. She is unable to abduct her right arm above 90 degrees. When she pushes against a wall, there is protrusion of the medial aspect of the right scapula. Injury to which of the following nerves is the most likely cause of this patient's condition?
A 61-year-old woman comes to her physician for a burning sensation and numbness in her right hand for 4 weeks. The burning sensation is worse at night and is sometimes relieved by shaking the wrist. In the past week, she has noticed an exacerbation of her symptoms. She has rheumatoid arthritis and type 2 diabetes mellitus. Her medications include insulin, methotrexate, and naproxen. Her vital signs are within normal limits. Examination shows swan neck deformities of the fingers on both hands and multiple subcutaneous nodules over bilateral olecranon processes. There is tingling and numbness over the right thumb, index finger, and middle finger when the wrist is actively flexed. The remainder of the examination shows no abnormalities. Which of the following is the most appropriate next best step in management?
A 25-year-old man was referred to a neurologist for right-hand weakness. He was involved in a motor vehicle accident 2 months ago in which his right hand was injured. On examination, his grip is weak, especially in fingers 2, 4, and 5 and he is unable to adduct these fingers. Which of the following groups of muscles is most likely affected?
A 47-year-old woman presents to her primary care provider because of numbness and tingling on the palmar aspects of both hands. She denies any symptoms at the base of her thumbs. The symptoms are worse on the right (dominant hand) and are increased with activities such as driving or brushing her hair. She frequently wakes up with pain and has to shake her hand for pain relief. She has had rheumatoid arthritis for 9 years, for which she takes methotrexate. Her blood pressure is 124/76 mm Hg, the heart rate is 75/min, and the respiratory rate is 15/min. Lightly tapping over the middle of the anterior aspect of the right wrist leads to a tingling sensation in the palm. In this patient, electromyography (EMG) will most likely show which of the following results?
A 60-year-old woman is rushed to the emergency room after falling on her right elbow while walking down the stairs. She cannot raise her right arm. Her vital signs are stable, and the physical examination reveals loss of sensation over the upper lateral aspect of the right arm and shoulder. A radiologic evaluation shows a fracture of the surgical neck of the right humerus. Which of the following muscles is supplied by the nerve that is most likely damaged?
A 35-year-old man is brought to the trauma bay by ambulance after sustaining a gunshot wound to the right arm. The patient is in excruciating pain and states that he can't move or feel his hand. The patient states that he has no other medical conditions. On exam, the patient's temperature is 98.4°F (36.9°C), blood pressure is 140/86 mmHg, pulse is 112/min, and respirations are 14/min. The patient is alert and his Glasgow coma scale is 15. On exam, he has a single wound on his right forearm without continued bleeding. The patient has preserved motor and sensation in his right elbow; however, he is unable to extend his wrist or extend his fingers further. He is able to clench his hand, but this is limited by pain. On sensory exam, the patient has no sensation to the first dorsal web space but has preserved sensation on most of the volar surface. Which of the following structures is most likely injured?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
