Corticospinal tracts — MCQs

On this page
A 46-year-old man comes to the physician because of a 2-month history of hoarseness and drooling. Initially, he had difficulty swallowing solid food, but now he has difficulty swallowing foods like oatmeal as well. During this period, he also developed weakness in both arms and has had an 8.2 kg (18 lb) weight loss. He appears ill. His vital signs are within normal limits. Examination shows tongue atrophy and pooled oral secretions. There is diffuse muscle atrophy in all extremities. Deep tendon reflexes are 3+ in all extremities. Sensation to pinprick, light touch, and vibration is intact. An esophagogastroduodenoscopy shows no abnormalities. Which of the following is the most likely cause of this patient's symptoms?
A 45-year-old woman comes to the physician’s office with complaints of clumsiness. She feels like she is tripping over her feet more often, and she recently fell and sprained her wrist. Her medical history is significant for well-controlled diabetes. She has been a strict vegan for over 20 years. She lives at home with her husband and two children. On exam, she appears well-nourished. She has diminished proprioception and vibration sense in both her feet. She has a positive Romberg sign. She has diminished Achilles reflexes bilaterally. Which of the following tracts are most likely damaged in this patient?
A 34-year-old man presents to the emergency department with leg weakness that significantly impairs and slows down his walking ability. He has noticed that he has been getting progressively weaker over the past 3 months. He has also experienced spontaneous twitching in his arms and thighs that is becoming more frequent. On physical examination, moderate atrophy of his arm and thigh muscles is observed. Significant thenar atrophy is noted bilaterally, and deep tendon reflexes are increased. His lower limbs have resistance to movement and feel rigid. Pupillary light and accommodation reflexes are both normal. The patient can maintain his balance upon closing his eyes. Considering this case presentation, which of the following is the likely site of the lesion?
A 39-year-old woman is brought to the emergency department following a stab wound to the neck. Per the patient, she was walking her dog when she got robbed and was subsequently stabbed with a knife. Vitals are stable. Strength examination reveals 2/5 right-sided elbow flexion and extension, wrist extension, and finger motions. Babinski sign is upward-going on the right. There is decreased sensation to light touch and vibration on the patient's right side up to her shoulder. She also reports decreased sensation to pinprick and temperature on her left side, including her lower extremities, posterior forearm, and middle finger. The patient's right pupil is 2 mm smaller than the left with drooping of the right upper eyelid. Which of the following is the most likely cause of the patient’s presentation?
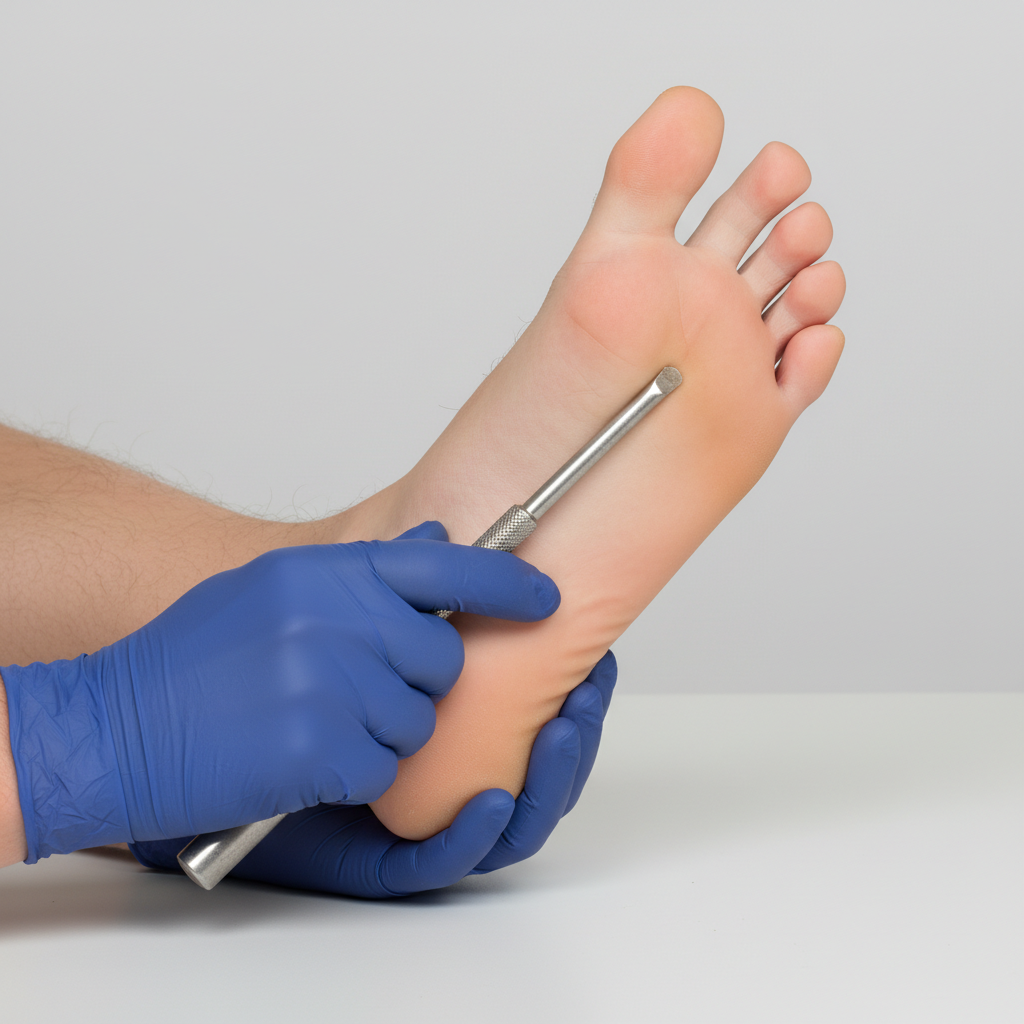
You are seeing a patient in clinic who presents with complaints of weakness. Her physical exam is notable for right sided hyperreflexia, as well as the reflex finding shown in the image below. Where is the most likely location of this patient's lesion?
A 61-year-old man is brought to the emergency department because of increasing weakness of his right arm and leg that began when he woke up that morning. He did not notice any weakness when he went to bed the night before. He has hypertension and hypercholesterolemia. Current medications include hydrochlorothiazide and atorvastatin. He is alert and oriented to person, time, place. His temperature is 36.7°C (98°F), pulse is 91/min, and blood pressure is 132/84 mm Hg. Examination shows drooping of the right side of the face. Muscle strength is decreased in the right upper and lower extremities. Deep tendon reflexes are 4+ on the right side. Sensation is intact. His speech is normal in rate and rhythm. The remainder of the examination shows no abnormalities. An infarction of which of the following sites is the most likely cause of this patient's symptoms?
A 61-year-old man is brought to the emergency department by his son after collapsing to the ground while at home. His son immediately performed cardiopulmonary resuscitation and later the patient underwent successful defibrillation after being evaluated by the emergency medical technician. The patient has a medical history of hypertension, hyperlipidemia, and type II diabetes mellitus. He has smoked one-half pack of cigarettes for approximately 30 years. The patient was admitted to the cardiac intensive care unit, and after a few days developed acute onset right upper extremity weakness. His temperature is 99°F (37.2°C), blood pressure is 145/91 mmHg, pulse is 102/min and irregularly irregular, and respirations are 16/min. On physical examination, the patient is alert and orientated to person, place, and time. His language is fluent and he is able to name, repeat, and read. His strength is 5/5 throughout except in the right hand, wrist, and arm, which is 2/5. Based on this patient's clinical presentation, the affected neuronal fibers decussate at which level of the central nervous system?
Practice by Chapter
Origin and course of lateral corticospinal tract
Practice Questions
Origin and course of anterior corticospinal tract
Practice Questions
Upper motor neuron anatomy
Practice Questions
Lower motor neuron anatomy
Practice Questions
Decussation of pyramids
Practice Questions
Somatotopic organization
Practice Questions
Alternative motor pathways
Practice Questions
UMN vs LMN lesions
Practice Questions
Spinal cord injury levels and their effects
Practice Questions
Clinical testing of corticospinal tract function
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
