Lower motor neuron anatomy — MCQs

You are seeing a patient in clinic who presents with complaints of weakness. Her physical exam is notable for right sided hyperreflexia, as well as the reflex finding shown in the image below. Where is the most likely location of this patient's lesion?
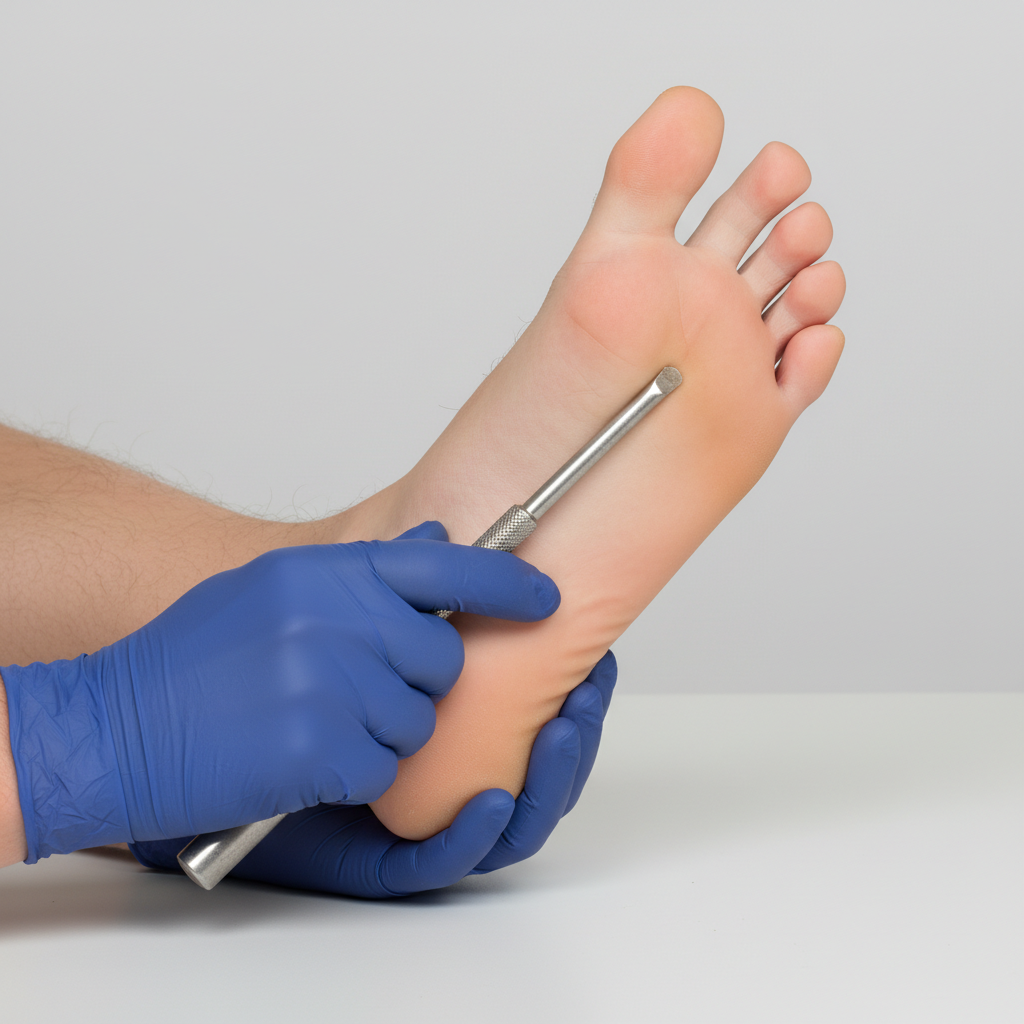
A 45-year-old man presents to the physician with complaints of burning pain in both feet and lower legs for 3 months. He reports that the pain is especially severe at night. He has a history of diabetes mellitus for the past 5 years, and he frequently skips his oral antidiabetic medications. His temperature is 36.9°C (98.4°F), heart rate is 80/min, respiratory rate is 15/min, and blood pressure is 120/80 mm Hg. His weight is 70 kg (154.3 lb) and height is 165 cm (approx. 5 ft 5 in). The neurologic examination reveals loss of sensations of pain and temperature over the dorsal and ventral sides of the feet and over the distal one-third of both legs. Proprioception is normal; knee jerks and ankle reflexes are also normal. The tone and strength in all muscles are normal. The hemoglobin A1C is 7.8%. Involvement of what type of nerve fibers is the most likely cause of the patient’s symptoms?
A 32-year-old woman presents to the clinic with the complaint of excessive fatigue for the past few weeks. After returning home from the office, she feels too tired to climb up the stairs, comb her hair, or chew her food. She has occasionally experienced double vision. She denies any history of fever, cough, weight loss, night sweats, or snoring. Past history is unremarkable. Physical examination reveals: blood pressure 124/86 mm Hg, heart rate 85/min, respiratory rate 14/min, temperature 37.0°C (98.6°F), and body mass index (BMI) 22.6 kg/m2. On examination, the right upper eyelid is slightly drooping when compared to the left side. Her eye movements are normal. Flexion of the neck is mildly weak. Muscle strength is 5/5 in all 4 limbs. When she is asked to alternately flex and extend her shoulder continuously for 5 minutes, the power in the proximal upper limb muscles becomes 4/5. The muscle tone and deep tendon reflexes are normal. What is the most appropriate test to diagnose this condition?
An investigator is developing a drug that selectively inhibits the retrograde axonal transport of rabies virus towards the central nervous system. To achieve this effect, this drug must target which of the following?
A 62-year-old woman is brought to the physician because of 6 months of progressive weakness in her arms and legs. During this time, she has also had difficulty swallowing and holding her head up. Examination shows pooling of oral secretions. Muscle strength and tone are decreased in the upper extremities. Deep tendon reflexes are 1+ in the right upper and lower extremities, 3+ in the left upper extremity, and 4+ in the left lower extremity. Sensation to light touch, pinprick, and vibration are intact. Which of the following is the most likely diagnosis?
A 32-year-old woman presents with diplopia. She says that she has been experiencing drooping of her eyelids and severe muscle weakness. She reports that her symptoms are worse at the end of the day. Which of the following additional findings would most likely be seen in this patient?
A 5-year-old boy who recently emigrated from Nigeria is brought to the emergency department because of a 2-day history of lower leg weakness, swallowing difficulty, and drooling of saliva. He has not yet received any childhood vaccinations. Two days after admission, the patient develops shortness of breath. Pulse oximetry shows an oxygen saturation of 64%. Despite resuscitative efforts, the patient dies of respiratory failure. At autopsy, examination of the spinal cord shows destruction of the anterior horn cells. Neurological examination of this patient would have most likely shown which of the following findings?
During a physical examination, a physician tests the strength of hip adduction against resistance. Which of the following nerves innervates the primary muscles responsible for this action?
A 46-year-old man comes to the physician because of a 2-month history of hoarseness and drooling. Initially, he had difficulty swallowing solid food, but now he has difficulty swallowing foods like oatmeal as well. During this period, he also developed weakness in both arms and has had an 8.2 kg (18 lb) weight loss. He appears ill. His vital signs are within normal limits. Examination shows tongue atrophy and pooled oral secretions. There is diffuse muscle atrophy in all extremities. Deep tendon reflexes are 3+ in all extremities. Sensation to pinprick, light touch, and vibration is intact. An esophagogastroduodenoscopy shows no abnormalities. Which of the following is the most likely cause of this patient's symptoms?
A 61-year-old man is brought to the emergency department because of increasing weakness of his right arm and leg that began when he woke up that morning. He did not notice any weakness when he went to bed the night before. He has hypertension and hypercholesterolemia. Current medications include hydrochlorothiazide and atorvastatin. He is alert and oriented to person, time, place. His temperature is 36.7°C (98°F), pulse is 91/min, and blood pressure is 132/84 mm Hg. Examination shows drooping of the right side of the face. Muscle strength is decreased in the right upper and lower extremities. Deep tendon reflexes are 4+ on the right side. Sensation is intact. His speech is normal in rate and rhythm. The remainder of the examination shows no abnormalities. An infarction of which of the following sites is the most likely cause of this patient's symptoms?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
