Vascular Surgery — MCQs

On this page
Intermittent claudication is seen when the ankle-brachial index is?
Complications arising out of A-V fistula done for renal failure include the following EXCEPT?
A 45-year-old woman presents with right lower extremity swelling and multiple varicosities two months after undergoing cardiac catheterization via a right femoral approach. Examination reveals a bruit over the right groin. What is the most likely diagnosis?
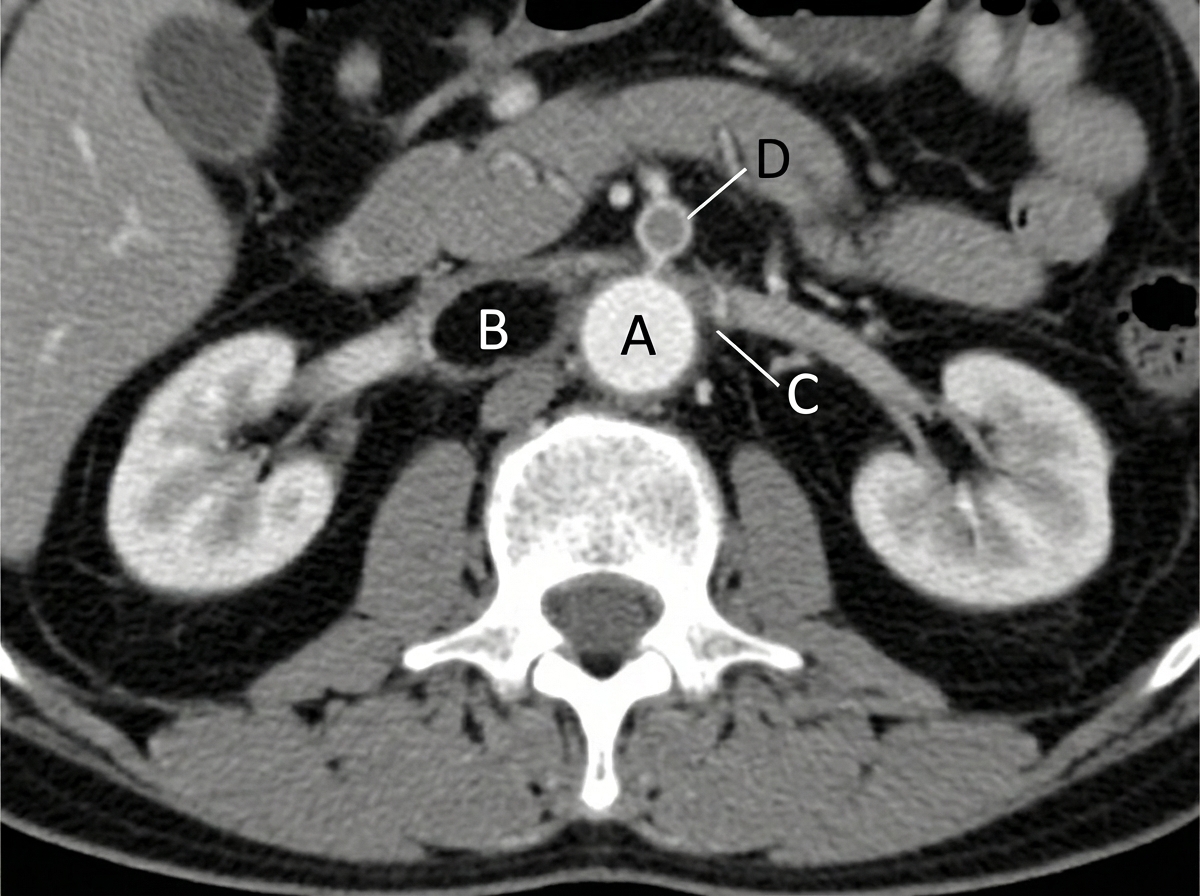
A 70-year-old woman with a history of myocardial ischemia and peripheral vascular disease presented with sudden onset of severe, rapidly increasing epigastric pain, nausea, vomiting, and minimal abdominal tenderness. She was writhing in pain, had normal bowel sounds, and a small amount of blood in her stool. Electrolyte analysis revealed a bicarbonate level of 15 mEq/L, and serum lactate was elevated, indicating tissue hypoxia and injury. A CT scan was planned. What anatomical structure is likely involved?
Which of the following describes stage 3 limb ischemia as per the Fontaine classification?
Which sympathetic ganglia are spared in a lumbar sympathectomy?
Which of the following statements about ischemic rest pain is TRUE?
In the CEAP classification of varicose veins, which stage is characterized by the 'beer bottle appearance'?
A 24-year-old man complains of progressive intermittent claudication of the left leg. On examination, the popliteal, dorsalis pedis, and posterior tibial pulses are normal but disappear on dorsiflexion of the foot. What is the most likely diagnosis?
Which one of the following is NOT a feature of Leriche syndrome?
Practice by Chapter
Atherosclerotic Disease
Practice Questions
Aortic Aneurysms
Practice Questions
Peripheral Arterial Disease
Practice Questions
Carotid Artery Disease
Practice Questions
Venous Thromboembolism
Practice Questions
Chronic Venous Insufficiency
Practice Questions
Mesenteric Vascular Disease
Practice Questions
Vascular Trauma
Practice Questions
Vascular Access for Hemodialysis
Practice Questions
Endovascular Techniques
Practice Questions
Diabetic Foot Vascular Disease
Practice Questions
Vasculitis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
