Vascular Surgery — MCQs

On this page
Which of the following is NOT a clinical presentation of Peripheral arterial occlusion?
In an extraperitoneal approach for left sympathectomy, which of the following structures may be injured?
Following graft repair of a thoraco-abdominal aneurysm, a patient develops lower limb weakness. What is the most probable cause for this complication?
What is the most common site of lymph node enlargement in Hodgkin's lymphoma?
What are the presenting symptoms of immunoproliferative small intestinal lymphoma?
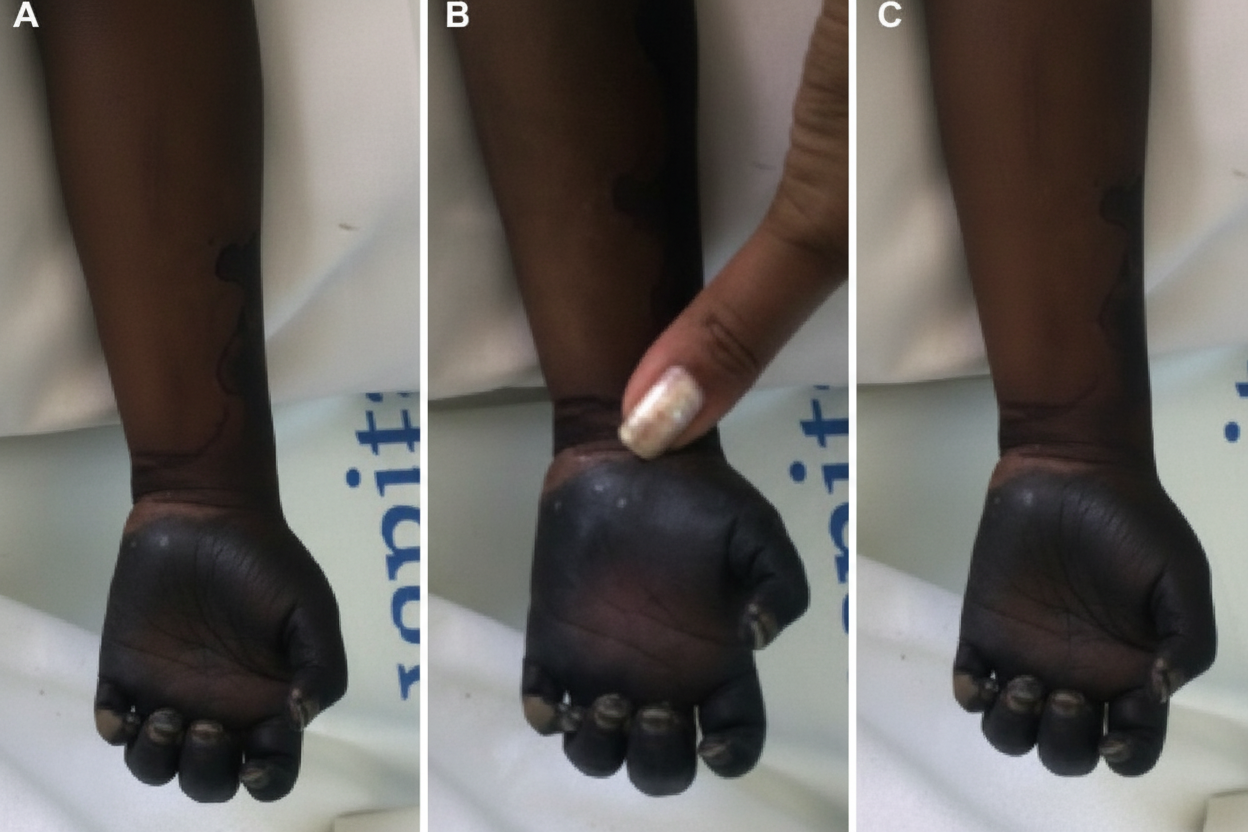
A 30-year-old chronic smoker male presents with a condition requiring diagnosis. What is the most likely diagnosis?
Which of the following is not a complication of surgery for thoracic outlet syndrome?
Which of the following statements is true regarding a descending aortic dissection?
Which of the following best describes Buerger's disease?
What is the most common cause of a thrombus in the common femoral artery in a 40-year-old male?
Practice by Chapter
Atherosclerotic Disease
Practice Questions
Aortic Aneurysms
Practice Questions
Peripheral Arterial Disease
Practice Questions
Carotid Artery Disease
Practice Questions
Venous Thromboembolism
Practice Questions
Chronic Venous Insufficiency
Practice Questions
Mesenteric Vascular Disease
Practice Questions
Vascular Trauma
Practice Questions
Vascular Access for Hemodialysis
Practice Questions
Endovascular Techniques
Practice Questions
Diabetic Foot Vascular Disease
Practice Questions
Vasculitis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
