Vascular Surgery — MCQs

On this page
What is the treatment of femoral artery aneurysm?
What does Grade I lymphedema mean?
What is true about primary lymphedema?
What is the primary treatment for an acute femoral embolus?
Lumbar sympathectomy is not indicated in which of the following conditions?
Milroy's disease is an example of:
A 72-year-old woman presents with a fall after an episode of dizziness, accompanied by 3 days of low-back pain. She is hypotensive and has cold, clammy extremities. A pulsating mass is palpable on abdominal examination. Following resuscitation, what is the next most appropriate step in management?
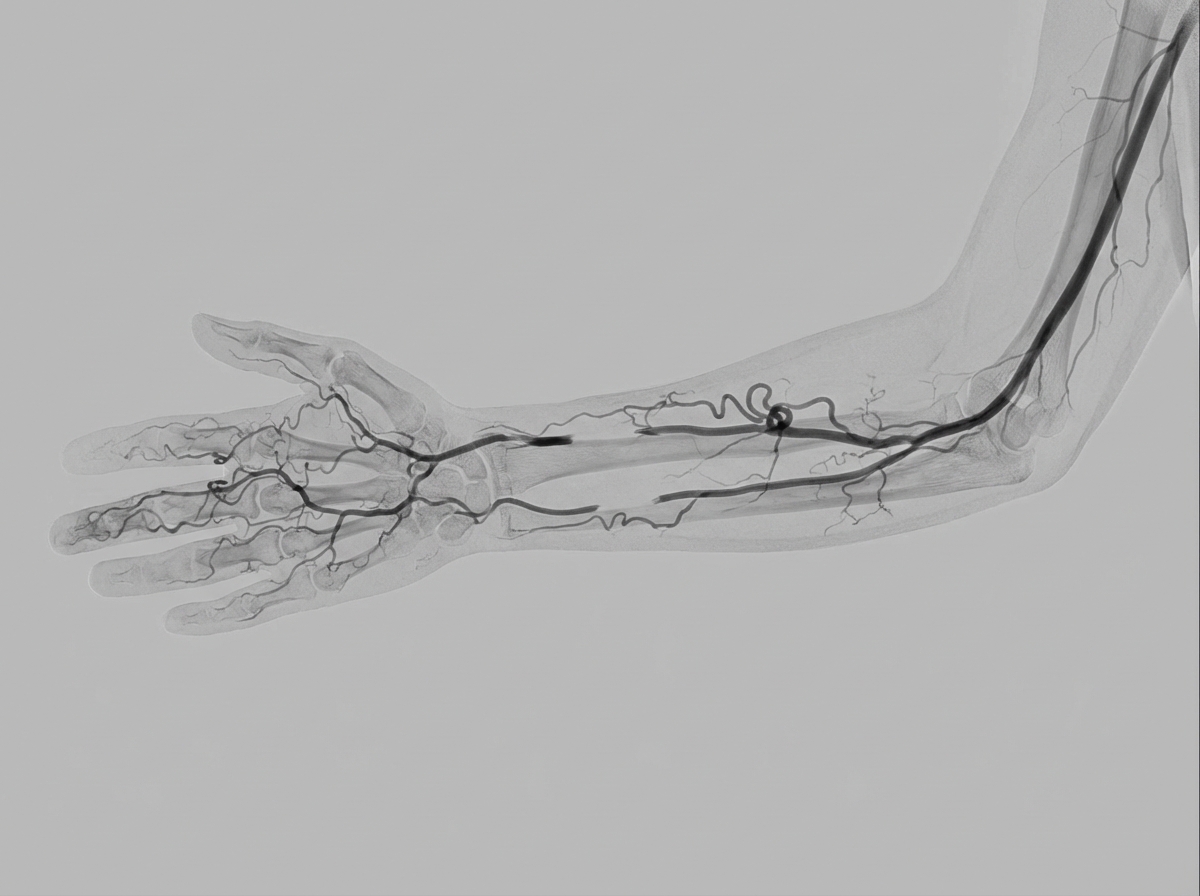
A 30-year-old construction worker presented with exertional pain in his bilateral forearms and hands. There is a history of chronic cigarette smoking. On examination, faint radial and ulnar pulses were noted, with easily palpable brachial pulses. Angiography of the hand was performed. Which of the following is the best treatment for this condition?
Fogarty's catheter is used for what purpose?
Left sided portal hypertension is best treated by:
Practice by Chapter
Atherosclerotic Disease
Practice Questions
Aortic Aneurysms
Practice Questions
Peripheral Arterial Disease
Practice Questions
Carotid Artery Disease
Practice Questions
Venous Thromboembolism
Practice Questions
Chronic Venous Insufficiency
Practice Questions
Mesenteric Vascular Disease
Practice Questions
Vascular Trauma
Practice Questions
Vascular Access for Hemodialysis
Practice Questions
Endovascular Techniques
Practice Questions
Diabetic Foot Vascular Disease
Practice Questions
Vasculitis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
