Vascular Surgery — MCQs

On this page
Buerger's disease is associated with:
An arteriogram of a 75-year-old man with an asymptomatic carotid bruit, mild hypertension, and mild COPD is shown. What is the current recommended management for this patient?
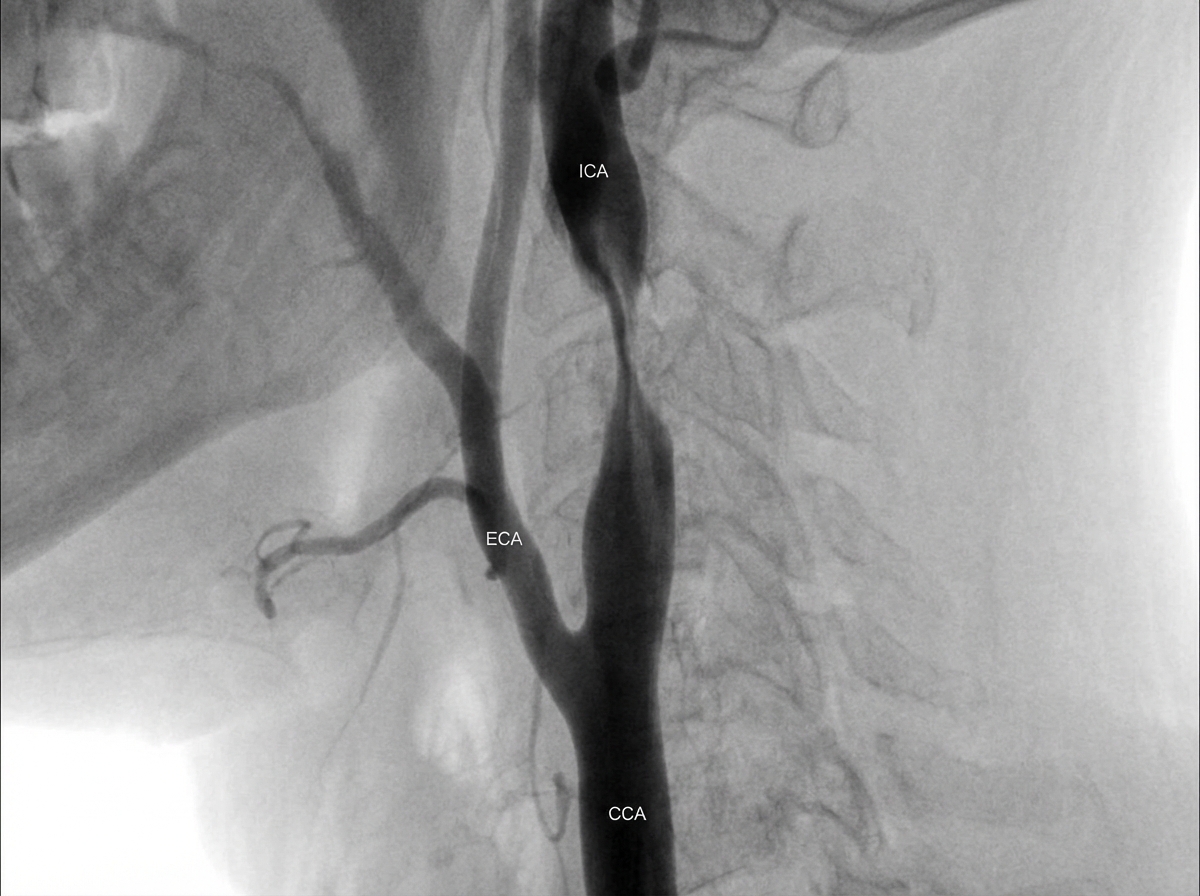
A 40-year-old male, a chronic smoker, presents with claudication and a medial leg ulcer. For the past one month, he is experiencing rest pain. Which of the following procedures would not relieve his rest pain?
Intermittent claudication at the hip level indicates which of the following?
A Potts shunt is:
Congenital arteriovenous fistulas in the thigh will be associated with all of the following except?
What is the purpose of the device shown below?
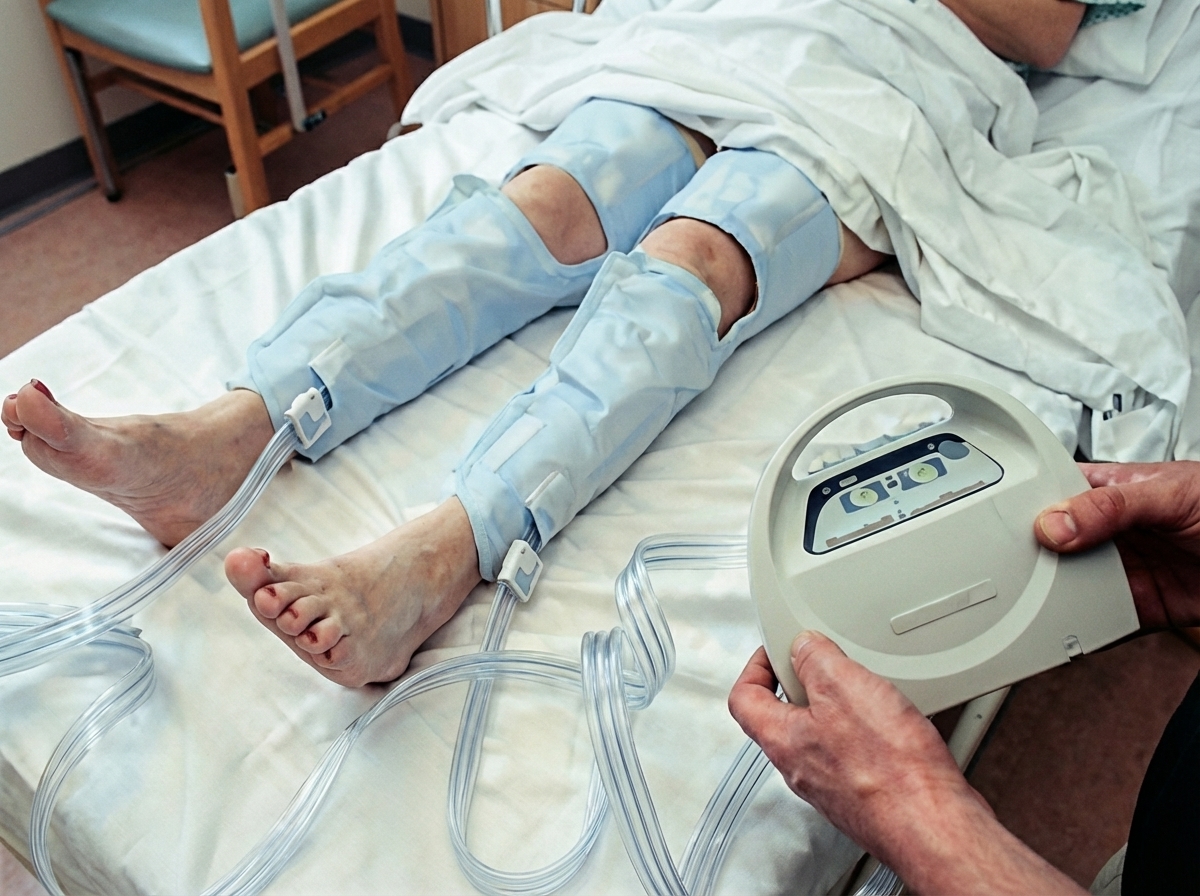
What are the causes of unilateral lymphedema of the leg that should be investigated?
Regarding varicose veins, which one of the following statements is true?
Which of the following statements about carotid stenosis is true?
Practice by Chapter
Atherosclerotic Disease
Practice Questions
Aortic Aneurysms
Practice Questions
Peripheral Arterial Disease
Practice Questions
Carotid Artery Disease
Practice Questions
Venous Thromboembolism
Practice Questions
Chronic Venous Insufficiency
Practice Questions
Mesenteric Vascular Disease
Practice Questions
Vascular Trauma
Practice Questions
Vascular Access for Hemodialysis
Practice Questions
Endovascular Techniques
Practice Questions
Diabetic Foot Vascular Disease
Practice Questions
Vasculitis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
