Carotid Artery Disease — MCQs

Investigation of choice for screening of proximal internal carotid artery stenosis is :
All of the following come under priority of Stroke control programme EXCEPT:
Following are the risk factors of atherosclerosis, except?
Anterior choroidal artery is a branch of which of the following arteries?
A woman presenting with abrupt onset of "the worst headache of her life" Which is the best investigation?
Which of the following is the best management for radiation induced occlusive disease of carotid artery?
Which of these is a palliative shunt procedure created between the left subclavian artery and pulmonary artery to treat cyanotic congenital heart disease?
Following endarterectomy on the right common carotid, a patient is found to be blind in the right eye. It appears that a small thrombus embolized during surgery and lodged in the artery supplying the retina. Which artery would be blocked?
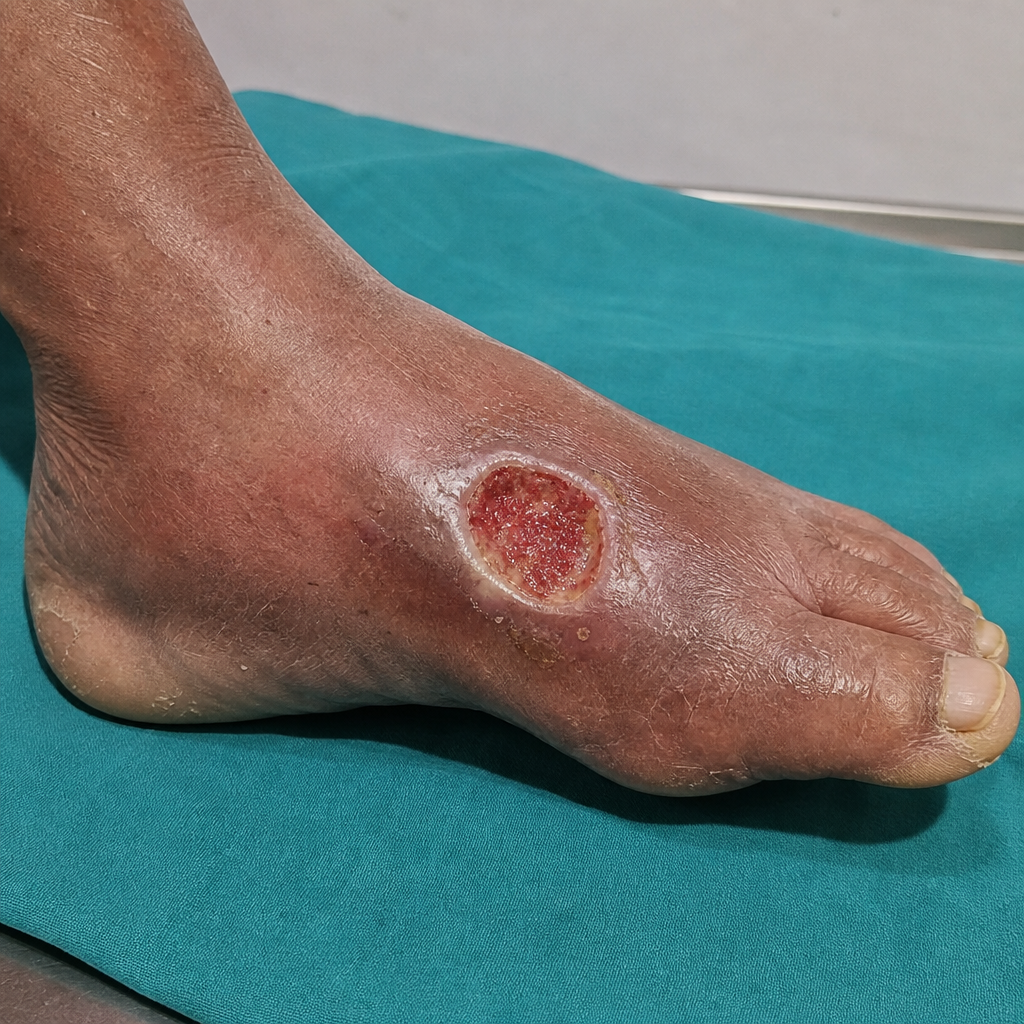
What type of ulcer is shown below?
Indication of Coronary artery bypass grafting (CABG) is:
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
