Urology — MCQs

On this page
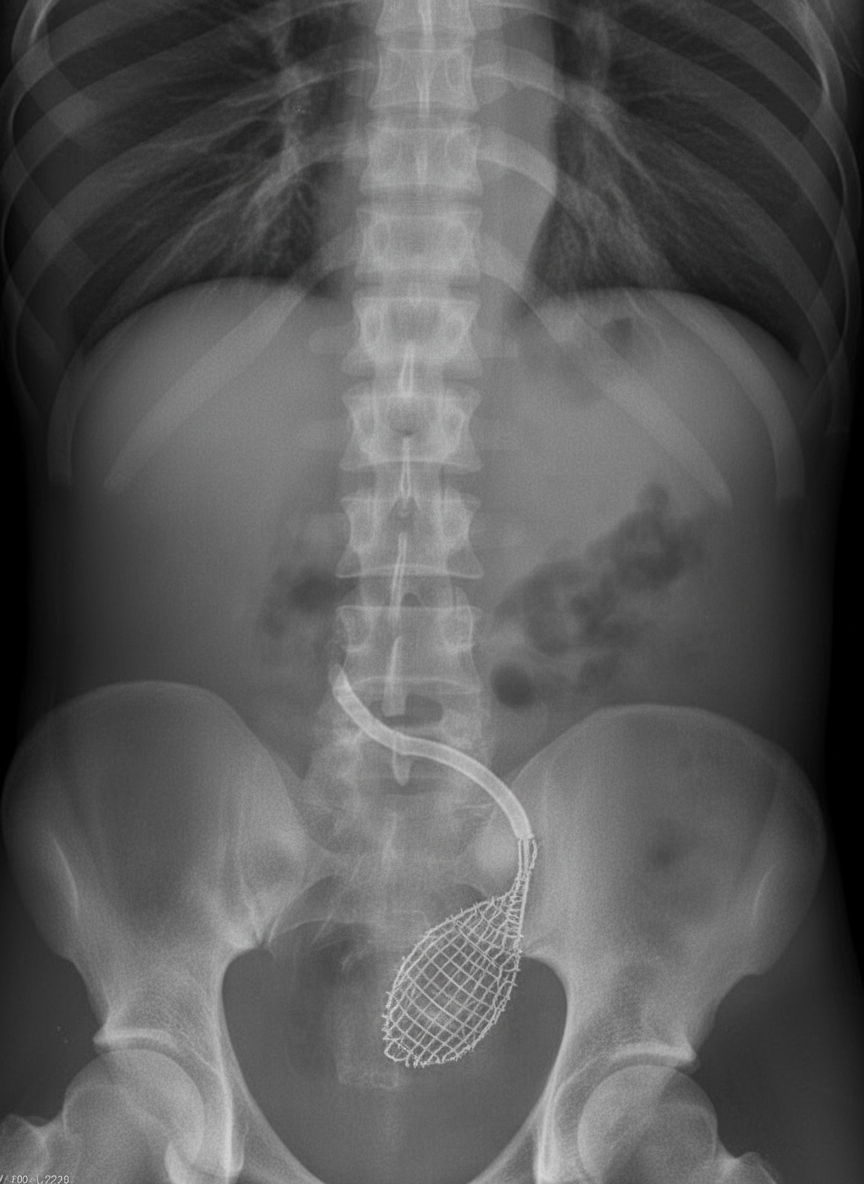
What procedure is shown in the ureter?
All of the following are seen in cystitis EXCEPT:
A patient was brought to the hospital eight hours after an injury. A few drops of blood are noted at the external urethral meatus. He has not passed urine and his bladder is palpable per abdomen. What is the probable diagnosis?
Epidermoid carcinoma of the renal pelvis is usually associated with:
Undescended testis can lead to all of the following complications except:
A 32-year-old man with a pelvic fracture presents with urinary retention and blood at the external meatus. A retrograde urethrogram shows prostatomembranous disruption. What is the most appropriate immediate treatment?
Urinary retention in a child is most commonly caused by which of the following conditions?
All of the following are true about bulbar urethral rupture, except:
A 25-year-old married male presents with infertility. He underwent retroperitoneal lymph node dissection at age 15 for embryonal carcinoma of the right testis. Semen analysis shows a quantity of 0.5 ml, no sperm, and no fructose. Testis biopsy shows normal spermatogenesis. What is the best treatment?
Which is the most common site for ectopic testis?
Practice by Chapter
Urological Anatomy
Practice Questions
Hematuria Evaluation
Practice Questions
Urinary Calculi
Practice Questions
Benign Prostatic Hyperplasia
Practice Questions
Prostate Cancer
Practice Questions
Bladder Cancer
Practice Questions
Renal Cell Carcinoma
Practice Questions
Testicular Tumors
Practice Questions
Urinary Tract Infections
Practice Questions
Urinary Incontinence
Practice Questions
Genitourinary Trauma
Practice Questions
Pediatric Urology Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
