Urology — MCQs

On this page
A 13-year-old boy presents with acute onset right scrotal pain. The pain is not relieved on elevation of the scrotum, and he has no fever or dysuria. The testis is enlarged and tender. His routine urinary examination is normal, and there is no history of trauma. Which of the following is the most appropriate management?
Which of the following is NOT a feature of ectopia vesicae?
All are features of Fournier's gangrene except?
What is the commonest endocrine tumor of the pancreas?
What is an indication for percutaneous nephrostomy?
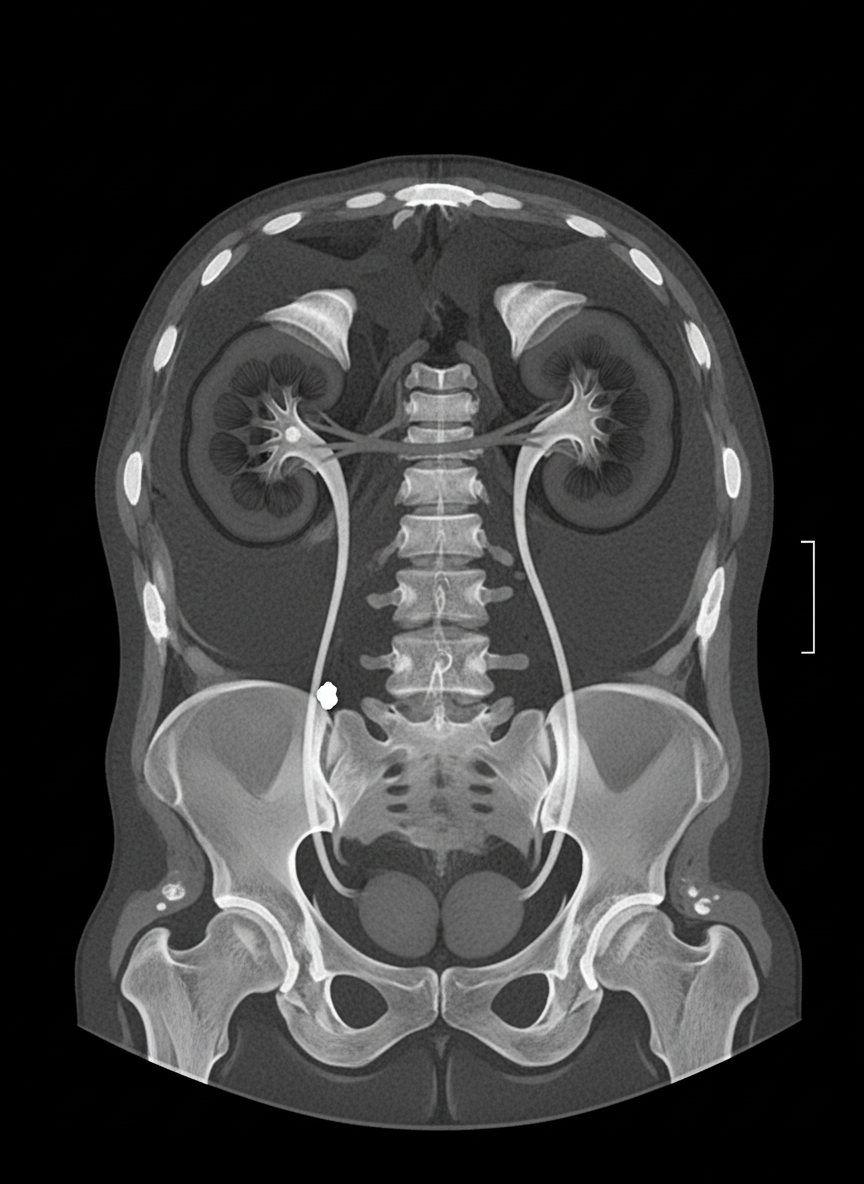
A 40-year-old male presented with severe pain in the left upper abdomen radiating to the groin. Urine routine examination shows 6-8 pus cells and 15-20 RBCs. A CT scan was performed. What is the most likely diagnosis?
During urethral catheterization in male patients, resistance is encountered at which of the following sites EXCEPT?
Which of the following are indications for percutaneous nephrostomy?
Recovery is complete in which of the following types of nerve injuries?
Which of the following is a complication of total parenteral nutrition?
Practice by Chapter
Urological Anatomy
Practice Questions
Hematuria Evaluation
Practice Questions
Urinary Calculi
Practice Questions
Benign Prostatic Hyperplasia
Practice Questions
Prostate Cancer
Practice Questions
Bladder Cancer
Practice Questions
Renal Cell Carcinoma
Practice Questions
Testicular Tumors
Practice Questions
Urinary Tract Infections
Practice Questions
Urinary Incontinence
Practice Questions
Genitourinary Trauma
Practice Questions
Pediatric Urology Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
