Urology — MCQs

On this page
In severe hypospadias, how is the possibility of an intersex problem definitively assessed?
Remnants of the primitive streak give rise to which of the following tumors?
Complications arising out of an arteriovenous fistula created for renal failure include the following EXCEPT?
Which of the following is a common retroperitoneal tumor?
Which complication following kidney transplantation is caused by Cytomegalovirus (CMV)?
Name the operation shown here.
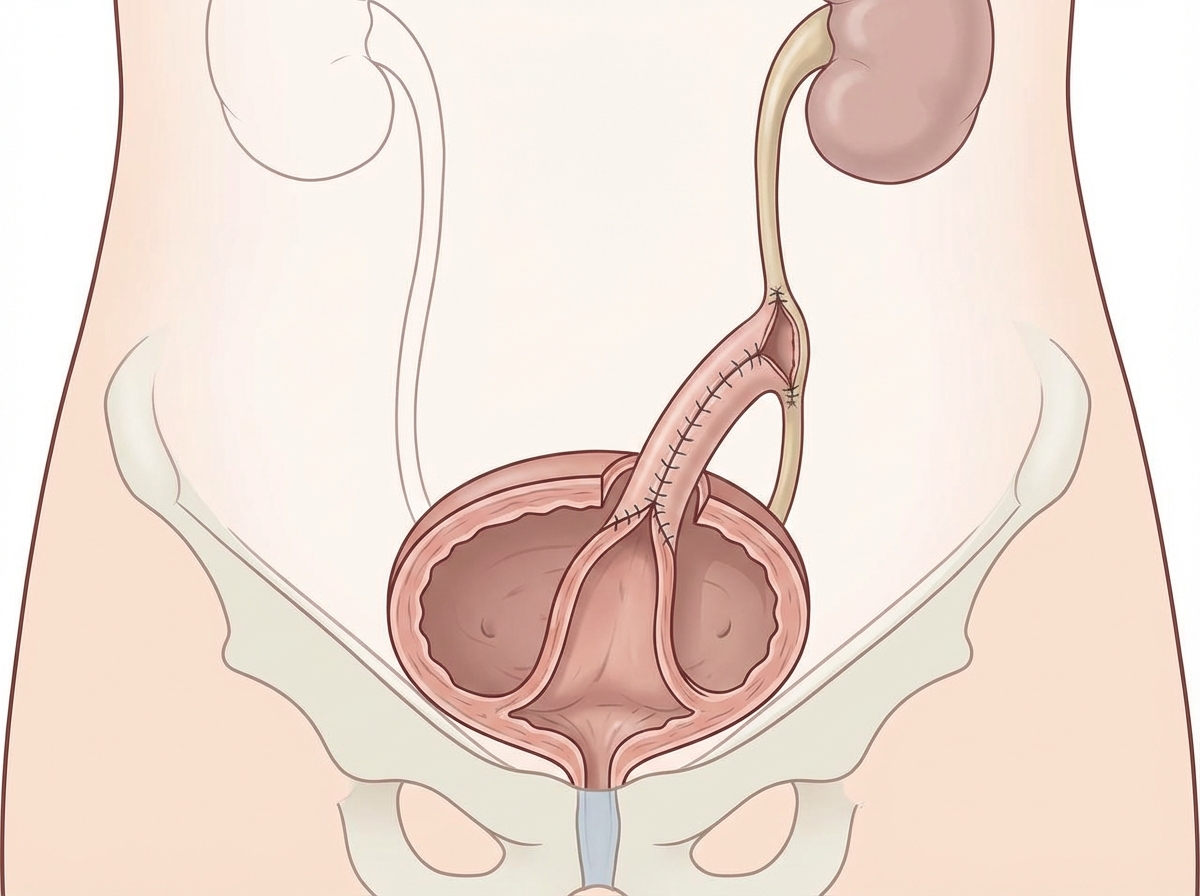
Which of the following statements regarding pain of renal and urinary tract origin is true?
What is the ideal method to remove a retained Foley's catheter if its balloon does not deflate?
During endoscopic surgery, what is the typical patient position?
Bosniak classification is used for the assessment of which of the following?
Practice by Chapter
Urological Anatomy
Practice Questions
Hematuria Evaluation
Practice Questions
Urinary Calculi
Practice Questions
Benign Prostatic Hyperplasia
Practice Questions
Prostate Cancer
Practice Questions
Bladder Cancer
Practice Questions
Renal Cell Carcinoma
Practice Questions
Testicular Tumors
Practice Questions
Urinary Tract Infections
Practice Questions
Urinary Incontinence
Practice Questions
Genitourinary Trauma
Practice Questions
Pediatric Urology Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
