Urology — MCQs

On this page
A child presents with complaints of abdominal colic and hematuria. Ultrasonography showed a renal stone 2.5 cm in diameter in the renal pelvis. What is the next step in the management of this case?
All of the following are true about prostate-specific antigen except?
What is the standard treatment for seminoma?
Which of the following is the most common cause of delayed urinary tract obstructive symptoms after TURP?
Carcinoma of the testis, to which anatomical location does lymphatic metastasis typically occur first?
A patient with a suspected pelvic fracture presents with urethral bleeding and inability to pass urine. What is the immediate management step?
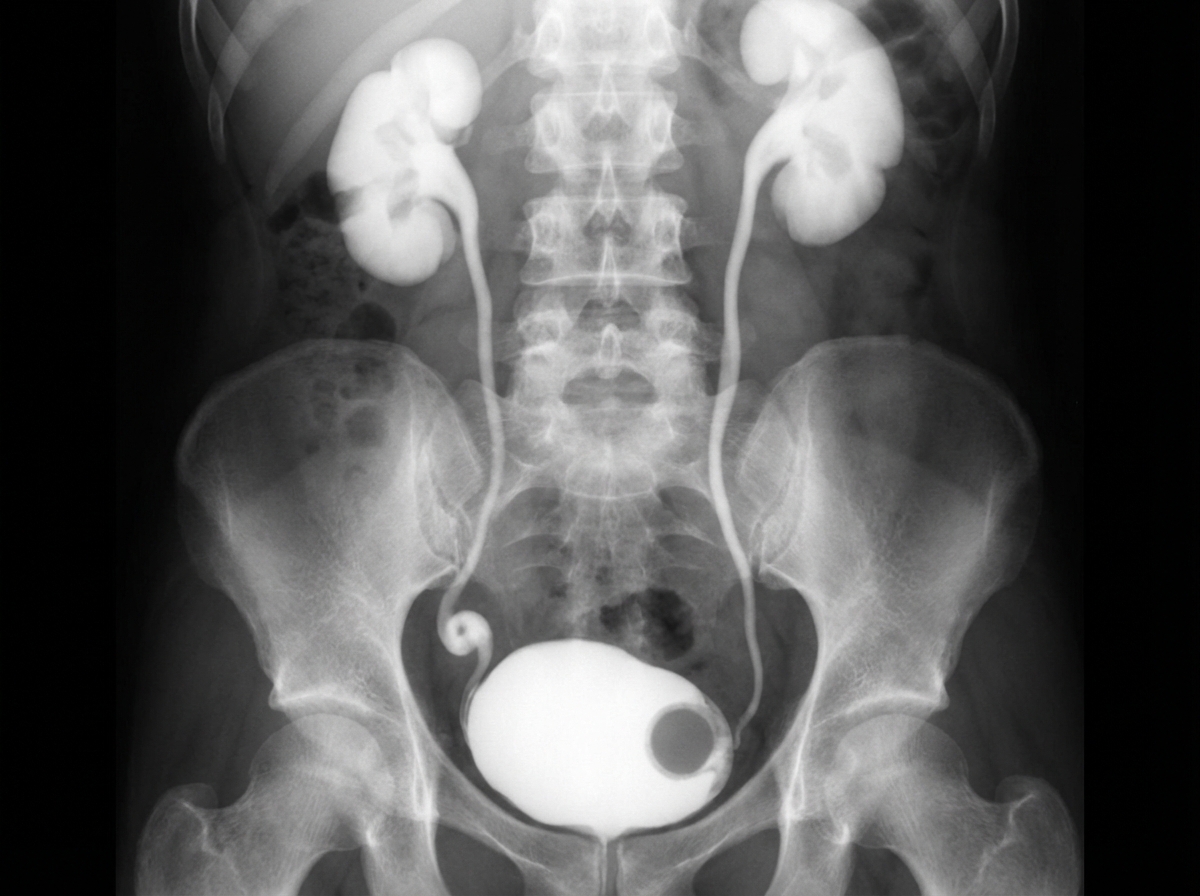
A 10-year-old girl was evaluated for recurrent UTI and dysuria. An IVP finding is shown. What is the preferred treatment option for this case?
Operative management of varicocele is indicated in all of the following conditions except?
Which of the following is an alkaline type of renal calculi?
A patient presents with urethral bleeding and perineal swelling following a straddle injury, indicative of a ruptured bulbar urethra. Which of the following statements regarding his management is FALSE?
Practice by Chapter
Urological Anatomy
Practice Questions
Hematuria Evaluation
Practice Questions
Urinary Calculi
Practice Questions
Benign Prostatic Hyperplasia
Practice Questions
Prostate Cancer
Practice Questions
Bladder Cancer
Practice Questions
Renal Cell Carcinoma
Practice Questions
Testicular Tumors
Practice Questions
Urinary Tract Infections
Practice Questions
Urinary Incontinence
Practice Questions
Genitourinary Trauma
Practice Questions
Pediatric Urology Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
