Urology — MCQs

On this page
What is the commonest cause of ureteric injury during surgical operation?
According to the classification of renal injuries, which grade is assigned to a laceration more than 1 cm deep without extension into the renal pelvis or collecting system?
A 23-year-old male presented with fever, chills, and back pain. He also complained of increased frequency of voiding. Ultrasonography revealed bladder stones. All of the following are true about bladder stones, EXCEPT:
A male has a history of bilateral undescended testes. What is the most likely consequence?
Which of the following statements about hypospadias is/are true?
What is the recommended method for collecting samples for the diagnosis of renal tuberculosis?
The Hunt-Hess scale is used for the grading of which condition?
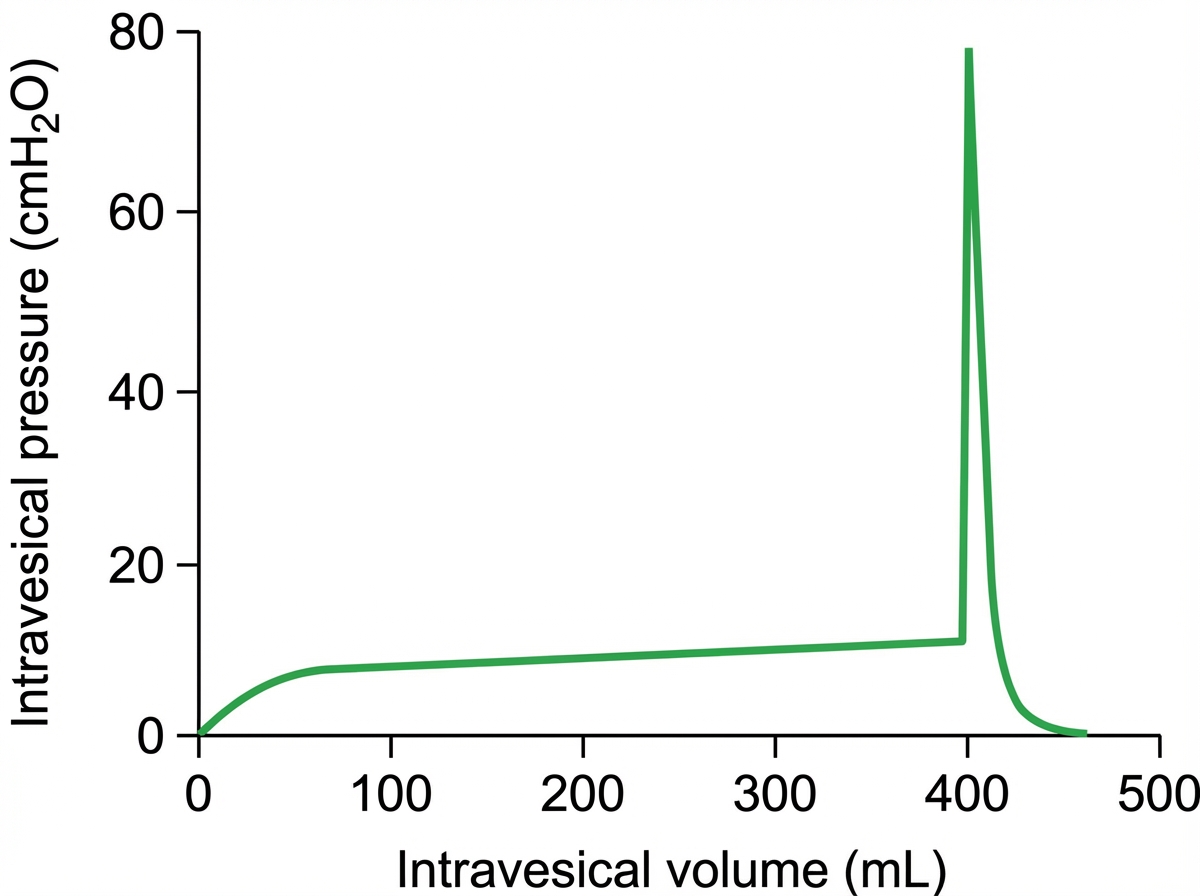
The graph shown in the illustration is known as:
What is the best treatment for Grade I benign prostate with outflow obstruction?
Scrambled egg appearance is seen in which of the following conditions?
Practice by Chapter
Urological Anatomy
Practice Questions
Hematuria Evaluation
Practice Questions
Urinary Calculi
Practice Questions
Benign Prostatic Hyperplasia
Practice Questions
Prostate Cancer
Practice Questions
Bladder Cancer
Practice Questions
Renal Cell Carcinoma
Practice Questions
Testicular Tumors
Practice Questions
Urinary Tract Infections
Practice Questions
Urinary Incontinence
Practice Questions
Genitourinary Trauma
Practice Questions
Pediatric Urology Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
