Urology — MCQs

On this page
Which among the following is the most important preventive strategy of penile cancer?
Which of the following is a key differentiator between functional gastrointestinal disorders and organic gastrointestinal disorders?
What is true about undescended testes?
Cabana procedure is done in which of the following conditions?
Which of the following statements is NOT true regarding undescended testes?
A young man presents with primary infertility, and his semen analysis reveals low volume, fructose-negative ejaculate with azoospermia. Which of the following is the most useful imaging modality to evaluate the cause of his infertility?
What investigation is done to differentiate between stress incontinence and detrusor instability?
Which type of urinary stone is resistant to lithotripsy?
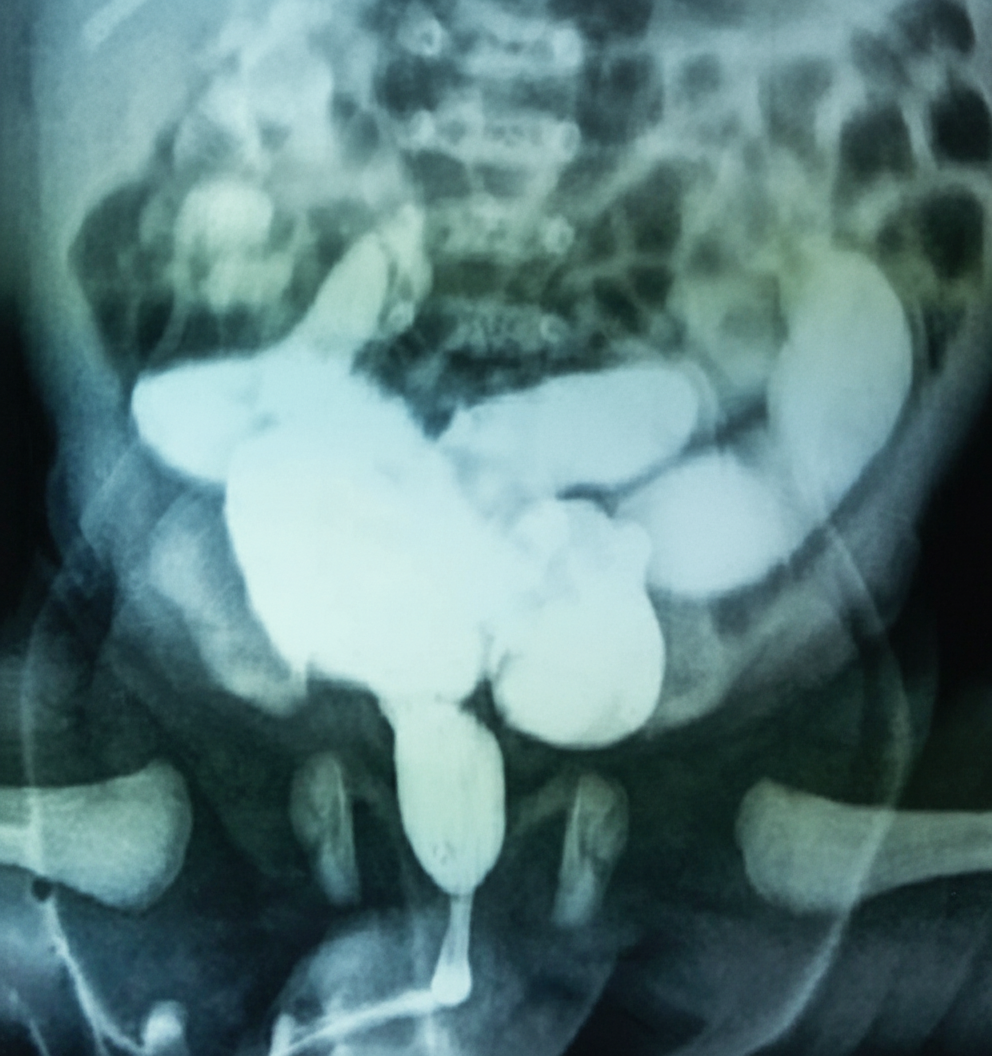
Physical examination of a neonate reveals a distended bladder and palpable kidneys. The infant produces a weak urinary stream. A voiding cystourethrogram is shown. He appears to be otherwise normal. Which of the following is the most likely diagnosis?
Prostate cancer is best diagnosed by?
Practice by Chapter
Urological Anatomy
Practice Questions
Hematuria Evaluation
Practice Questions
Urinary Calculi
Practice Questions
Benign Prostatic Hyperplasia
Practice Questions
Prostate Cancer
Practice Questions
Bladder Cancer
Practice Questions
Renal Cell Carcinoma
Practice Questions
Testicular Tumors
Practice Questions
Urinary Tract Infections
Practice Questions
Urinary Incontinence
Practice Questions
Genitourinary Trauma
Practice Questions
Pediatric Urology Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
