Urology — MCQs

On this page
An elderly male presents with one episode of gross hematuria. Which of the following investigations is NOT recommended for this patient?
Which of the following statements regarding ureteric stones is false?
Sterile pyuria is seen in which of the following conditions?
Fir tree appearance of the bladder is seen in which condition?
What is the investigation of choice in ureteric colic?
A 65-year-old female presents with recurrent episodes of gross painless hematuria. What is the most common cause of gross painless hematuria?
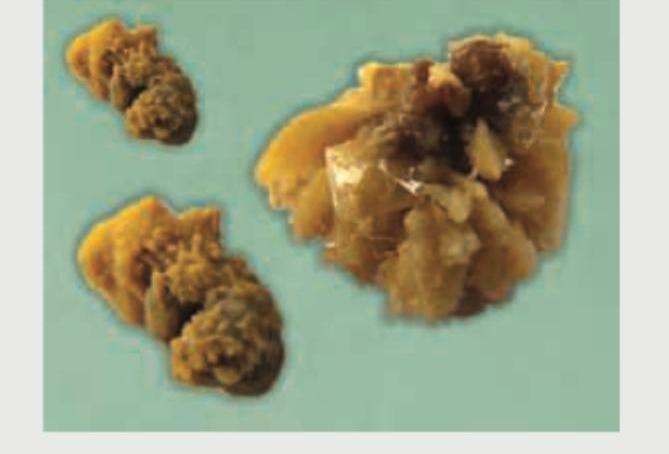
What is the composition of this stone?
MEN 2A is associated with the following conditions, except:
A 60-year-old male presents with a poor stream of urine, a post-void residual urine volume of 400 mL, bilateral hydronephrosis, and a prostate weighing 70 g. His urea is 120 mg/dL and creatinine is 3.5 mg/dL. What is the ideal next immediate step?
What is the treatment of choice for ureteric colic?
Practice by Chapter
Urological Anatomy
Practice Questions
Hematuria Evaluation
Practice Questions
Urinary Calculi
Practice Questions
Benign Prostatic Hyperplasia
Practice Questions
Prostate Cancer
Practice Questions
Bladder Cancer
Practice Questions
Renal Cell Carcinoma
Practice Questions
Testicular Tumors
Practice Questions
Urinary Tract Infections
Practice Questions
Urinary Incontinence
Practice Questions
Genitourinary Trauma
Practice Questions
Pediatric Urology Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
