Urology — MCQs

On this page
What is the most common site for extramammary Paget's disease?
Regarding ectopia vesicae, which of the following is true EXCEPT?
What is the first-line treatment for overactive bladder?
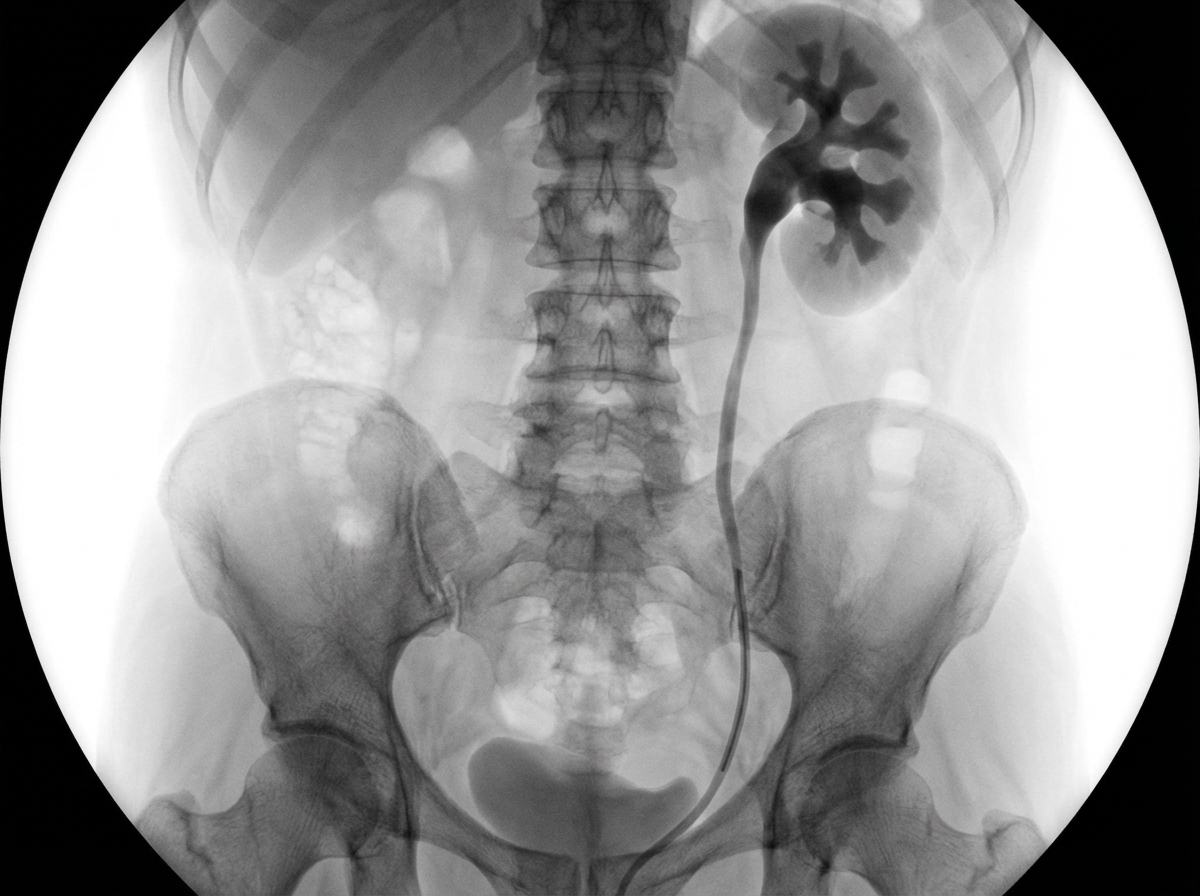
What is this study?
Peyronie's disease affects which of the following structures?
A 55-year-old smoker presents with a history of five episodes of macroscopic hematuria, each lasting for about 4-5 days over the past five years. Which of the following investigations should be performed to evaluate the suspected diagnosis?
Which of the following statements about varicocele is false?
What is the most appropriate treatment for acute paronychia?
A 68-year-old male with hypertension presents for annual examination. On review of systems, he reports urinary hesitancy and nocturia. His examination reveals a nontender but enlarged prostate without nodules. His blood pressure logs and clinic readings show average values of 150/80 mm Hg. Which medication offer treatment of hypertension and prostatic symptoms?
Squamous cell carcinoma of the urinary bladder is associated with which of the following?
Practice by Chapter
Urological Anatomy
Practice Questions
Hematuria Evaluation
Practice Questions
Urinary Calculi
Practice Questions
Benign Prostatic Hyperplasia
Practice Questions
Prostate Cancer
Practice Questions
Bladder Cancer
Practice Questions
Renal Cell Carcinoma
Practice Questions
Testicular Tumors
Practice Questions
Urinary Tract Infections
Practice Questions
Urinary Incontinence
Practice Questions
Genitourinary Trauma
Practice Questions
Pediatric Urology Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
