Trauma — MCQs

On this page
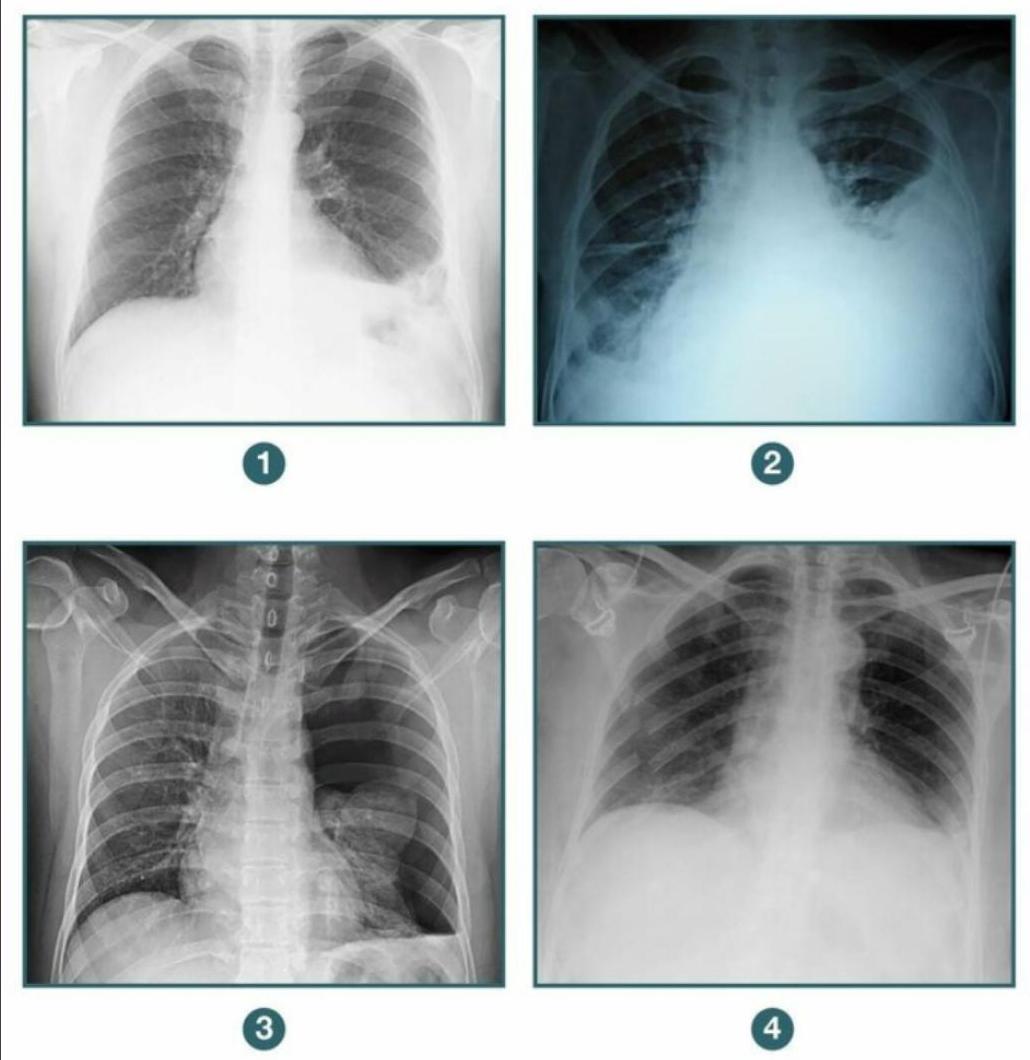
A patient presents to the casualty following blunt trauma to the chest. A chest X-ray was done. Among the following radiographs, in which case would you further evaluate the patient before putting a chest tube? 1. Diaphragmatic hernia 2. Hemothorax 3. Pneumothorax 4. Flail chest
A patient presents with pneumothorax on chest x-ray. Which of the following is NOT a boundary of the triangle of safety for intercostal chest drain (ICD) insertion?
What is the correct sequence of management in a patient who presents to the casualty with an RTA? 1. Cervical spine stabilization 2. Intubation 3. IV cannulation 4. CECT
Which of these is the most life-threatening injury that can be identified by assessing the breathing component of the patient?
What should be done as an immediate measure for ongoing bleeding in a patient with pelvic bone fracture?
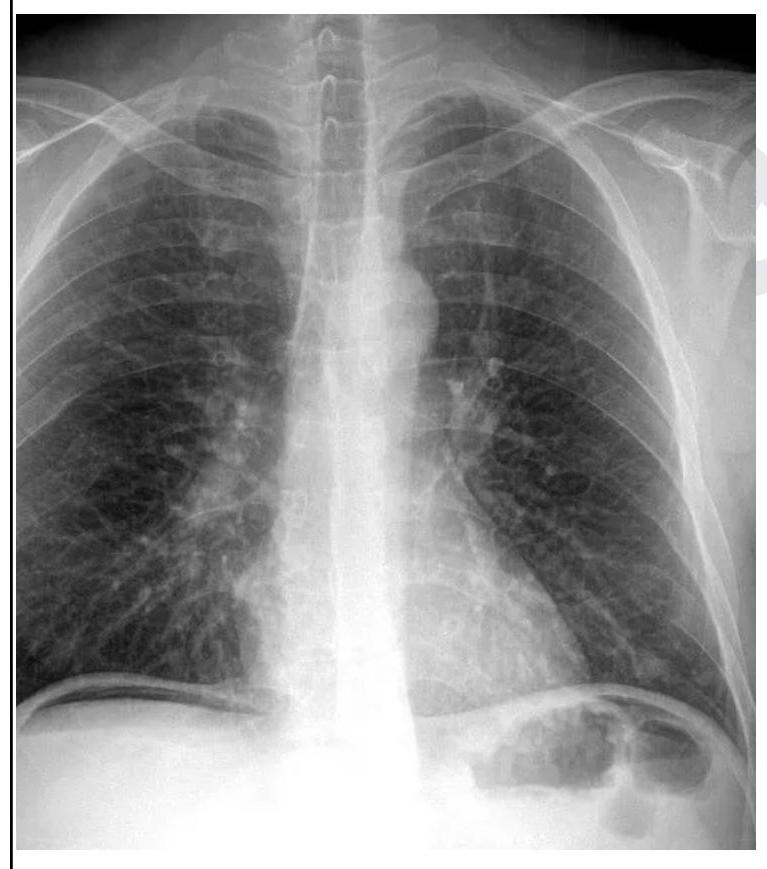
A 26 year old male patient was brought to the emergency department with abdominal pain and obstipation for 3 days. He gives a history of bull gore to the abdomen 3 days back. His chest X-ray is given below. What is the probable diagnosis?
Which of the following findings appear late in compartment syndrome?
A 36-year-old woman is brought to the emergency department 20 minutes after being involved in a high-speed motor vehicle collision. On arrival, she is unconscious. Her pulse is 140/min, respirations are 12/min and shallow, and blood pressure is 76/55 mm Hg. 0.9% saline infusion is begun. A focused assessment with sonography shows blood in the left upper quadrant of the abdomen. Her hemoglobin concentration is 7.6 g/dL and hematocrit is 22%. The surgeon decided to move the patient to the operating room for an emergent explorative laparotomy. Packed red blood cell transfusion is ordered prior to surgery. However, a friend of the patient asks for the transfusion to be held as the patient is a Jehovah's Witness. The patient has no advance directive and there is no documentation showing her refusal of blood transfusions. The patient's husband and children cannot be contacted. Which of the following is the most appropriate next best step in management?
A 24-year-old man is rushed to the emergency room after he was involved in a motor vehicle accident. He says that he is having difficulty breathing and has right-sided chest pain, which he describes as 8/10, sharp in character, and worse with deep inspiration. His vitals are: blood pressure 90/65 mm Hg, respiratory rate 30/min, pulse 120/min, temperature 37.2°C (99.0°F). On physical examination, patient is alert and oriented but in severe distress. There are multiple bruises over the anterior chest wall. There is also significant jugular venous distention and the presence of subcutaneous emphysema at the base of the neck. There is an absence of breath sounds on the right and hyperresonance to percussion. A bedside chest radiograph shows evidence of a collapsed right lung with a depressed right hemidiaphragm and tracheal deviation to the left. Which of the following findings is the strongest indicator of cardiogenic shock in this patient?
A 56-year-old man is brought to the emergency department 30 minutes after falling from a height of 3 feet onto a sharp metal fence pole. He is unconscious. Physical examination shows a wound on the upper margin of the right clavicle in the parasternal line that is 3-cm-deep. Which of the following is the most likely result of this patient's injury?
Practice by Chapter
Initial Assessment of Trauma Patient
Practice Questions
Advanced Trauma Life Support (ATLS) Principles
Practice Questions
Chest Trauma
Practice Questions
Abdominal Trauma
Practice Questions
Head Trauma
Practice Questions
Spinal Trauma
Practice Questions
Extremity Trauma
Practice Questions
Vascular Trauma
Practice Questions
Genitourinary Trauma
Practice Questions
Burns Management
Practice Questions
Mass Casualty Management
Practice Questions
Damage Control Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
