Trauma — MCQs

On this page
A 40-year-old male presents to the emergency department with severe respiratory distress, BP: 70/59 mmHg, tracheal deviation to the right, distended neck veins, and absent breath sounds on the left side. These findings are suggestive of a tension pneumothorax. What is the most appropriate immediate next step in management?
Which of the following is correct about the maneuver being performed in the image?
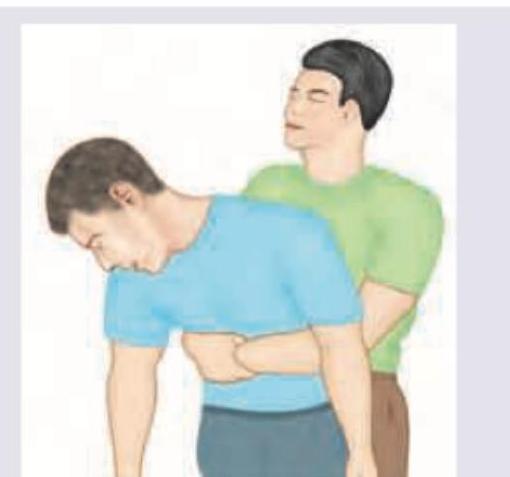
All are true about the procedure shown below except: (Recent NEET Pattern 2016-17)
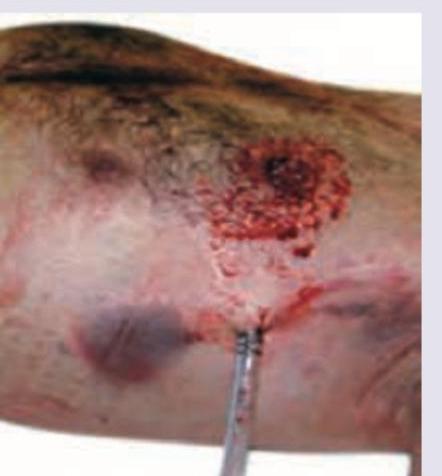
A splenorenal shunt procedure may be required for treatment of:
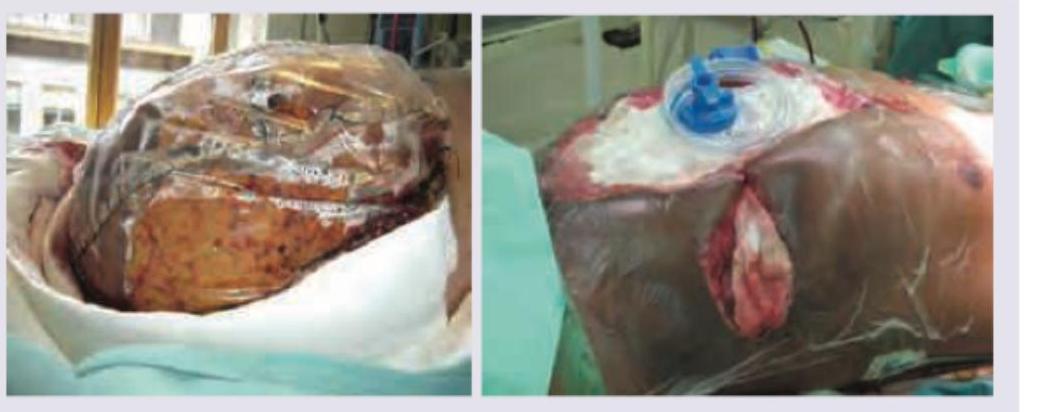
A 30-year-old young male who met with a road traffic accident was brought to trauma center. On admission his BP was 90/50 mmHg, pulse rate is 150/min, SpO₂ is 80% and GCS is 8. He has multiple injuries and FAST reveals presence of blood in all quadrants. He was operated upon and his postoperative pictures are given below. Which of the following options best describe these pictures? (AIIMS Nov 2016)
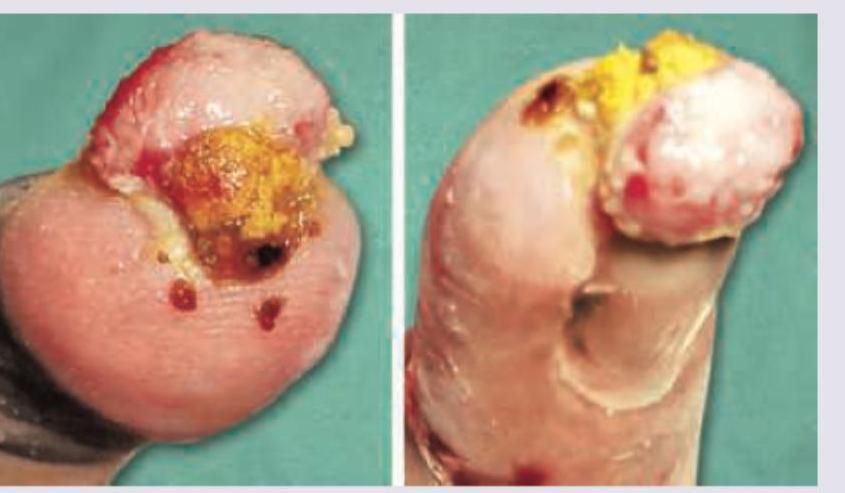
A 30-year-old construction worker had a partial traumatic nail avulsion. 3 weeks later he presents with the presentation shown below. What is the diagnosis?
Which is the best method to secure airway and administer oxygen in case of burns shown below?
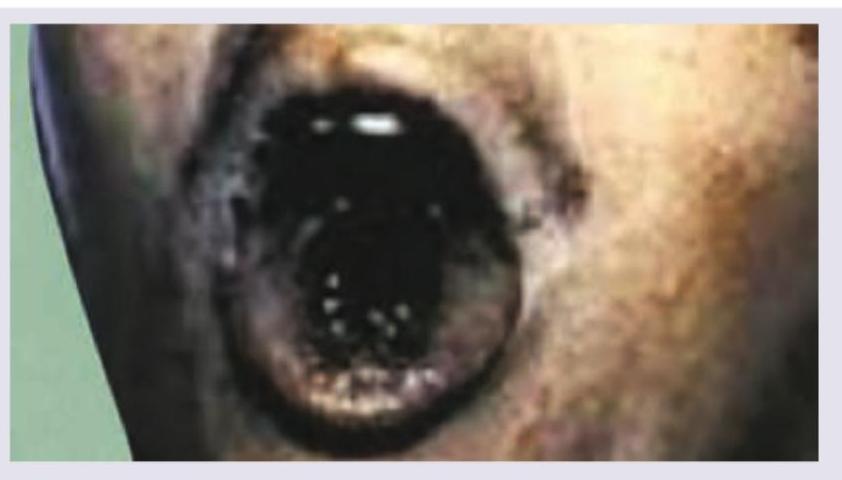
A soldier was airlifted from Siachen glacier after being trapped in an avalanche. All of the following are done in this condition except:
A mixed martial arts boxer lost his match by knockout. One week later, he is having daily headaches, vomiting and disorientation. On arrival in casualty $\mathrm{GCS}=7$ and fundus shows presence of papilledema. Urgent CT scan head shows?
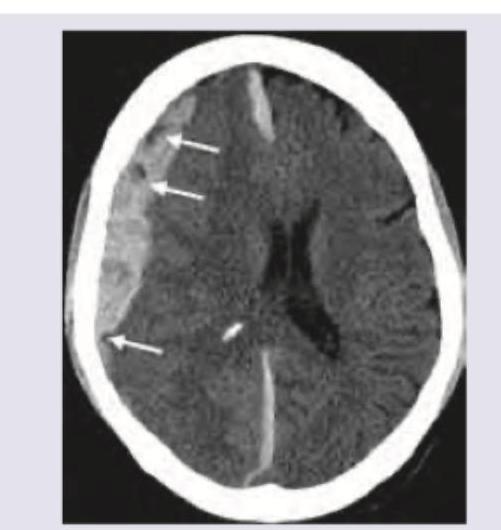
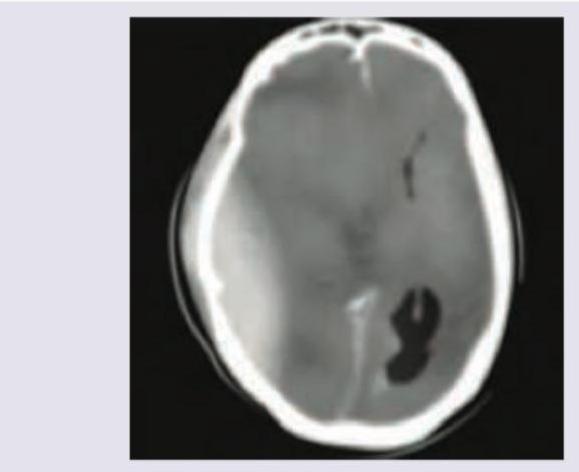
A 25-year-old patient presents in coma with GCS of 5 and extensor posturing after a bike accident. CT head was performed. Which of the following will be the best management of the patient?
Practice by Chapter
Initial Assessment of Trauma Patient
Practice Questions
Advanced Trauma Life Support (ATLS) Principles
Practice Questions
Chest Trauma
Practice Questions
Abdominal Trauma
Practice Questions
Head Trauma
Practice Questions
Spinal Trauma
Practice Questions
Extremity Trauma
Practice Questions
Vascular Trauma
Practice Questions
Genitourinary Trauma
Practice Questions
Burns Management
Practice Questions
Mass Casualty Management
Practice Questions
Damage Control Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
