Trauma — MCQs

On this page
If a fracture of the mandible occurs distal to a lost tooth, what is the treatment of choice?
A young male presented with dyspnea, bleeding, and petechial hemorrhage in the chest 2 days following a fracture of the shaft of the right femur. What is the most likely cause?
What is the best management of a contaminated wound with necrotic material?
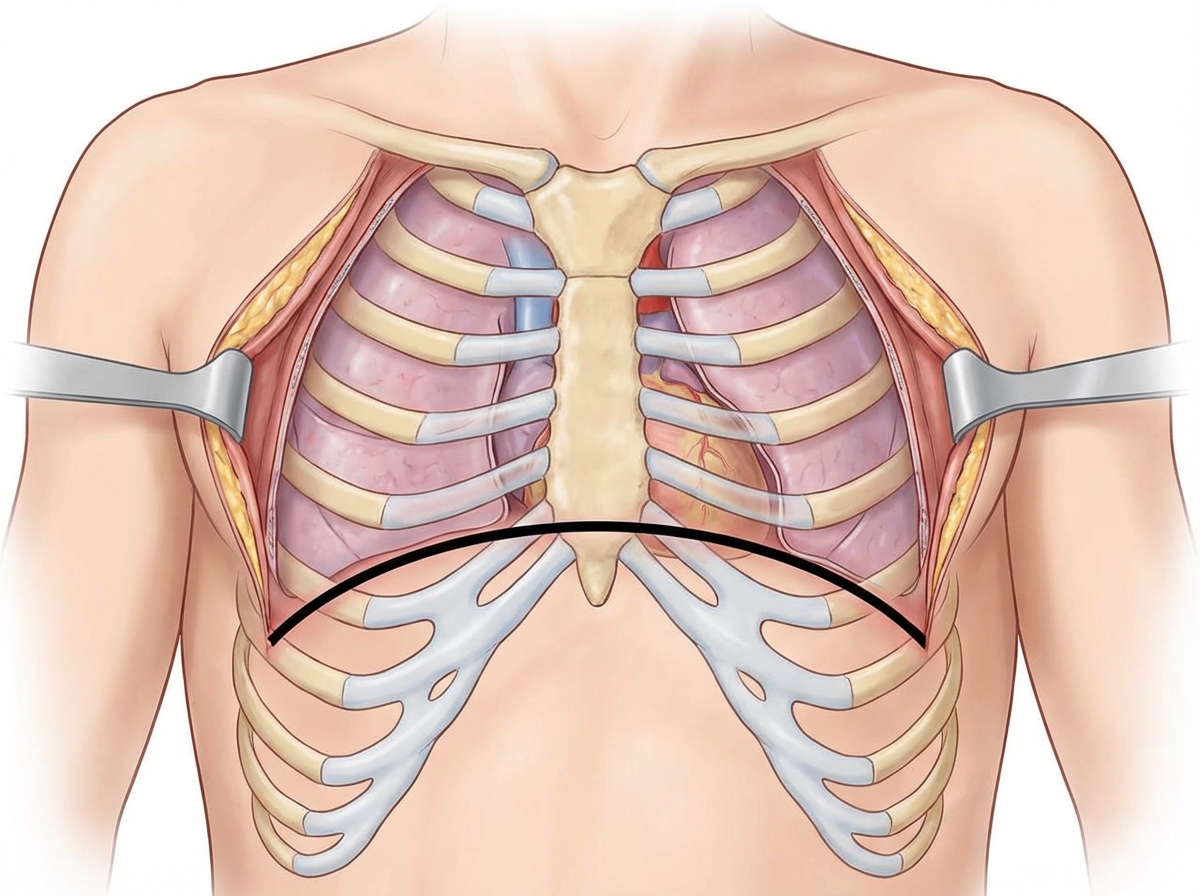
What is the name of the emergency thoracotomy procedure illustrated?
A 70 kg female has 50% burns and an inhalation burn injury. What is the fluid requirement in the first 8 hours according to the Parkland formula?
A patient presents to the emergency department with a stab injury to the left side of the abdomen. She is hemodynamically stable, and a contrast-enhanced CT scan reveals a laceration in the spleen. Laparoscopy is planned; however, the patient's pO2 suddenly drops as soon as pneumoperitoneum is created. What is the most likely cause?
A male patient is admitted following a fall from height. On arrival his Glasgow Coma Scale score is 5/15 and he is therefore intubated. During primary resuscitation, a chest film is taken which shows a widened mediastinum and right-sided deviation of the trachea. What is the most likely diagnosis?
A man presented with fractures of 4th to 10th ribs and respiratory distress after a Road Traffic Accident. He is diagnosed to have flail chest. What is the recommended management?
What is the management of an open wound seen 12 hours after the injury?
A patient admitted to the casualty department after a road traffic accident shows bruising behind the mastoid. This sign is known as?
Practice by Chapter
Initial Assessment of Trauma Patient
Practice Questions
Advanced Trauma Life Support (ATLS) Principles
Practice Questions
Chest Trauma
Practice Questions
Abdominal Trauma
Practice Questions
Head Trauma
Practice Questions
Spinal Trauma
Practice Questions
Extremity Trauma
Practice Questions
Vascular Trauma
Practice Questions
Genitourinary Trauma
Practice Questions
Burns Management
Practice Questions
Mass Casualty Management
Practice Questions
Damage Control Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
