Trauma — MCQs

On this page
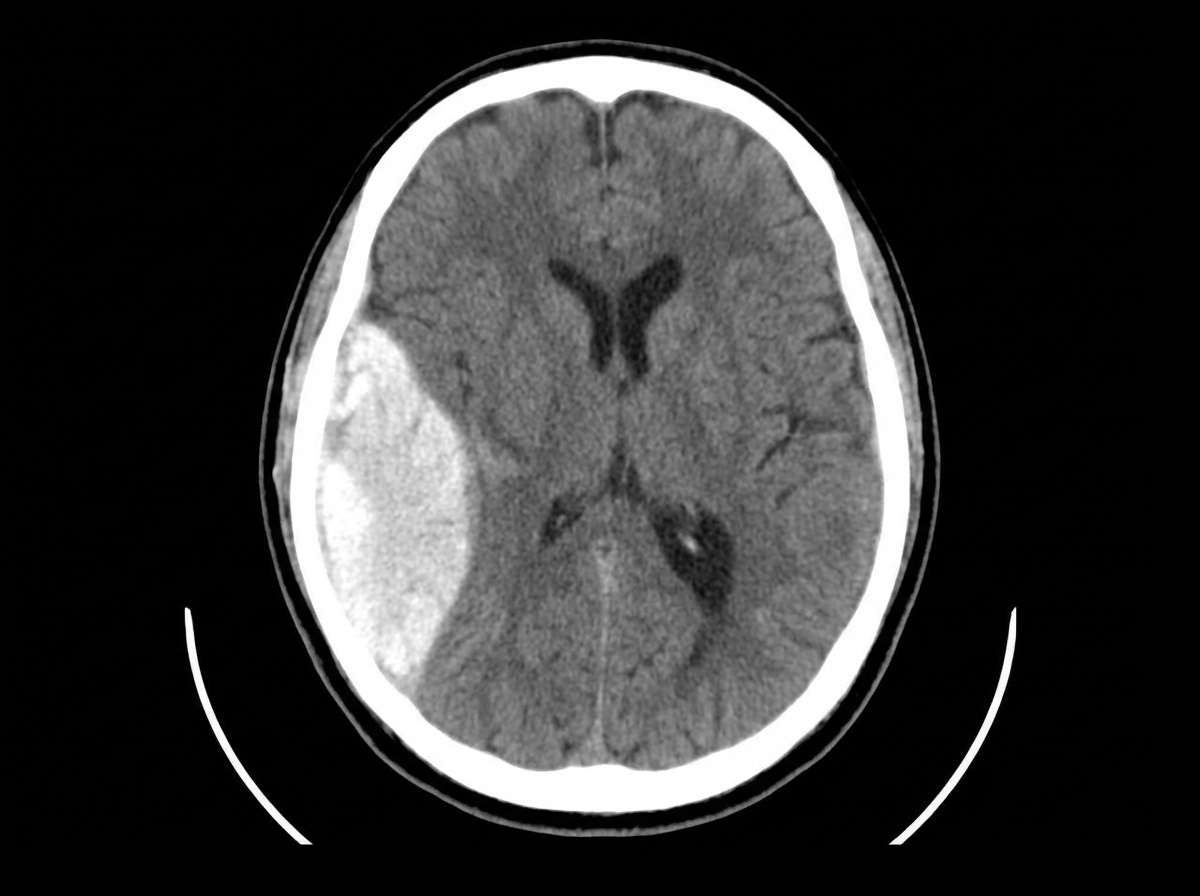
A 30-year-old patient with a head injury presented to the emergency department. NCCT findings are provided. All of the following are true about this condition except:
A 50-year-old male presents with severe vomiting and retching accompanied by sharp substernal pain. Four hours later, a chest X-ray reveals air density outlining the left descending aorta. What is the optimum strategy for his care?
After an open injury, what is the optimum time for nerve suture?
In burns, when does pus formation typically occur?
Which of the following are causes of secondary brain injury?
A 50-year-old man with a history of being a Jehovah's Witness, who refuses blood transfusions, is brought to the emergency department after a motor vehicle accident. He presents with signs of shock (hypotension, tachycardia) and abdominal ultrasound reveals free fluid, necessitating an emergency laparotomy. If the patient requires blood during the operation, what is the surgeon's best course of action?
Kernohan's notch is seen in which organ injury?
What is the correct method for examining the spine of a polytrauma patient?
A 40-year-old man sustained injuries to the liver, gallbladder, small intestine, and colon from gunshot wounds. At the time of surgery, a cholecystostomy was placed in the injured gallbladder to expedite operative management. Four weeks later, the patient is doing well. Which is the next step in management?
A 25-year-old female was involved in a car accident. Her Glasgow Coma Scale (GCS) was normal. On examination, her heart rate was 150/min, blood pressure was 90/60 mm Hg, and respiratory rate was 20/min. Her jugular venous pressure (JVP) was raised, her abdomen was not tender, and she had ecchymosis over her anterior chest. Breath sounds were absent on one side. What is the most appropriate diagnosis?
Practice by Chapter
Initial Assessment of Trauma Patient
Practice Questions
Advanced Trauma Life Support (ATLS) Principles
Practice Questions
Chest Trauma
Practice Questions
Abdominal Trauma
Practice Questions
Head Trauma
Practice Questions
Spinal Trauma
Practice Questions
Extremity Trauma
Practice Questions
Vascular Trauma
Practice Questions
Genitourinary Trauma
Practice Questions
Burns Management
Practice Questions
Mass Casualty Management
Practice Questions
Damage Control Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
