Trauma — MCQs

On this page
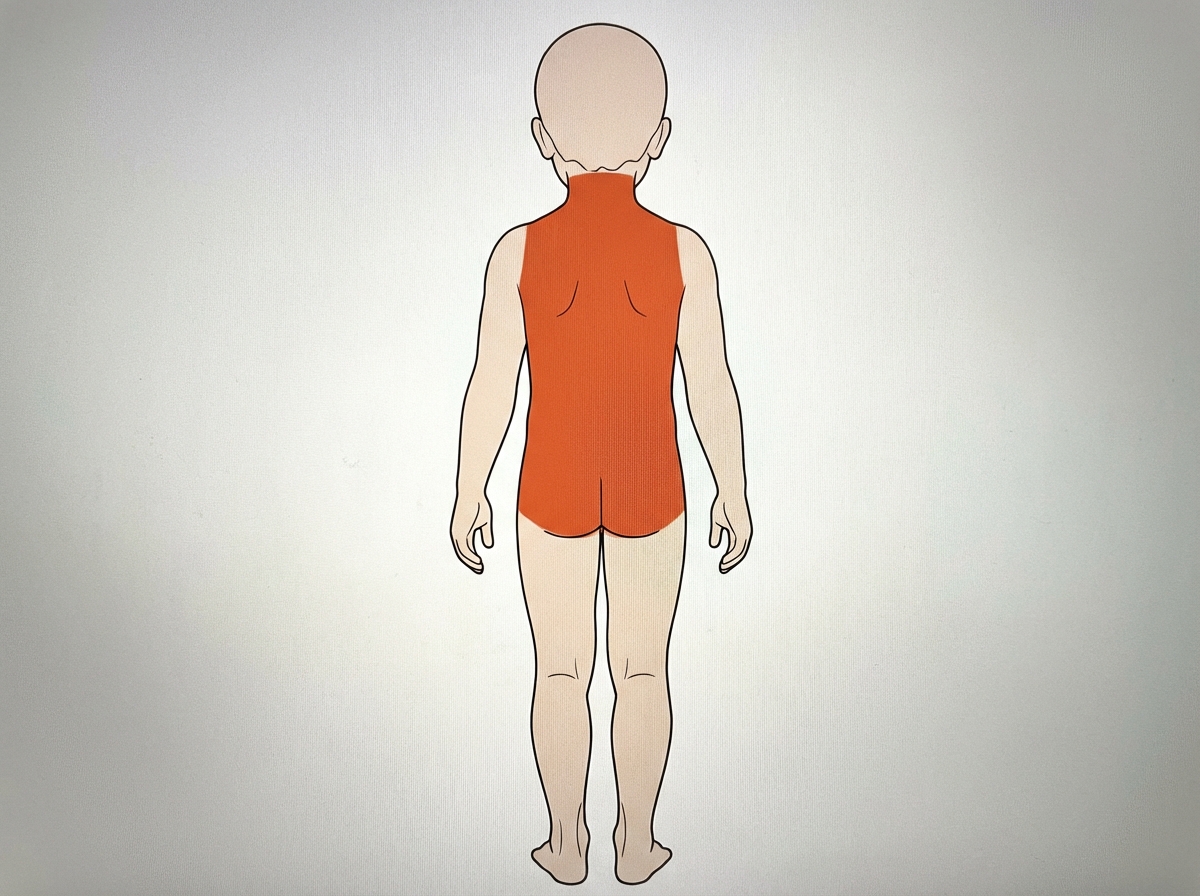
A 10-year-old boy sustained a burn injury on his back. What percentage of his Total Body Surface Area (TBSA) does this injury represent?
A 40-year-old man with severe maxillofacial trauma following a motor vehicle accident presents to the emergency department one hour after the incident. His vital signs are: Pulse rate 120/min, BP 100/70 mm Hg, and SpO2 80% on oxygen. What is the most appropriate immediate management?
A patient with head injury opens eyes on painful stimulus, uses inappropriate words and localizes pain. What is his GCS score?
A 42-year-old man presents with fractures of the left tenth, eleventh, and twelfth ribs and left tibia and fibula fractures following trauma. His vital signs are: blood pressure 120/90 mm Hg, pulse rate 100 bpm, and respiration rate 24 breaths per minute. He has hematuria and left flank pain. Intravenous pyelography shows no excretion from the left kidney but normal excretion from the right. What is the next step in management?
A patient with spine, chest, and abdominal injury in a road traffic accident developed hypotension and bradycardia. What is the most likely reason?
A patient presents with irritability and altered sensorium 4 weeks after head trauma. What is the most common cause of these symptoms?
A fracture mandible should be immobilized for an average of how many weeks?
Which is the most common neurofibroma in the posterior mediastinum?
Which of the following wiring is indicated in case of symphysis fracture of the mandible?
A 24-year-old male, a victim of a road traffic accident, is brought to the casualty department with breathlessness and tachypnea. Examination reveals tracheal deviation to the left and a hyperresonant sound on the right side of the chest. How should this patient be managed?
Practice by Chapter
Initial Assessment of Trauma Patient
Practice Questions
Advanced Trauma Life Support (ATLS) Principles
Practice Questions
Chest Trauma
Practice Questions
Abdominal Trauma
Practice Questions
Head Trauma
Practice Questions
Spinal Trauma
Practice Questions
Extremity Trauma
Practice Questions
Vascular Trauma
Practice Questions
Genitourinary Trauma
Practice Questions
Burns Management
Practice Questions
Mass Casualty Management
Practice Questions
Damage Control Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
