Trauma — MCQs

On this page
Which of the following is not a component of the crush syndrome?
Decision regarding surgery in a case of hemothorax due to blunt trauma chest should be based on which of the following?
Hypertonic saline is not indicated in which of the following conditions?
Diplopia is most common with which of the following injuries?
A 40-year-old woman was involved in a car crash and was unconscious for 5 minutes. X-ray revealed a depressed fracture in the frontal region. Which of the following statements is true of skull fracture?
A 40-year-old construction worker is pulled from the rubble after a building collapse, sustaining a comminuted fracture of the right tibia and fibula in his right lower leg. The dorsal pedis and posterior tibial pulses are palpable. The patient reports severe pain, which is worsened with dorsiflexion of the foot, and the calf feels tense. What is the appropriate next step?
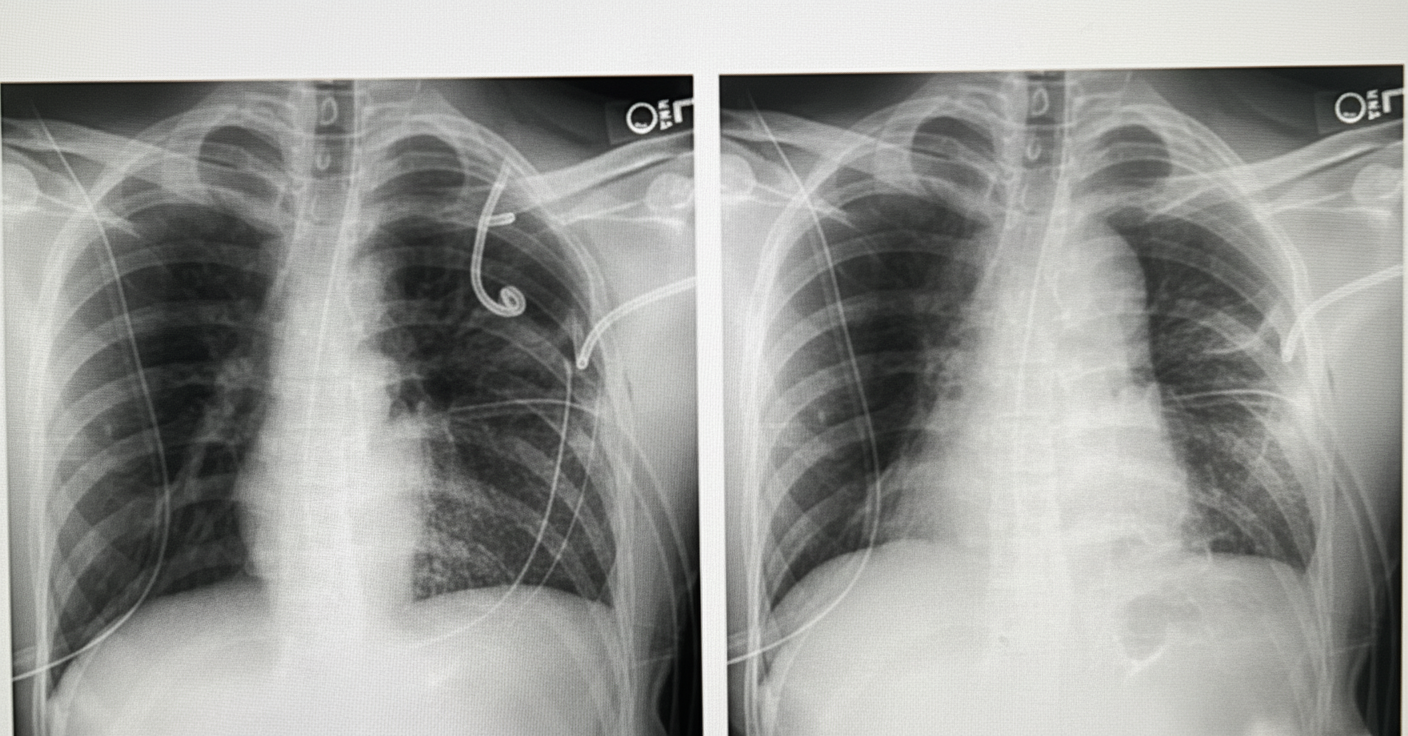
A 50-year-old patient presents to the ER with a history of a road traffic accident. The patient is unconscious. e-FAST revealed fluid in the pelvis. Chest X-ray is provided. What is the most likely diagnosis?
In an injured patient with hypovolemia, which parameter primarily guides intravenous fluid administration?
Capillary fill is fast in which of the following types of shock?
Damage control surgery is defined as:
Practice by Chapter
Initial Assessment of Trauma Patient
Practice Questions
Advanced Trauma Life Support (ATLS) Principles
Practice Questions
Chest Trauma
Practice Questions
Abdominal Trauma
Practice Questions
Head Trauma
Practice Questions
Spinal Trauma
Practice Questions
Extremity Trauma
Practice Questions
Vascular Trauma
Practice Questions
Genitourinary Trauma
Practice Questions
Burns Management
Practice Questions
Mass Casualty Management
Practice Questions
Damage Control Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
