Trauma — MCQs

On this page
What is the most common origin of cerebral metastases?
In order to expose the coeliac axis, left renal artery, superior mesenteric artery, and abdominal aorta in a case of trauma, which of the following procedures is performed?
A blow-out fracture of the zygomatic arch can cause which of the following?
Which of the following is NOT true about mandible fractures?
What is the most common site for an extradural hematoma?
Which of the following statements regarding the management of burns is incorrect?
A 25-year-old college student sustains injuries in a road traffic accident and is brought to the casualty department. The patient presents with marked abdominal distension, a pulse rate of 140/minute, and a blood pressure of 80/50 mm Hg. What is the most appropriate initial investigation?
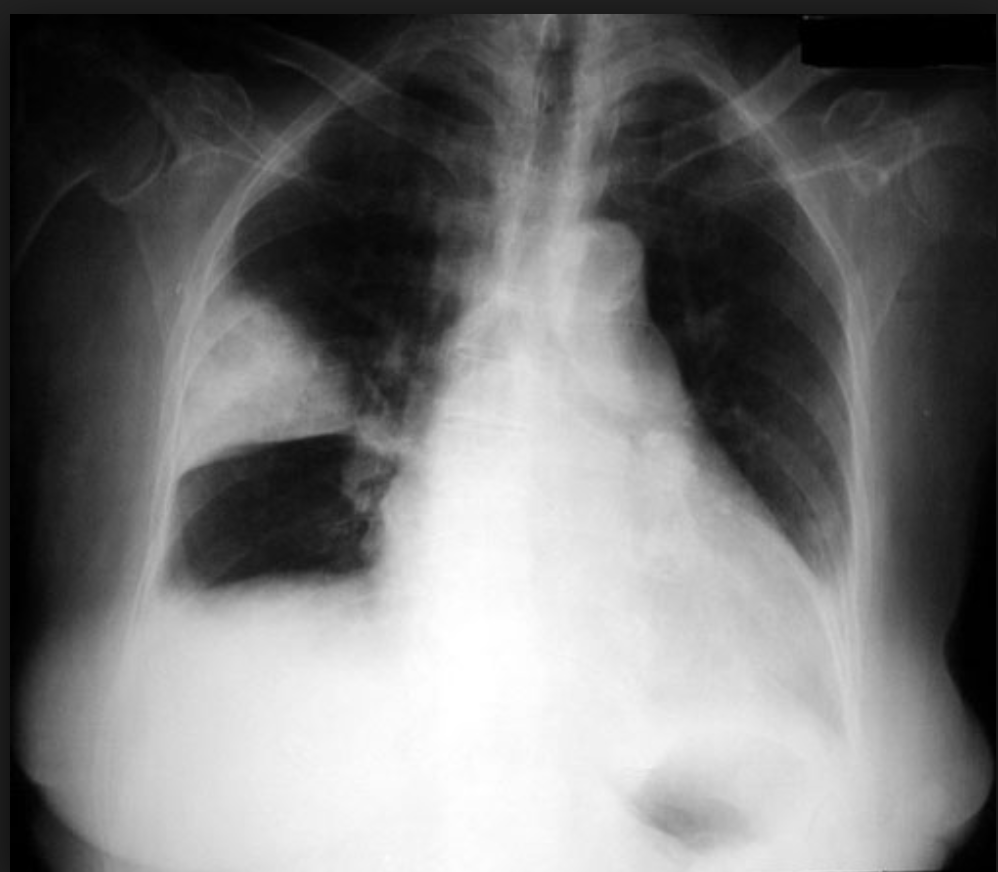
A patient presents to the emergency department with breathlessness following chest trauma. The chest X-ray is shown in the image below. What is the most appropriate next step in management?
Battle's sign is associated with which of the following conditions?
Which one of the following is the most common site of Berry aneurysm?
Practice by Chapter
Initial Assessment of Trauma Patient
Practice Questions
Advanced Trauma Life Support (ATLS) Principles
Practice Questions
Chest Trauma
Practice Questions
Abdominal Trauma
Practice Questions
Head Trauma
Practice Questions
Spinal Trauma
Practice Questions
Extremity Trauma
Practice Questions
Vascular Trauma
Practice Questions
Genitourinary Trauma
Practice Questions
Burns Management
Practice Questions
Mass Casualty Management
Practice Questions
Damage Control Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
