Trauma — MCQs

On this page
In burns management, what percentage of the total body surface area does the back constitute?
Which of the following is not a cause of secondary brain injury?
Gallow's traction is used for which of the following?
A patient presents with a condylar fracture. The occlusion is normal and mouth opening is normal. What is the best treatment?
A patient suffered from 3rd degree burn of the right upper limb, 2nd degree burns of the right lower limb, and 1st degree burn of the whole of the back. What is the total percentage of body surface area burned?
A person presents with severe abdominal trauma but was found to be hemodynamically stable on examination. What is the investigation of choice for this patient?
Which of the following is not associated with burns?
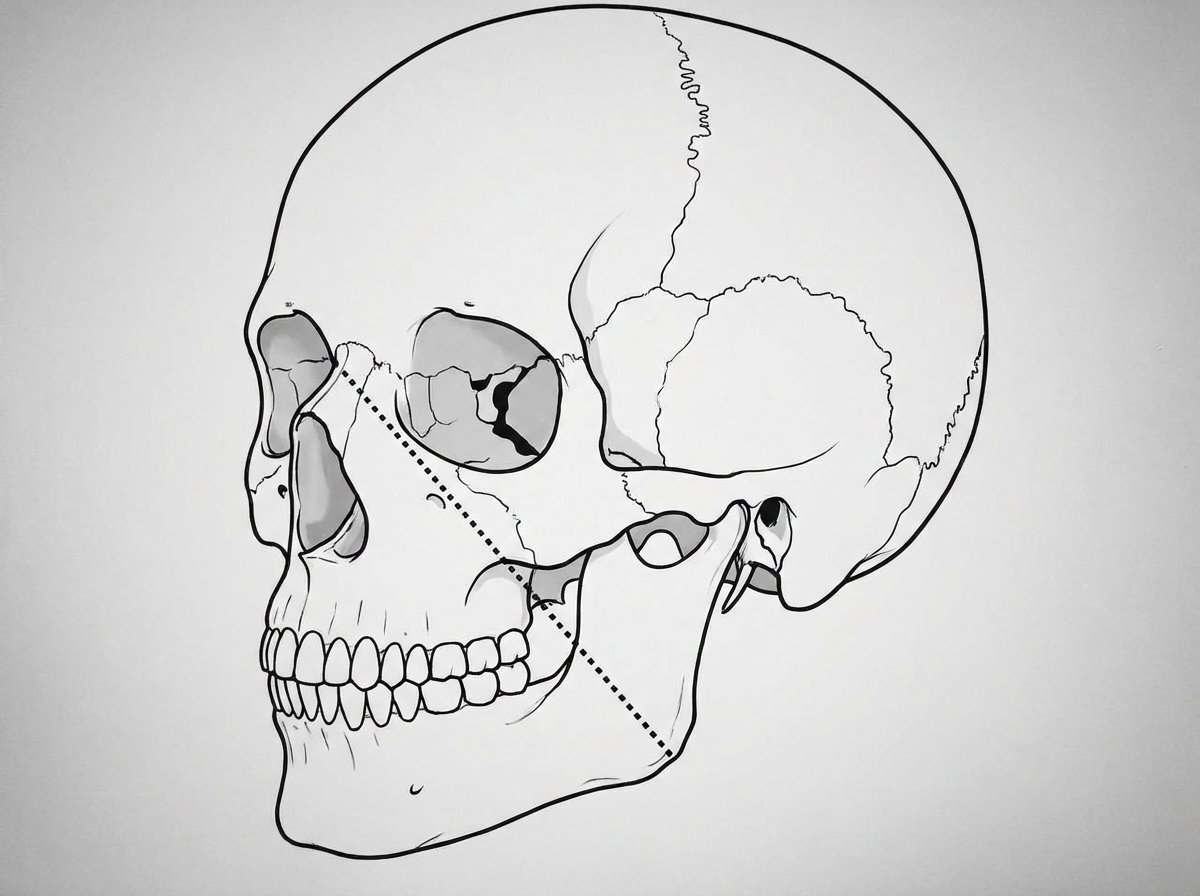
The dotted line has clinical significance in case of which of the following conditions?
A 50-year-old patient develops sudden left lower chest pain and epigastric pain after vomiting. The patient shows diaphoresis, breath sounds are decreased on the left, and there is abdominal guarding. What is the most appropriate diagnostic test?
Which of the following markers has a significant association with poor prognosis in traumatic brain injury?
Practice by Chapter
Initial Assessment of Trauma Patient
Practice Questions
Advanced Trauma Life Support (ATLS) Principles
Practice Questions
Chest Trauma
Practice Questions
Abdominal Trauma
Practice Questions
Head Trauma
Practice Questions
Spinal Trauma
Practice Questions
Extremity Trauma
Practice Questions
Vascular Trauma
Practice Questions
Genitourinary Trauma
Practice Questions
Burns Management
Practice Questions
Mass Casualty Management
Practice Questions
Damage Control Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
