Trauma — MCQs

On this page
Immediate treatment of compound fracture of tibia includes:
Which of the following is a major risk factor for fat embolism syndrome in a patient with major trauma?
Which of the following is commonest source of Extradural haemorrhage -
A 17-year-old boy is admitted to the hospital after a road traffic accident. Per abdomen examination is normal. After adequate resuscitation, his pulse rate is 80/min and BP is 110/70 mm Hg. Abdominal CT reveals a laceration in the left lobe of the liver extending from the dome more than half way through the parenchyma. Appropriate management at this time would be:
Which of the following is a treatment option for Volkmann's ischemia?
A trauma patient was brought to emergency. On evaluation, patient was found to have metabolic acidosis and coagulopathy with liver and duodenal injury. Next step:
A comatose 28-year-old woman sustained a depressed skull fracture in an automobile collision. She has been unconscious for 6 weeks. Her vital signs are stable and she breathes room air. Following her initial decompressive craniotomy, she has returned to the operating room twice due to intracranial bleeding. Select the best method of physiologic monitoring necessary for the patient.
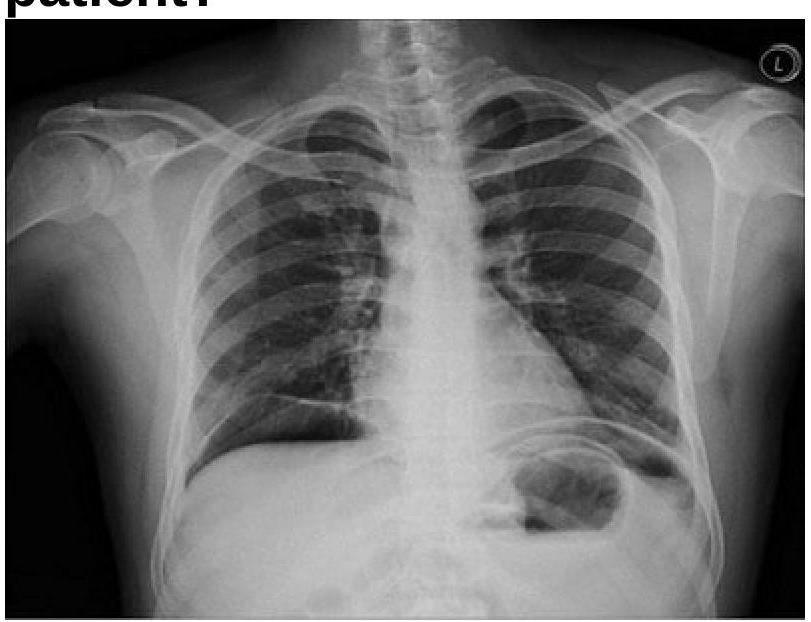
A 40 years old male was brought emergency with severe abdominal pain. On examination, pulse rate was 112/minute and systolic BP was 80 mmHg. Chest x-ray is given below. What is the most appropriate management?
What is the most common site of injury in an underwater blast?
Glasgow coma scale of a patient with head injury who is confused, localizes to pain on the right side but shows abnormal flexion on the left side, and opens eyes only to painful stimuli on sternum:
Practice by Chapter
Initial Assessment of Trauma Patient
Practice Questions
Advanced Trauma Life Support (ATLS) Principles
Practice Questions
Chest Trauma
Practice Questions
Abdominal Trauma
Practice Questions
Head Trauma
Practice Questions
Spinal Trauma
Practice Questions
Extremity Trauma
Practice Questions
Vascular Trauma
Practice Questions
Genitourinary Trauma
Practice Questions
Burns Management
Practice Questions
Mass Casualty Management
Practice Questions
Damage Control Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
