Surgical Oncology Principles — MCQs

On this page
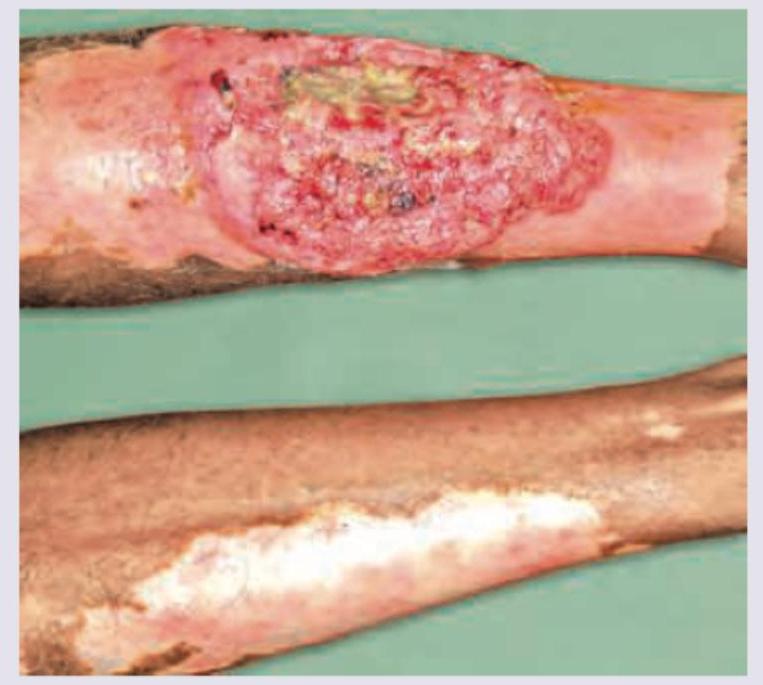
What is the most likely diagnosis based on the image provided? The patient had a snake bite at this site 5 years ago.
What technique has been depicted in the image shown below?
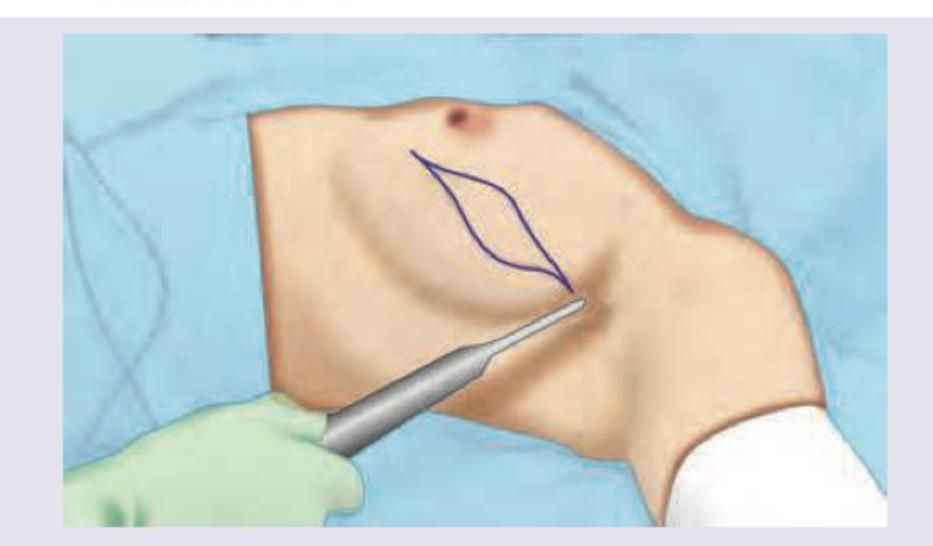
After undergoing surgery, for carcinoma of colon, a patient developed single liver metastasis of 2 cm. What would be the next treatment?
A 35-year-old HIV-positive woman (CD4 count 180/μL, on HAART) develops extensive perianal condyloma acuminata resistant to conventional treatments. HPV typing shows type 16. What is the most appropriate management approach?
A 50-year-old alcoholic patient presents with a history of waxing and waning jaundice for the past 2 months. His CT examination reveals dilatation of the common bile duct and pancreatic duct. What is the most probable diagnosis in the patient?
Which of the following cancers are correctly matched with the criteria for the minimum number of lymph nodes required for pathological staging? A. CA stomach -10 B. CA colon -12 C. CA gall bladder -6 D. CA breast -15
Marjolin's ulcer is:-
What is the most common anterior mediastinal tumor?
NOT an indication for surgery in a Ventricular septal defect
Intraoperative radiation therapy (IORT) is most commonly used in which of the following cancers?
Practice by Chapter
Cancer Biology Basics
Practice Questions
Principles of Cancer Therapy
Practice Questions
Screening and Early Detection
Practice Questions
Surgical Staging
Practice Questions
Surgical Resection Principles
Practice Questions
Lymphadenectomy
Practice Questions
Management of Metastatic Disease
Practice Questions
Combined Modality Therapy
Practice Questions
Targeted Therapy Concepts
Practice Questions
Cancer Survivorship
Practice Questions
Palliative Surgical Interventions
Practice Questions
Ethics in Cancer Care
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
