Surgical Infections — MCQs

On this page
Secondary amyloidosis occurs in which of the following conditions?
Malignant pustule occurs in which condition?
Periosteal reaction in a case of acute osteomyelitis can be seen earliest at:
What is true about primary peritonitis?
A diabetic worker sustains a stab injury to the central region of his palm. After 3 days, he develops swelling, severe pain, and inability to extend his middle and ring fingers. Pus accumulation is suspected in one of the palmar spaces. Which of the following spaces is most likely involved?
A patient with diffuse severely contaminated peritonitis underwent laparotomy and was left open after surgery. Which of the following might help?
Identify the tube/catheter shown in the figure:

What is incorrect about the image shown?
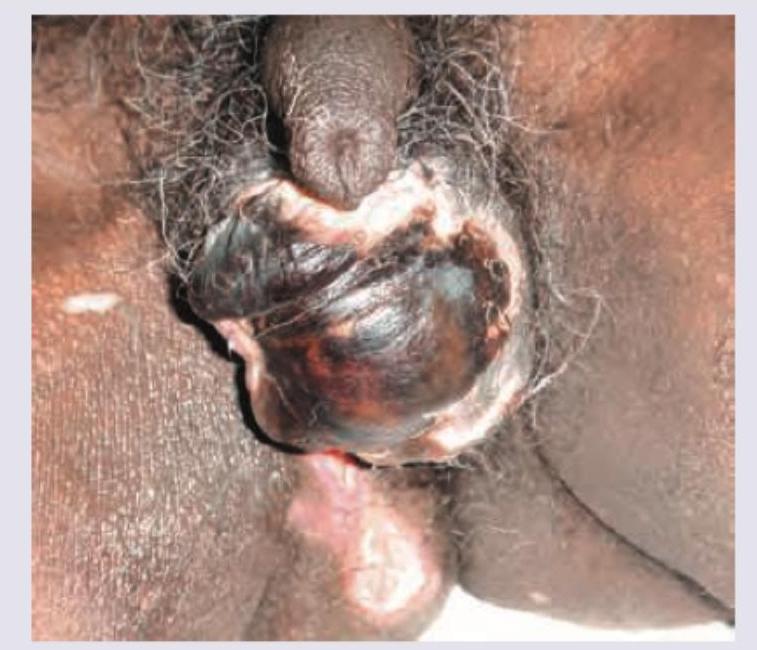
A 65-year-old patient presents with sudden pain in the scrotum associated with prostration, pallor and pyrexia. What could be the most probable diagnosis?
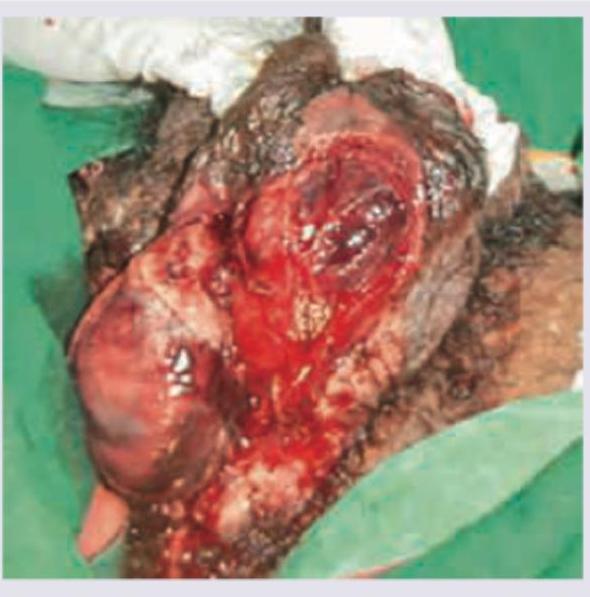
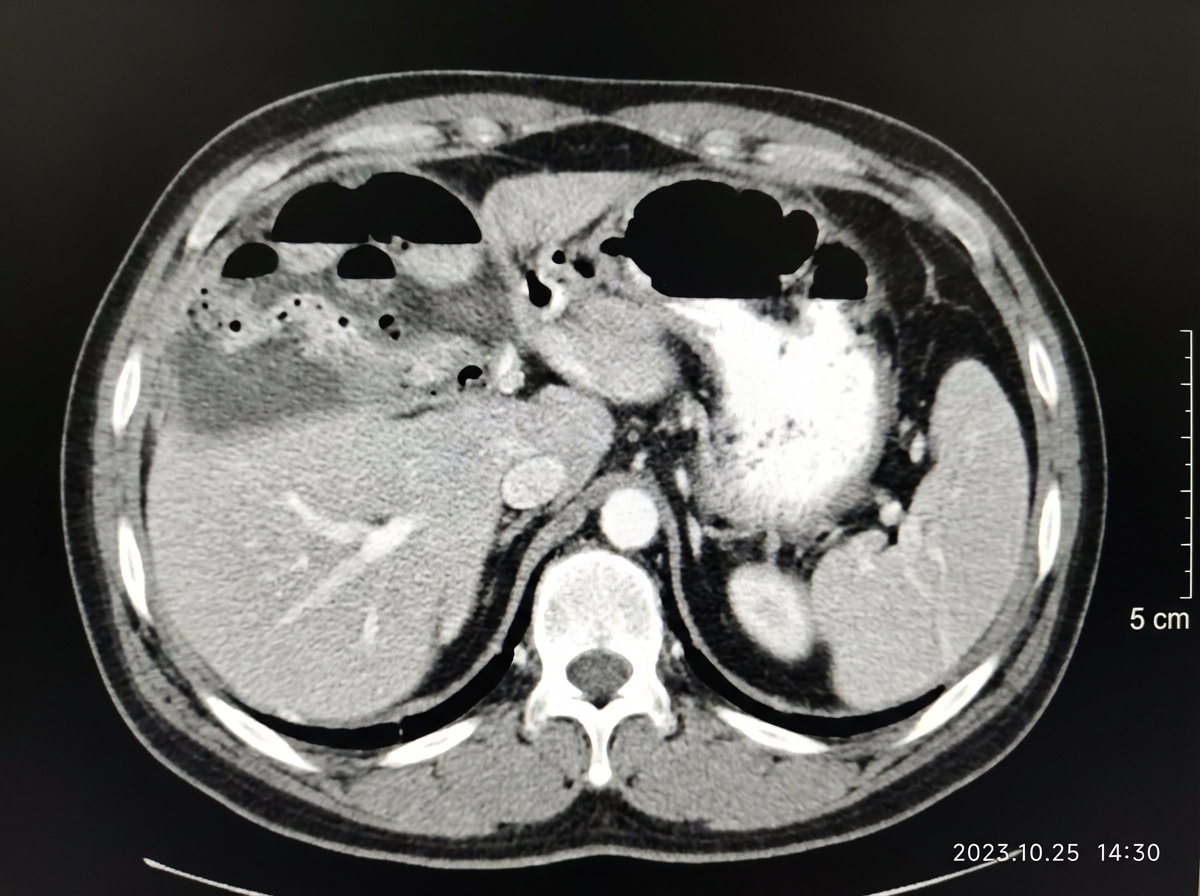
A patient after abdominal surgery presents with fever, chills, rigors along with pain in right hypochondrium, right shoulder along with Hoover's sign. Abdominal CT of the patient is given. What is the most likely diagnosis?
Practice by Chapter
Surgical Site Infections
Practice Questions
Intra-abdominal Infections
Practice Questions
Soft Tissue Infections
Practice Questions
Necrotizing Soft Tissue Infections
Practice Questions
Surgical Sepsis
Practice Questions
Tetanus Prophylaxis
Practice Questions
Antimicrobial Prophylaxis
Practice Questions
Antimicrobial Therapy in Surgical Infections
Practice Questions
Surgical Drainage Procedures
Practice Questions
Infection Control in Operating Room
Practice Questions
Biofilms and Implant-Related Infections
Practice Questions
Prevention Strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
