Preoperative and Postoperative Care — MCQs

On this page
What is the cardinal rule for dressing a pressure ulcer?
How many days before surgery should warfarin be stopped?
During a hysteroscopic removal of a submucosal fibroid, a fluid deficit of 2000 mL is estimated in a patient. What is the immediate complication of this?
The image below shows a pressure sore. Which stage does this belong to?
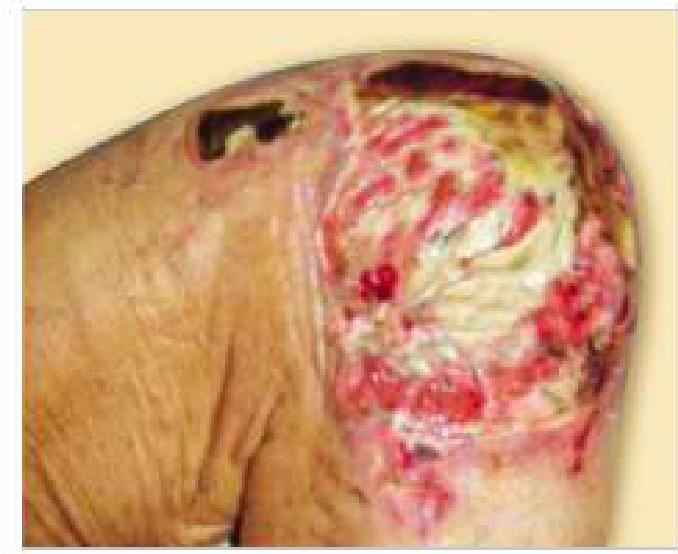
A pregnant female had meconium-stained liquor and underwent emergency LSCS. A few days later, her condition deteriorated, and an ultrasound showed edematous bowels. What is the most likely cause of her condition?
Reactionary Hemorrhage occurs due to?
What type of respiratory failure is most commonly observed in post-operative patients?
Steroids are injurious to wound healing when administered during which time frame?
Among the following single parameters, malnutrition in surgical patients is best assessed by:
In a case of perforation peritonitis treated with emergency laparotomy, a patient develops oliguria on the 2nd post-operative day. What is the most likely diagnosis?
Practice by Chapter
Preoperative Risk Assessment
Practice Questions
Perioperative Management of Comorbidities
Practice Questions
Preparation of Patient for Surgery
Practice Questions
Informed Consent Process
Practice Questions
Post-Anesthesia Care
Practice Questions
Pain Management
Practice Questions
Wound Care and Dressings
Practice Questions
Drain Management
Practice Questions
Postoperative Complications Detection
Practice Questions
Early Ambulation and Rehabilitation
Practice Questions
Enhanced Recovery After Surgery (ERAS) Protocols
Practice Questions
Discharge Planning and Follow-up
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
