Preoperative and Postoperative Care — MCQs

On this page
Which of the following is not a known complication associated with the procedure done in the patient?
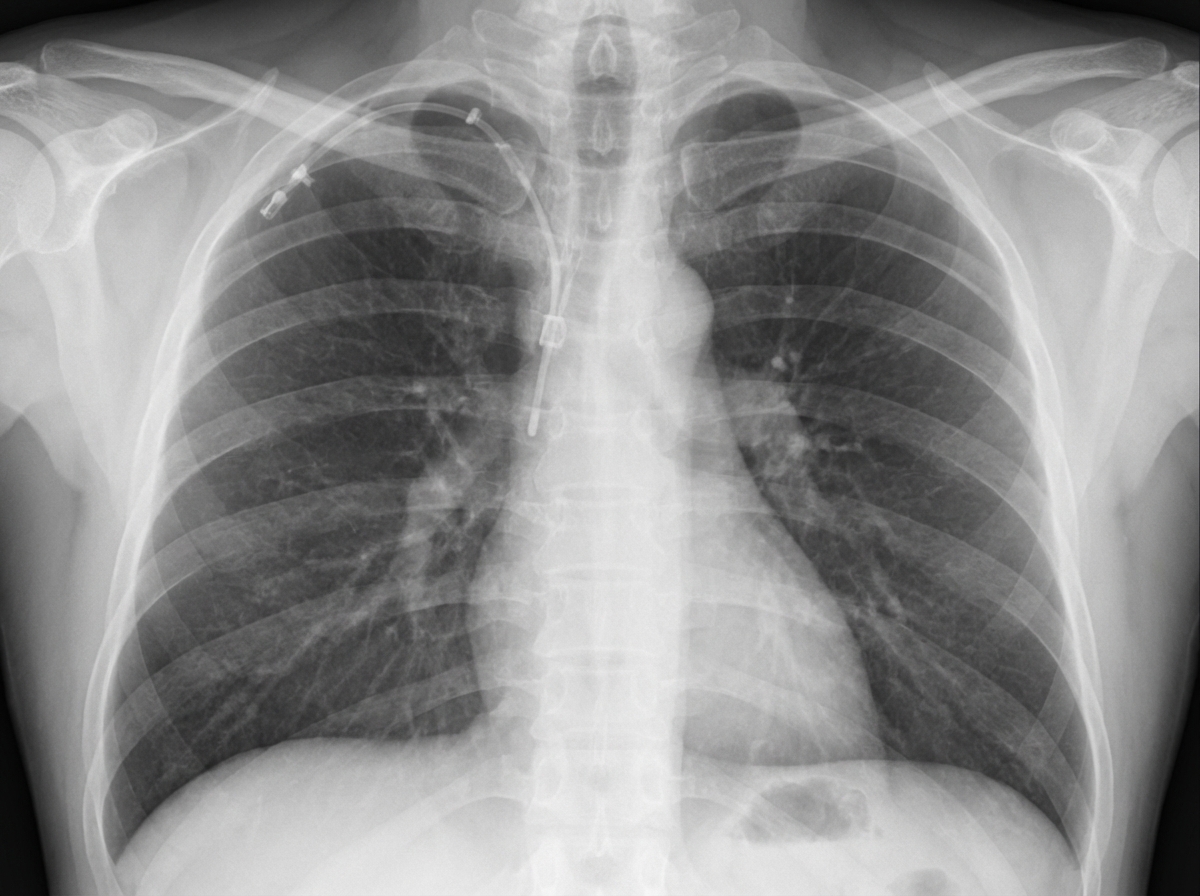
Secondary hemorrhage is seen:
Which of the following is not a risk factor for postoperative pulmonary complication?
All of the following are indicators of adequacy of pre-operative resuscitation except
Which of the following is not a component of the Goldman Revised Cardiac Risk Index?
If suture marks are to be avoided, skin sutures should be removed by:
Which of the following is the most pathognomonic sign of impending burst abdomen:
Blood loss during major surgery is best estimated by:
Which of the following surgical incisions is associated with the highest risk of postoperative pulmonary complications ?
Optimum urine output in post-operative patient:
Practice by Chapter
Preoperative Risk Assessment
Practice Questions
Perioperative Management of Comorbidities
Practice Questions
Preparation of Patient for Surgery
Practice Questions
Informed Consent Process
Practice Questions
Post-Anesthesia Care
Practice Questions
Pain Management
Practice Questions
Wound Care and Dressings
Practice Questions
Drain Management
Practice Questions
Postoperative Complications Detection
Practice Questions
Early Ambulation and Rehabilitation
Practice Questions
Enhanced Recovery After Surgery (ERAS) Protocols
Practice Questions
Discharge Planning and Follow-up
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
