Preoperative and Postoperative Care — MCQs

On this page
A woman presents 4 days after a laparotomy with complete wound dehiscence. After prescribing antibiotics the surgeon decides to suture the wound. Which of these suture materials should he use?
You are asked to put a 22-gauge cannula in a patient. Which of the following cannula will you put?
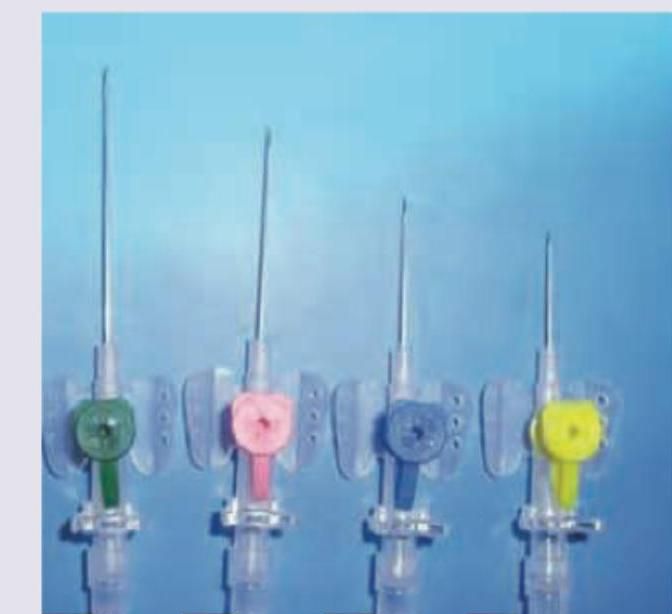
What does the image show? (AIIMS Nov 2018)
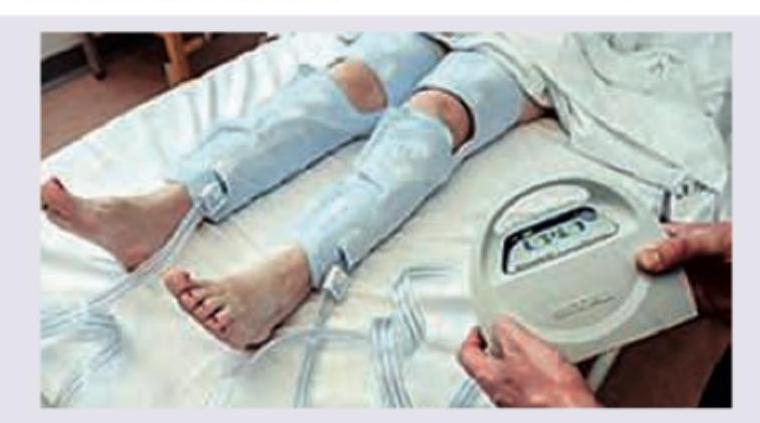
The following image shows:
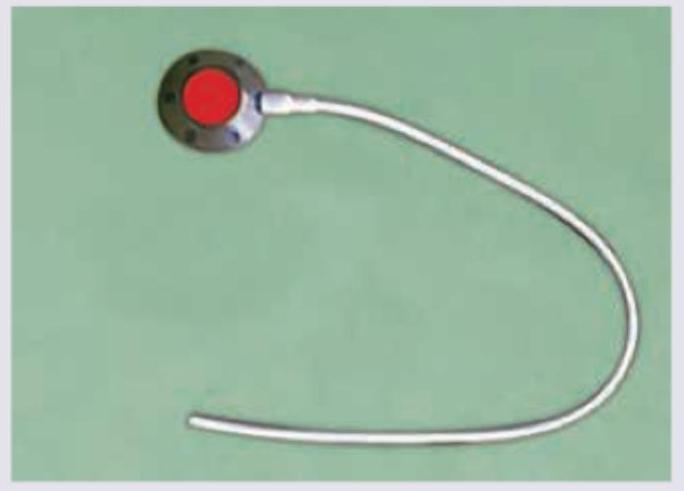
The image on the left shows a procedure. What is the procedure associated with this image?
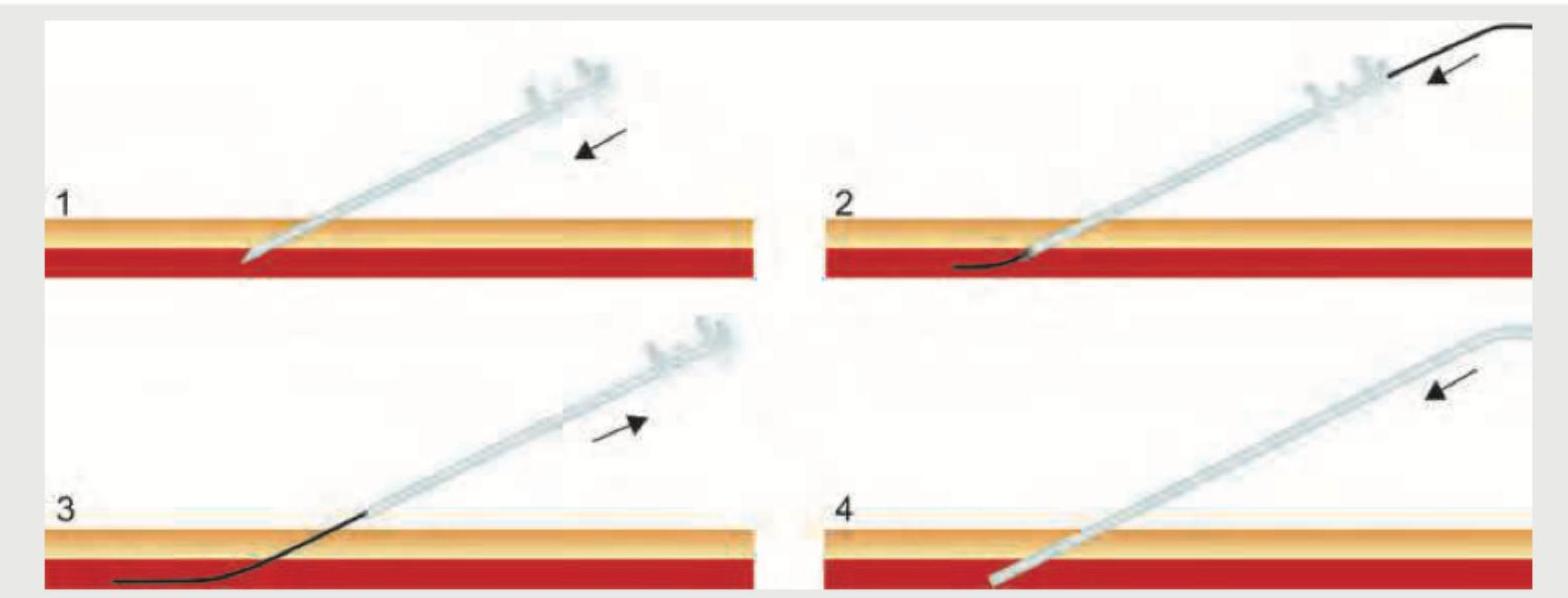
Consider the following : I. Diabetes II. Hypertension III. Renal failure IV. Jaundice Which of the above are the risk factors for post-operative wound dehiscence?
Which of the following are the common complications associated with enteral nutrition in postoperative patients ? 1. Tube malposition, displacement 2. Diarrhoea, constipation 3. Predisposition to systemic sepsis 4. Electrolytic imbalance Select the correct answer using the code given below :
A young 28-year-old male was operated for duodenal ulcer perforation peritonitis. After having recovered well for five days, he developed high fever with chills and symptoms of toxemia. He developed right shoulder tip pain and intractable hiccoughs. The most likely diagnosis is :
A malnourished 60-year-old man underwent emergency surgery for Strangulated Sigmoid Volvulus. After resection of the sigmoid colon, a colostomy was fashioned. The postoperative period was stormy and he developed a painful calf swelling in right lower limb. The most probable diagnosis is :
Preoperative investigations done prior to surgery depend upon which of the following? 1. Type of surgery 2. Patient origin 3. Patient comorbidities 4. Experience of surgeon
Practice by Chapter
Preoperative Risk Assessment
Practice Questions
Perioperative Management of Comorbidities
Practice Questions
Preparation of Patient for Surgery
Practice Questions
Informed Consent Process
Practice Questions
Post-Anesthesia Care
Practice Questions
Pain Management
Practice Questions
Wound Care and Dressings
Practice Questions
Drain Management
Practice Questions
Postoperative Complications Detection
Practice Questions
Early Ambulation and Rehabilitation
Practice Questions
Enhanced Recovery After Surgery (ERAS) Protocols
Practice Questions
Discharge Planning and Follow-up
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
