Plastic and Reconstructive Surgery — MCQs

On this page
Which flap is commonly used in breast reconstruction?
A skin graft is performed on a wound using skin taken from an identical twin brother. What type of graft is this?
Which layer is involved in blister formation in a superficial partial thickness burn?
Which statement regarding cleft palate repair is false?
A 65-year-old male presents with a 5 cm high-grade liposarcoma on the back of his lower thigh. What is the best management?
What is the most common type of skin carcinoma on the face in light-skinned individuals?
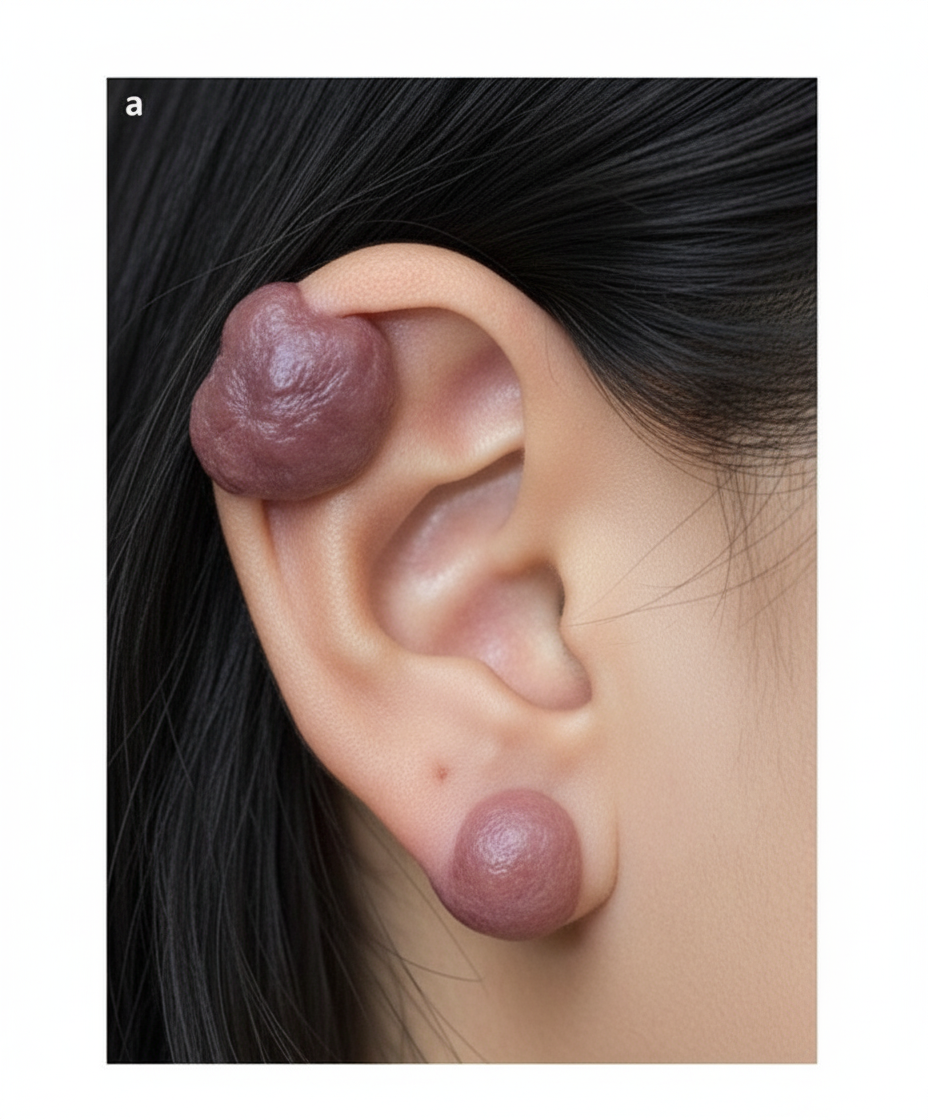
Which of the following is the best treatment for this condition?
Lahsal classification is used for:
A patient underwent surgery for pilonidal sinus, which type of flap is used in this surgery?
A patient underwent split-thickness skin grafting for a burn injury on the arm. On post-operative day 6, he develops stiffness of the arm during physiotherapy. What is the most appropriate next step in management?
Practice by Chapter
Wound Healing
Practice Questions
Skin Grafts
Practice Questions
Flap Surgery Principles
Practice Questions
Local Flaps
Practice Questions
Regional Flaps
Practice Questions
Microsurgical Techniques
Practice Questions
Tissue Expansion
Practice Questions
Breast Reconstruction
Practice Questions
Hand Surgery Basics
Practice Questions
Craniofacial Surgery Principles
Practice Questions
Aesthetic Surgery Concepts
Practice Questions
Body Contouring
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
