Plastic and Reconstructive Surgery — MCQs

On this page
A 3.3 kg, 36-week baby girl was born prematurely after labor caused by ruptured membranes. Prenatal ultrasound revealed polyhydramnios at 26 weeks. Fetal echocardiogram was normal and amniocentesis was without genetic aberrance. On examination, there was a normal anus, and a nasogastric tube drained bile-stained fluid. The baby passed some mucus but no typical dark meconium. A chest and abdominal X-ray showed a "double bubble sign". What is the most likely diagnosis?
What is the world's largest charity dedicated to cleft lip and palate treatment?
Which of the following statements regarding an axial flap is true?
Millard's 'Rule of Ten' includes all except?
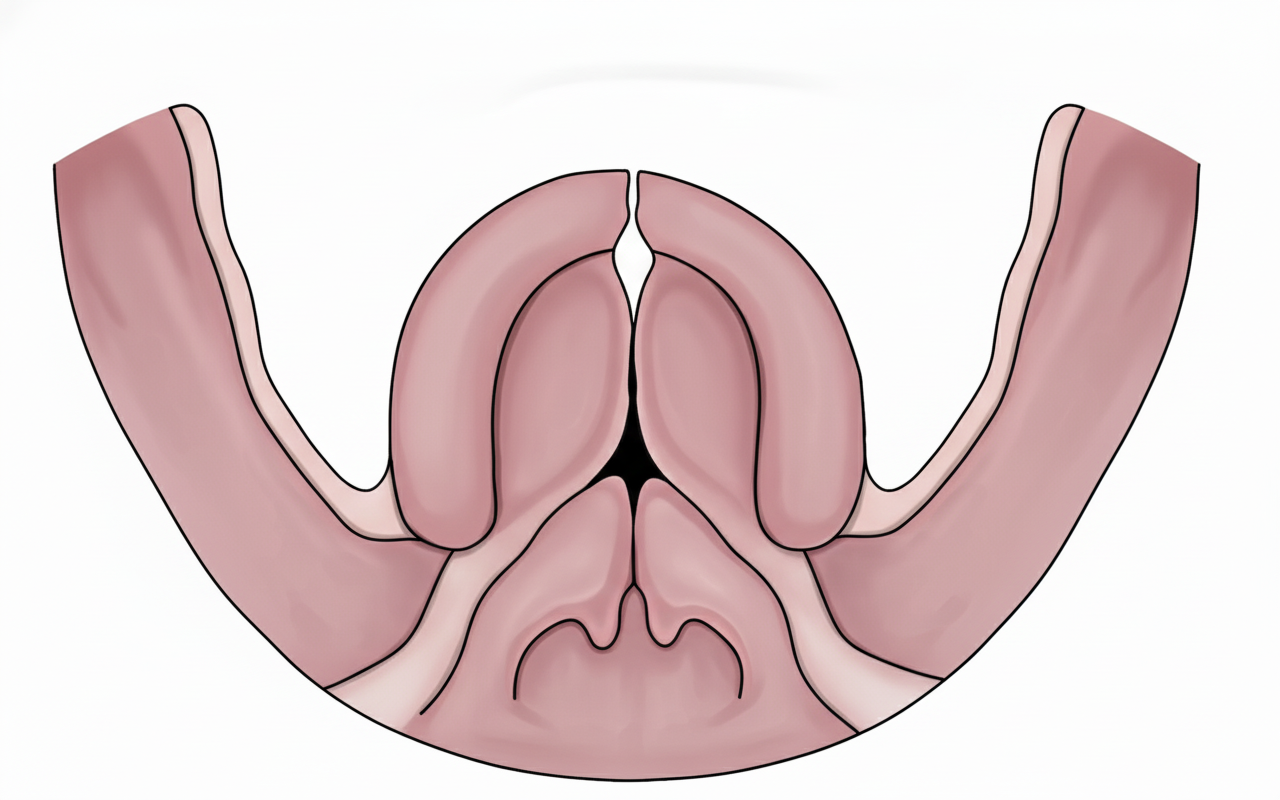
According to Veau's classification, which class does the diagrammatic representation of cleft palate belong to?
Acanthosis nigricans is typically associated with which of the following conditions?
Which of the following flaps are used for lip reconstruction?
What is the recommended incision for a felon?
Which of the following is NOT a method for operating on a cleft lip?
What is Zadek's procedure?
Practice by Chapter
Wound Healing
Practice Questions
Skin Grafts
Practice Questions
Flap Surgery Principles
Practice Questions
Local Flaps
Practice Questions
Regional Flaps
Practice Questions
Microsurgical Techniques
Practice Questions
Tissue Expansion
Practice Questions
Breast Reconstruction
Practice Questions
Hand Surgery Basics
Practice Questions
Craniofacial Surgery Principles
Practice Questions
Aesthetic Surgery Concepts
Practice Questions
Body Contouring
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
