Plastic and Reconstructive Surgery — MCQs

On this page
What is the typical thickness range for split-thickness skin grafts used in maxillofacial surgery?
Port wine stain is seen in which of the following conditions?
To avoid suture marks, when should sutures on the face be removed?
The Abbe-Estlander flap is used for reconstruction of which anatomical structure?
Down fracture of the zygomatic arch is a treatment modality for which condition?
Which neuromuscular preserving flap is used in lip reconstruction?
The names Manchot, Salmon, and Taylor are related to which of the following?
A free skin graft is typically rejected when transplanted onto which of the following tissues?
A 12-year-old girl presents to the emergency department following a skiing crash in which the left side of her mid torso hit a tree. She presents with left side lower chest and upper abdominal pain. She also complains of left shoulder pain. What is the most likely diagnosis?
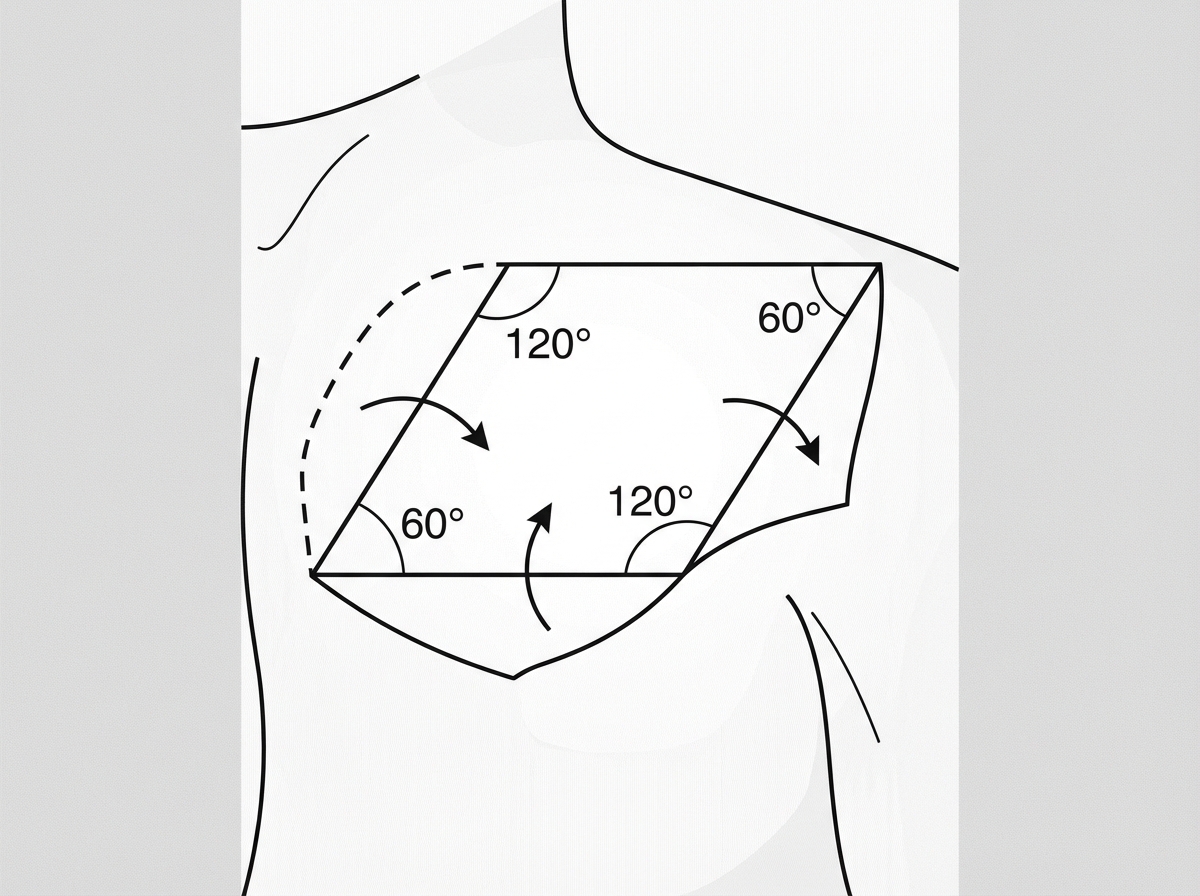
What is the name of the flap shown in the image?
Practice by Chapter
Wound Healing
Practice Questions
Skin Grafts
Practice Questions
Flap Surgery Principles
Practice Questions
Local Flaps
Practice Questions
Regional Flaps
Practice Questions
Microsurgical Techniques
Practice Questions
Tissue Expansion
Practice Questions
Breast Reconstruction
Practice Questions
Hand Surgery Basics
Practice Questions
Craniofacial Surgery Principles
Practice Questions
Aesthetic Surgery Concepts
Practice Questions
Body Contouring
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
