Plastic and Reconstructive Surgery — MCQs

On this page
What is the degree of this burn shown below?
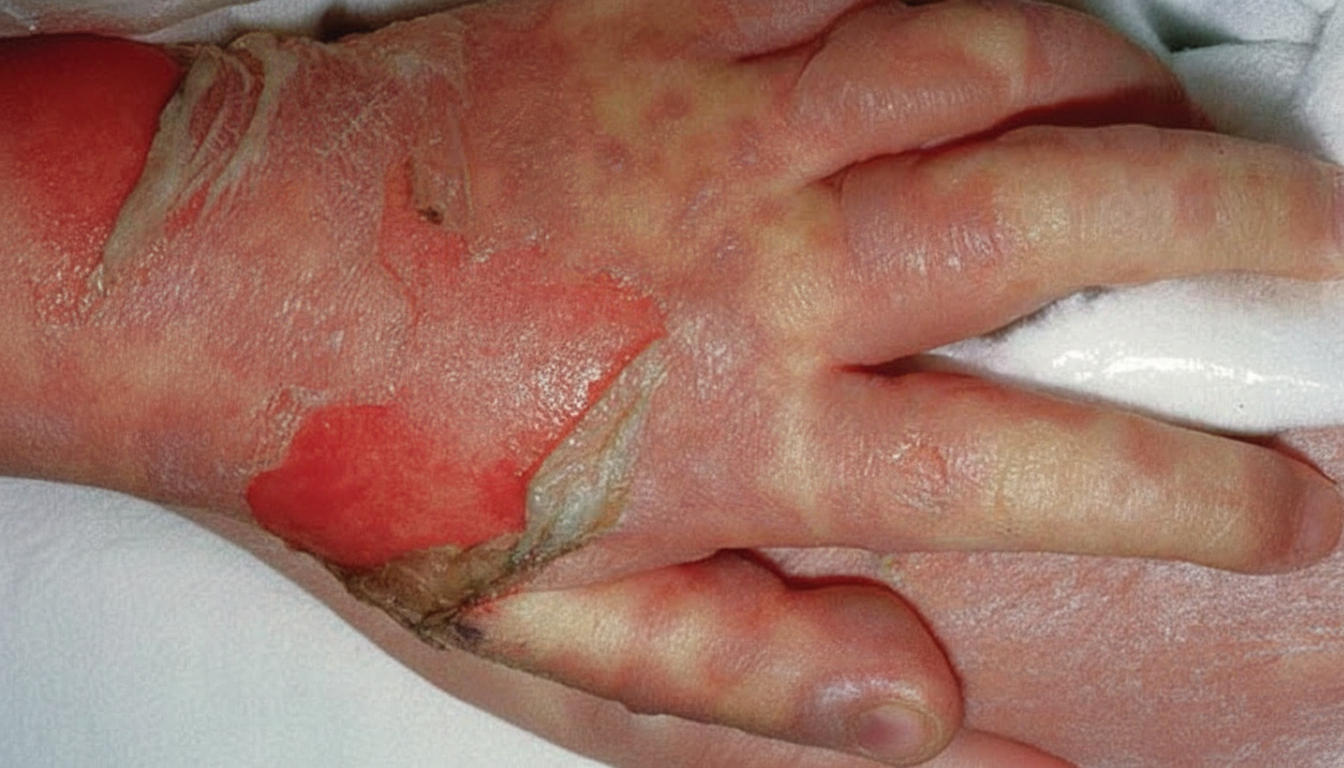
Poland syndrome is characterized by all of the following abnormalities except:
In the treatment of hand injuries, what is the greatest priority?
What is a partial-thickness skin graft also known as?
All of the following statements about cleft palate are true, EXCEPT:
The Abbe-Estlander flap is based on which artery?
What type of graft is a Thiersch graft?
The rectus abdominis free flap is supplied by which artery?
Thompson's Operation for Lymphoedema is:
What is the ideal graft for a leg injury with a 10 x 10 cm exposed bone area?
Practice by Chapter
Wound Healing
Practice Questions
Skin Grafts
Practice Questions
Flap Surgery Principles
Practice Questions
Local Flaps
Practice Questions
Regional Flaps
Practice Questions
Microsurgical Techniques
Practice Questions
Tissue Expansion
Practice Questions
Breast Reconstruction
Practice Questions
Hand Surgery Basics
Practice Questions
Craniofacial Surgery Principles
Practice Questions
Aesthetic Surgery Concepts
Practice Questions
Body Contouring
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
