Pediatric Surgery — MCQs

On this page
At what time is the optimal surgical timing for a sacrococcygeal teratoma?
What is the surgical treatment for duodenal atresia?
All of the following are suggestive of a low lesion in anorectal malformation except?
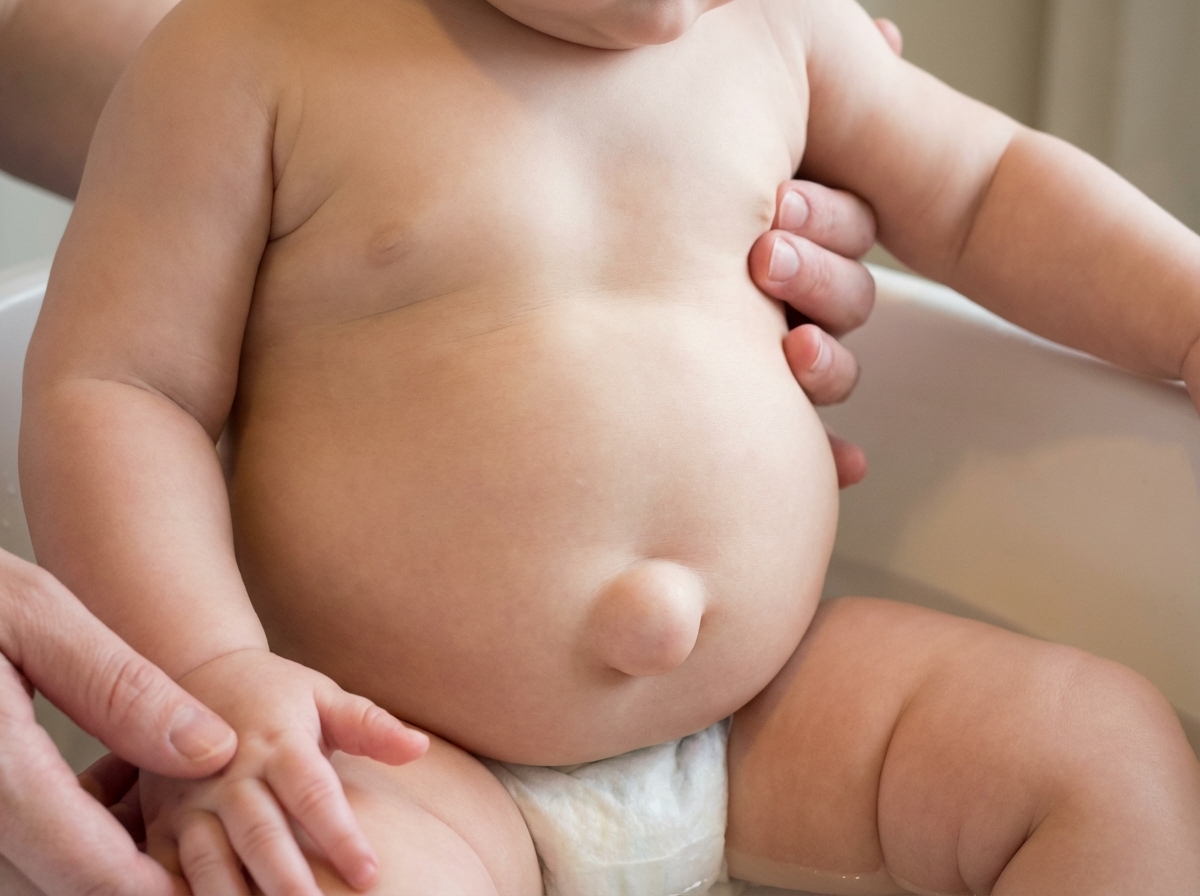
What is the indication for surgery in a child with an umbilical hernia?
Orchidopexy for incompletely descended testis is done after what age?
What is the most common intra-abdominal tumor in children under two years of age?
A child presented with evisceration of bowel loops coming out of a defect in the abdominal wall to the right of the umbilicus. What is the possible diagnosis?
What is the most common presentation of a double aortic arch in infants?
A 6-month-old child is brought to the clinic. The image shows the condition. What is the appropriate management protocol?
Unilateral undescended testes is ideally operated around what age?
Practice by Chapter
Neonatal Physiology
Practice Questions
Congenital Anomalies Overview
Practice Questions
Neonatal Intestinal Obstruction
Practice Questions
Necrotizing Enterocolitis
Practice Questions
Hirschsprung's Disease
Practice Questions
Anorectal Malformations
Practice Questions
Pediatric Hernias
Practice Questions
Pyloric Stenosis
Practice Questions
Biliary Atresia
Practice Questions
Pediatric Tumors
Practice Questions
Congenital Diaphragmatic Hernia
Practice Questions
Pediatric Trauma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
