Pediatric Surgery — MCQs

On this page
Kasai procedure is used in the treatment of which condition?
Two days after birth, a child developed respiratory distress and had a scaphoid abdomen. Breath sounds were decreased on the left side. After bag and mask ventilation, an endotracheal tube was inserted, and the maximal cardiac impulse shifted to the right side. What should be the next step in management?
Which condition is treated with a Bishop-Koop operation?
Regarding Gastroschisis and omphalocele, which of the following statements is false?
Cleft palate is ideally repaired at what age?
What is your diagnosis in this neonate with visible bowel loops at birth?
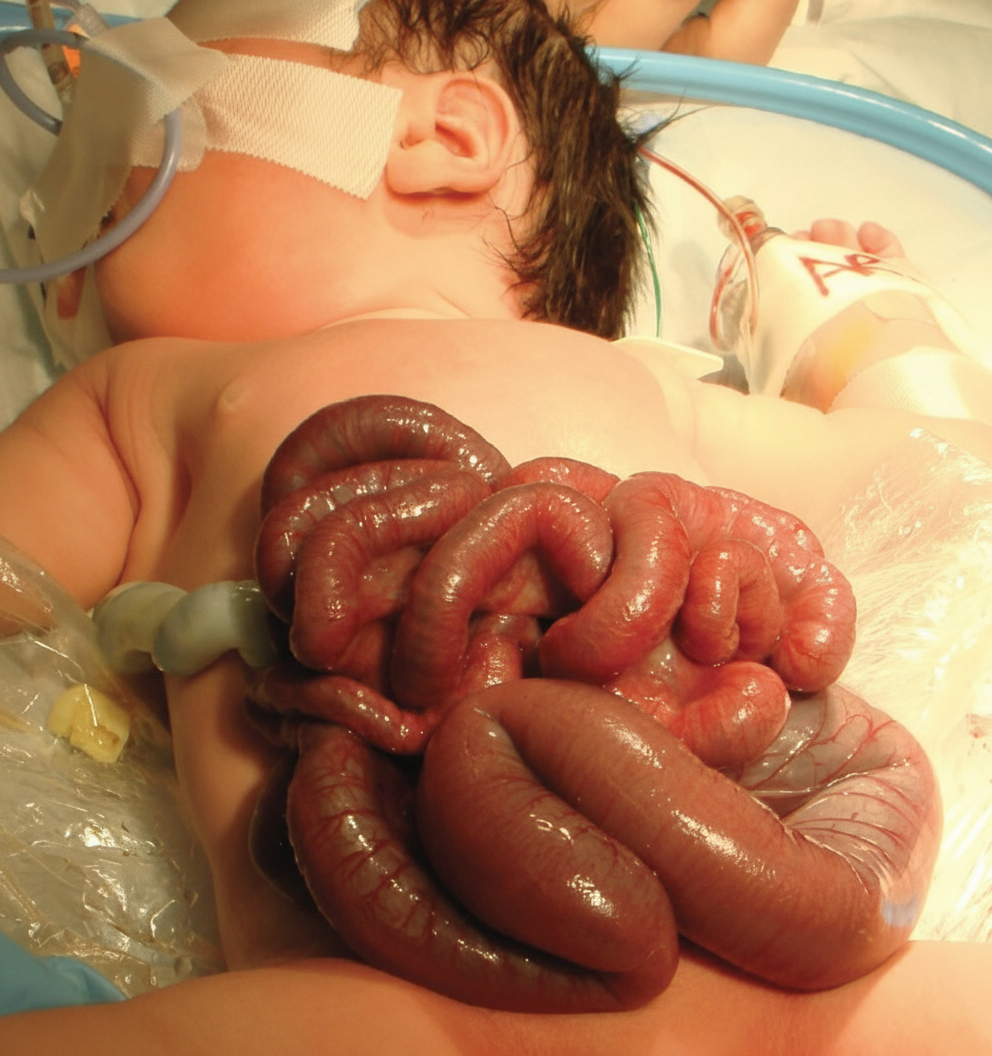
Which of the following statements regarding gastroschisis is TRUE?
Which one of the following is not a feature of congenital hypertrophic pyloric stenosis?
True about intussusceptions in children?
What is the approximate incidence of anastomotic leak following repair of esophageal atresia?
Practice by Chapter
Neonatal Physiology
Practice Questions
Congenital Anomalies Overview
Practice Questions
Neonatal Intestinal Obstruction
Practice Questions
Necrotizing Enterocolitis
Practice Questions
Hirschsprung's Disease
Practice Questions
Anorectal Malformations
Practice Questions
Pediatric Hernias
Practice Questions
Pyloric Stenosis
Practice Questions
Biliary Atresia
Practice Questions
Pediatric Tumors
Practice Questions
Congenital Diaphragmatic Hernia
Practice Questions
Pediatric Trauma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
