Pediatric Surgery — MCQs

On this page
What is the definitive treatment for Tetralogy of Fallot (TOF)?
All are features of congenital megacolon except:
A 13-year-old boy has a 3-day history of low-grade fever, symptoms of upper respiratory infection, and a sore throat. A few hours before his presentation to the emergency room, he has an abrupt onset of high fever, difficulty swallowing, and poor handling of his secretions. He indicates that he has a marked worsening in the severity of his sore throat. His pharynx has a fluctuant bulge in the posterior wall. A soft tissue radiograph of his neck is shown. Which of the following is the most appropriate initial therapy for this patient?

What is the most common complication occurring in tracheostomy in children? (March 2004)
A newborn suffering from perforated necrotizing enterocolitis is having very poor general condition. He is currently stabilized on ventilator. Which of the following should be done in the management of this patient?
The commonest cause of intestinal obstruction in children is –
A 12-year-old male is admitted to the hospital with profuse rectal bleeding but appears to be free of any associated pain. Which of the following is the most common cause of severe rectal bleeding in the pediatric age group?
The ideal timing of radiotherapy for Wilms tumour after surgery is:
A 7-year-old female who is somewhat obese is brought to the emergency department because of a soft lump above the buttocks. Upon physical examination you note the lump is located just superior to the iliac crest unilaterally on the left side. The protrusion is deep to the skin and pliable to the touch. Which of the following is the most probable diagnosis?
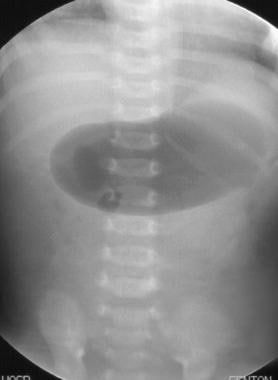
A 1-week-old previously healthy infant presents to the emergency room with the acute onset of bilious vomiting. The abdominal plain film in the emergency department (A) and the barium enema done after admission (B) are shown. Which of the following is the most likely diagnosis for this patient?
Practice by Chapter
Neonatal Physiology
Practice Questions
Congenital Anomalies Overview
Practice Questions
Neonatal Intestinal Obstruction
Practice Questions
Necrotizing Enterocolitis
Practice Questions
Hirschsprung's Disease
Practice Questions
Anorectal Malformations
Practice Questions
Pediatric Hernias
Practice Questions
Pyloric Stenosis
Practice Questions
Biliary Atresia
Practice Questions
Pediatric Tumors
Practice Questions
Congenital Diaphragmatic Hernia
Practice Questions
Pediatric Trauma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
