Pediatric Surgery — MCQs

On this page
A 3-year-old child presents with congenital diaphragmatic hernia requiring repair. Preoperative echocardiogram shows severe pulmonary hypertension with suprasystemic pressures. The pediatric surgeon recommends immediate repair, while the cardiologist suggests optimizing pulmonary pressures first. Evaluate the optimal timing and approach.
A 16-year-old competitive swimmer presents with recurrent shoulder dislocation. MRI shows a Bankart lesion and significant bone loss. His coach wants him to return to competition quickly, his parents are concerned about long-term function, and the patient wants to continue swimming. Evaluate the management approach that best addresses all stakeholder concerns.
A patient presents with fecal discharge from the umbilicus. What is the most likely diagnosis?
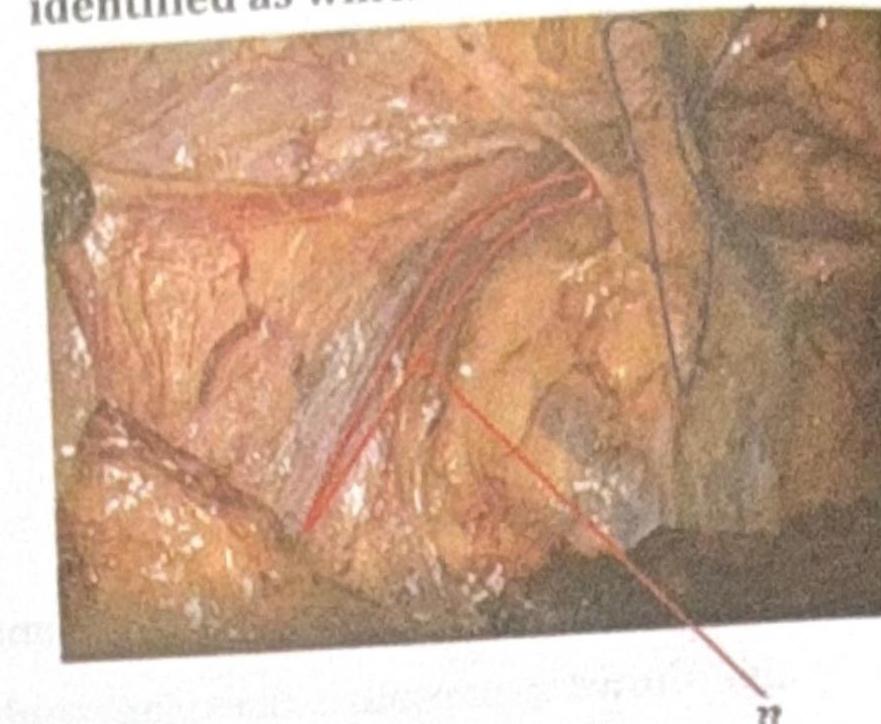
In the intraoperative image of congenital hernia repair, the structure marked by the red arrow is identified as which of the following?
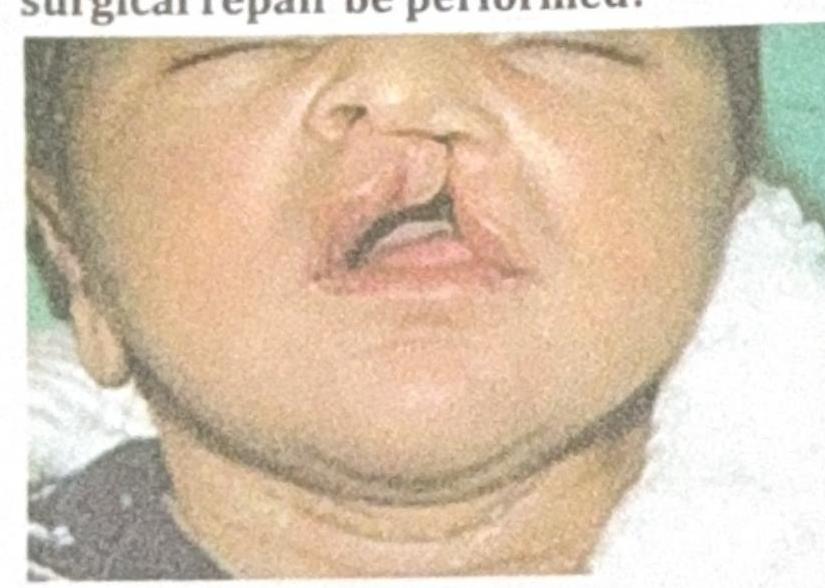
A child presents to the OPD with the finding shown in the image. When should the first surgical repair be performed?
A 6-month-old child presents with an umbilical hernia measuring 3 cm in diameter. What is the management protocol?
The metabolic derangement in congenital pyloric stenosis is -
All of the following are true about congenital hypertrophic pyloric stenosis except
Investigation of choice for Posterior urethral valves?
A child presented with intermittent episodes of left sided flank pain. Ultrasonography reveals large hydronephrosis with dilated renal pelvis and cortical thinning with a normal ureter. Kidney differential function was observed to be 19%. Which of the following is the best management?
Practice by Chapter
Neonatal Physiology
Practice Questions
Congenital Anomalies Overview
Practice Questions
Neonatal Intestinal Obstruction
Practice Questions
Necrotizing Enterocolitis
Practice Questions
Hirschsprung's Disease
Practice Questions
Anorectal Malformations
Practice Questions
Pediatric Hernias
Practice Questions
Pyloric Stenosis
Practice Questions
Biliary Atresia
Practice Questions
Pediatric Tumors
Practice Questions
Congenital Diaphragmatic Hernia
Practice Questions
Pediatric Trauma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
