Pediatric Surgery — MCQs

On this page
The EXIT (Ex utero intrapartum therapy) procedure is indicated for fetal conditions that obstruct the airway or impede ventilation. In which of the following conditions is the EXIT procedure NOT indicated?
What is the most common tumor of the small bowel in children?
A newborn with meningomyelocele is scheduled for surgery. What should be immediately used to cover the defect?
A boy with undescended testis, what is the primary concern that necessitates surgical intervention?
Which of the following is true regarding hypospadias?
What is the type of the given intestinal atresia?
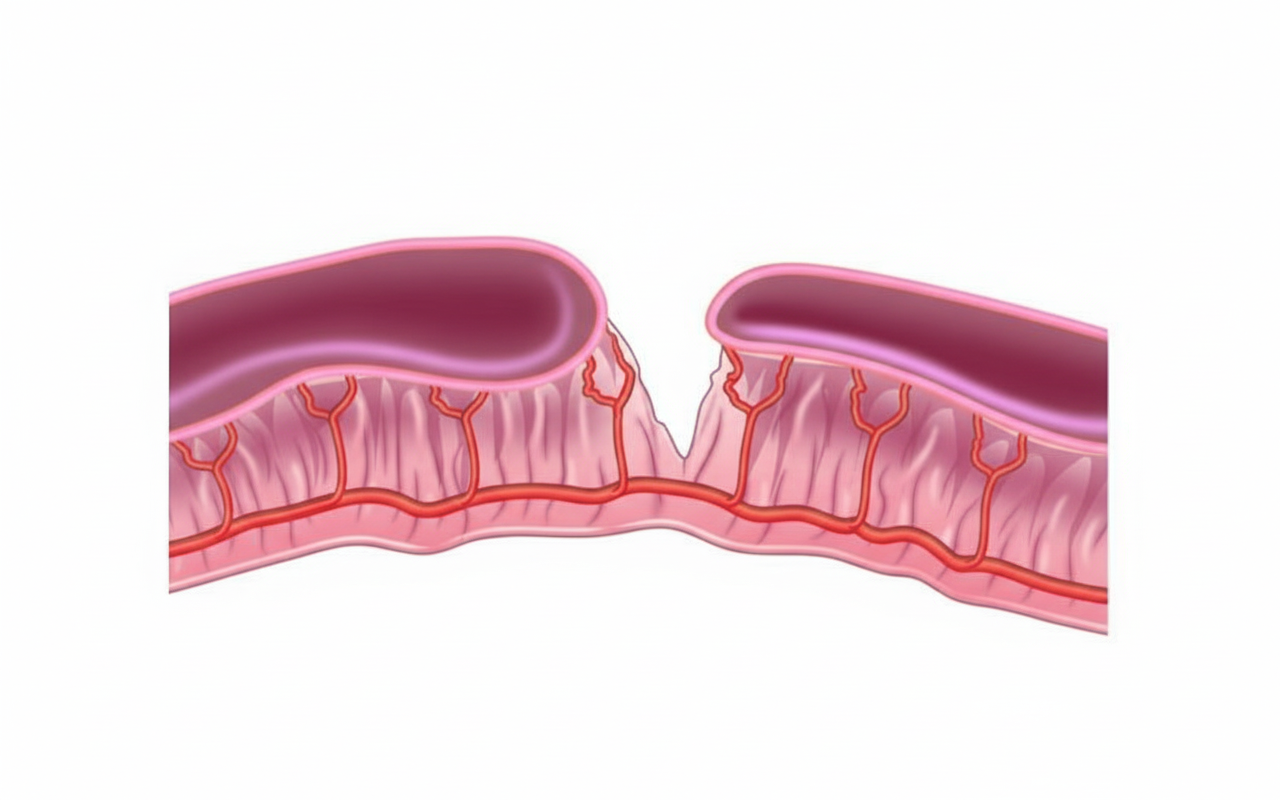
Which of the following statements about appendicitis in children is false?
Kasai's procedure is the treatment of choice for which condition?
What is the better prognostic factor for operation of biliary duct obstruction in a newborn?
Recurrent pain abdomen with intestinal obstruction and a mass passing per rectum is most suggestive of which condition?
Practice by Chapter
Neonatal Physiology
Practice Questions
Congenital Anomalies Overview
Practice Questions
Neonatal Intestinal Obstruction
Practice Questions
Necrotizing Enterocolitis
Practice Questions
Hirschsprung's Disease
Practice Questions
Anorectal Malformations
Practice Questions
Pediatric Hernias
Practice Questions
Pyloric Stenosis
Practice Questions
Biliary Atresia
Practice Questions
Pediatric Tumors
Practice Questions
Congenital Diaphragmatic Hernia
Practice Questions
Pediatric Trauma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
