Pancreatic Surgery — MCQs

On this page
A 50-year-old lady presents with a 2-year history of recurrent abdominal pain radiating to her back. The pain is severe and refractory to simple analgesics. Ultrasound abdomen and contrast-enhanced CT scan confirmed the diagnosis and showed a dilated pancreatic duct. Which of the following is the likely recommended surgical procedure of choice?
Hereditary pancreatitis is characterised by all except?
What is the gold standard investigation for chronic pancreatitis?
All are true about Zollinger-Ellison syndrome except?
All of the following can be used to predict severe acute pancreatitis except?
Which of the following is NOT an operation for chronic pancreatitis?
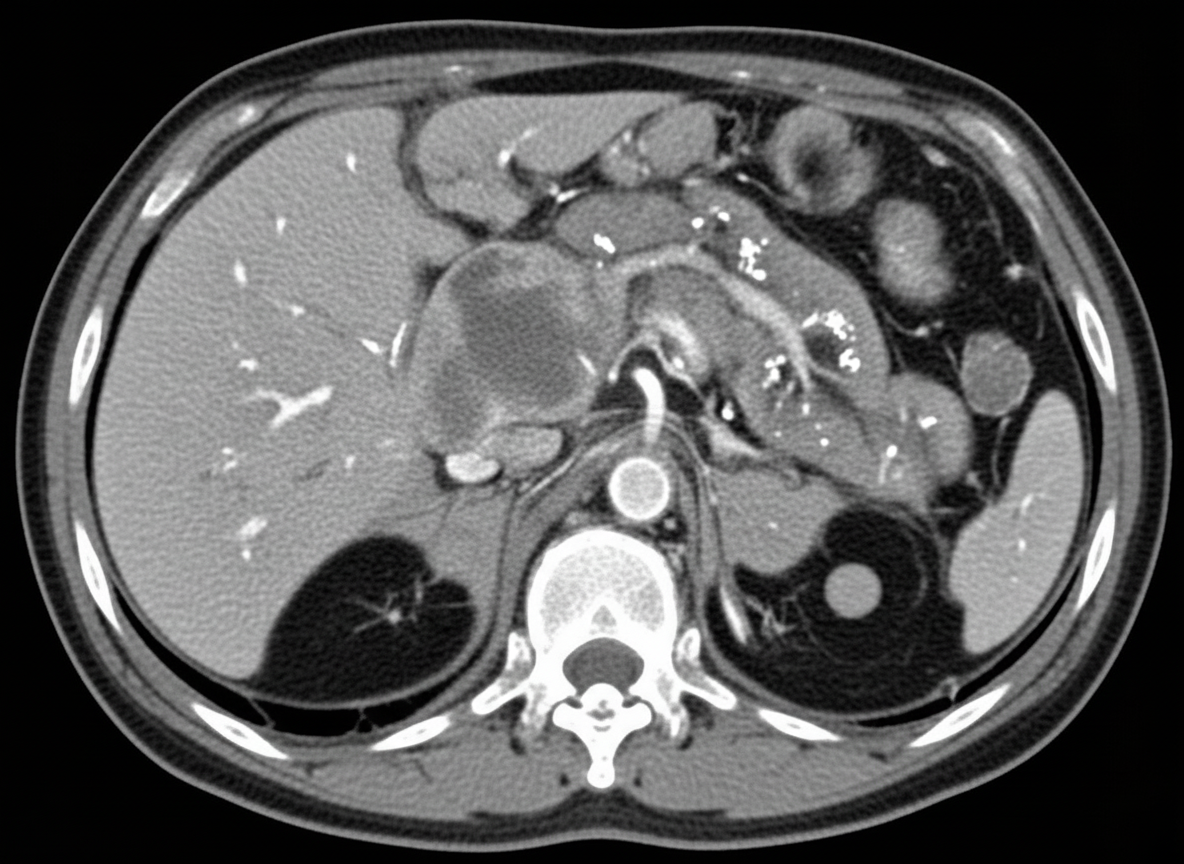
A 60-year-old woman with a history of chronic pancreatitis presents with worsening epigastric pain radiating to the back, accompanied by nausea and vomiting. She has experienced a 10 kg weight loss over the past 4 months. There is no evidence of jaundice, and liver function tests and serum amylase/lipase levels are within normal limits. A CT scan of the abdomen reveals significant findings. What is the most appropriate next step in managing this patient?
Which of the following is a poor prognostic factor in acute pancreatitis?
What is the most common site of ectopic pancreas?
Which of the following laboratory findings or scoring systems indicates severe pancreatitis?
Practice by Chapter
Pancreatic Anatomy and Physiology
Practice Questions
Acute Pancreatitis
Practice Questions
Chronic Pancreatitis
Practice Questions
Pancreatic Pseudocysts
Practice Questions
Pancreatic Adenocarcinoma
Practice Questions
Cystic Neoplasms of Pancreas
Practice Questions
Neuroendocrine Tumors of Pancreas
Practice Questions
Pancreatic Trauma
Practice Questions
Pancreatectomy Techniques
Practice Questions
Whipple Procedure
Practice Questions
Pancreatic Anastomosis
Practice Questions
Complications of Pancreatic Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
