Pancreatic Surgery — MCQs

On this page
Whipple's triad in insulinoma includes all of the following EXCEPT:
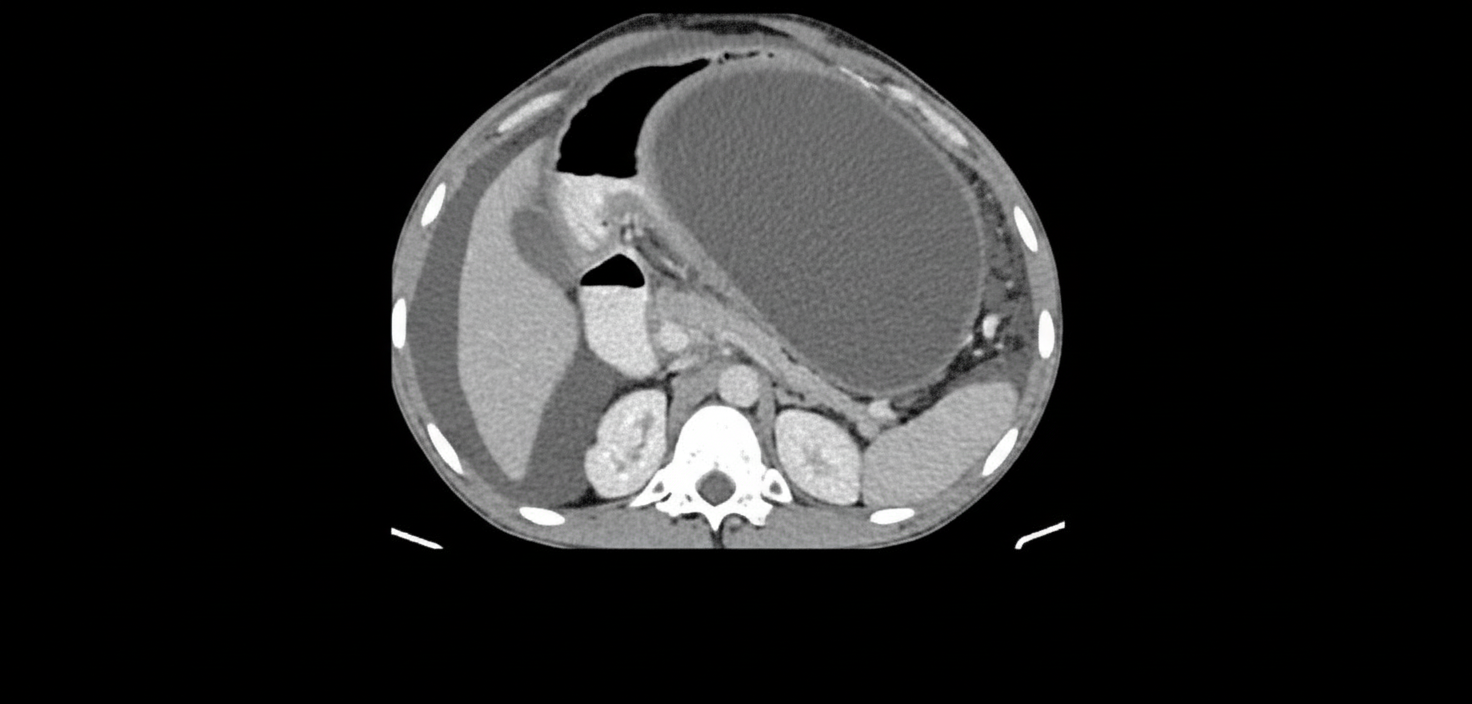
A 30-year-old patient presents with severe upper abdominal pain and elevated serum lipase. A CECT scan was performed and is shown. What is the next line of management?
Cullen's sign is seen in which of the following conditions?
All of the following are true about pancreatic cancer, EXCEPT:
Which of the following is FALSE about annular pancreas?
Which of the following criteria is NOT included in Ranson's criteria for predicting the severity of pancreatitis?
Whipple's operation is done for the treatment of which condition?
Which of the following does not affect prognosis in acute pancreatitis?
Localization in insulinoma is best with:
Which of the following clinical manifestations is most characteristic of a gastrinoma?
Practice by Chapter
Pancreatic Anatomy and Physiology
Practice Questions
Acute Pancreatitis
Practice Questions
Chronic Pancreatitis
Practice Questions
Pancreatic Pseudocysts
Practice Questions
Pancreatic Adenocarcinoma
Practice Questions
Cystic Neoplasms of Pancreas
Practice Questions
Neuroendocrine Tumors of Pancreas
Practice Questions
Pancreatic Trauma
Practice Questions
Pancreatectomy Techniques
Practice Questions
Whipple Procedure
Practice Questions
Pancreatic Anastomosis
Practice Questions
Complications of Pancreatic Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
