Pancreatic Surgery — MCQs

On this page
Which of the following is a cause of recurrent pancreatitis?
Which investigation is used to assess the resectability of pancreatic cancer?
A lady presented with recurrent attacks of giddiness and abdominal pain for three months. Endoscopy was normal. Her fasting blood glucose level was 40 mg/dL and insulin levels were elevated. CT abdomen showed a well-defined 8mm enhancing lesion in the head of the pancreas, with no other abnormal findings. What is the appropriate treatment plan?
Which of the following is the most common non-alcoholic cause of acute pancreatitis?
A 45-year-old female presented with vague abdominal pain. Laboratory investigations revealed normal amylase and raised CEA. A CT scan showed a hypodense lesion in the pancreas with internal septations and wall calcification. What is the most probable diagnosis?
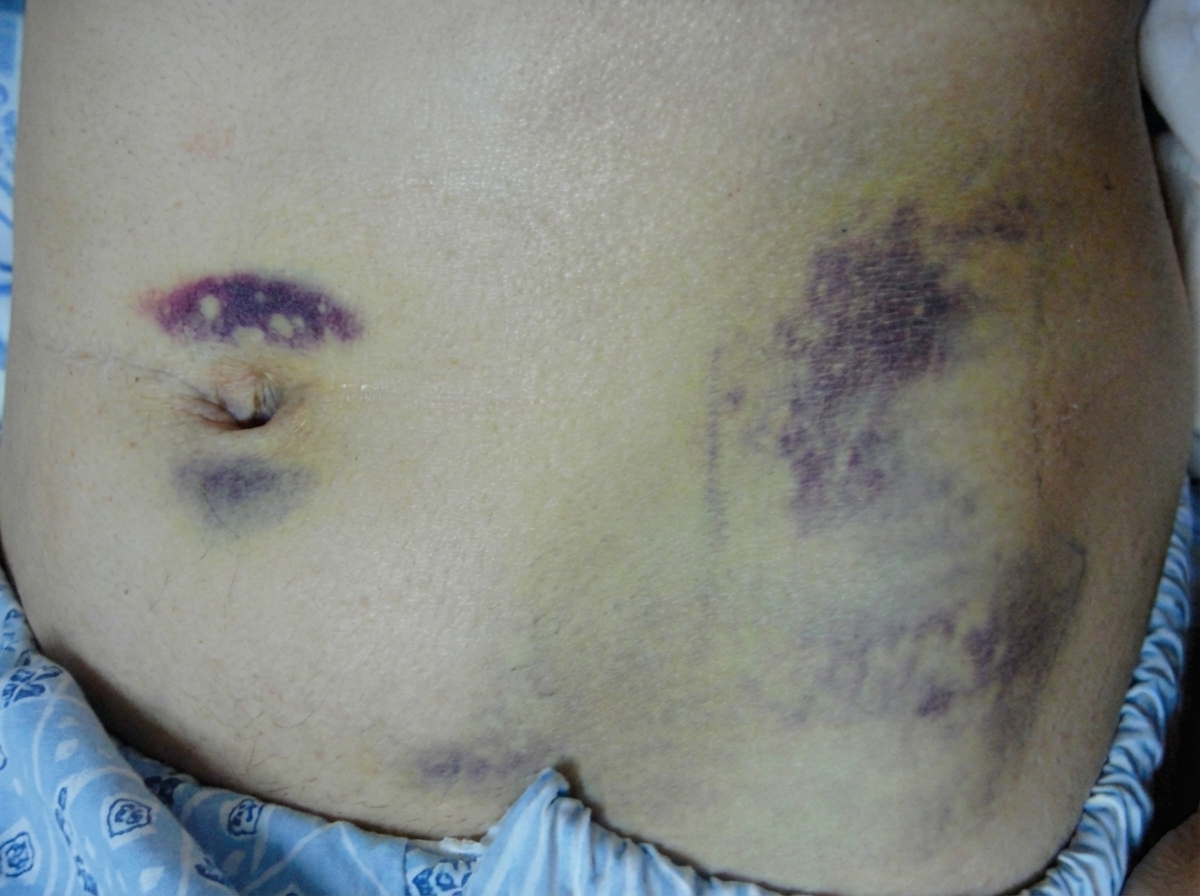
Bluish discoloration of the flank is known as which sign?
Which investigation can itself lead to acute pancreatitis?
The given signs are seen in which of the following conditions?
Tumor of which of the following cell types results in Zollinger-Ellison syndrome?
A patient with a known history of gallstones presents with severe abdominal pain and elevated serum lipase levels, along with periumbilical ecchymosis. Which of the following values helps to predict the severity of the condition, except?
Practice by Chapter
Pancreatic Anatomy and Physiology
Practice Questions
Acute Pancreatitis
Practice Questions
Chronic Pancreatitis
Practice Questions
Pancreatic Pseudocysts
Practice Questions
Pancreatic Adenocarcinoma
Practice Questions
Cystic Neoplasms of Pancreas
Practice Questions
Neuroendocrine Tumors of Pancreas
Practice Questions
Pancreatic Trauma
Practice Questions
Pancreatectomy Techniques
Practice Questions
Whipple Procedure
Practice Questions
Pancreatic Anastomosis
Practice Questions
Complications of Pancreatic Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
