Pancreatic Surgery — MCQs

On this page
Which statement is NOT true regarding insulinoma?
All of the following are known complications of pancreatitis except?
What is the investigation of choice to detect gastrinoma less than 5 mm in size?
Which of the following best assesses the severity of pancreatitis?
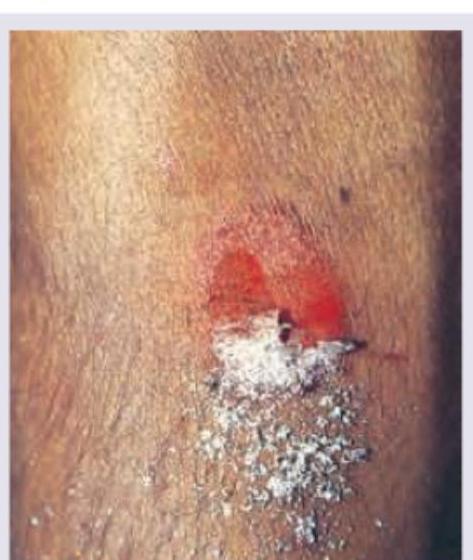
Which of the following neuroendocrine tumors of the pancreas is most commonly associated with the given manifestation?
The Duval procedure in chronic pancreatitis involves which of the following?
What is true regarding pancreatic trauma?
What are the treatment options for a pseudocyst of the pancreas?
What is the most common mutation in pancreatic adenocarcinoma?
A 35-year-old man presents with acute pancreatitis. What is the ideal fluid of choice for management?
Practice by Chapter
Pancreatic Anatomy and Physiology
Practice Questions
Acute Pancreatitis
Practice Questions
Chronic Pancreatitis
Practice Questions
Pancreatic Pseudocysts
Practice Questions
Pancreatic Adenocarcinoma
Practice Questions
Cystic Neoplasms of Pancreas
Practice Questions
Neuroendocrine Tumors of Pancreas
Practice Questions
Pancreatic Trauma
Practice Questions
Pancreatectomy Techniques
Practice Questions
Whipple Procedure
Practice Questions
Pancreatic Anastomosis
Practice Questions
Complications of Pancreatic Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
