Pancreatic Surgery — MCQs

On this page
Which of the following is the most common cause of pancreatic pseudocyst?
Complications of chronic pancreatitis include the following, except:
Which of the following is the most diagnostic investigation for acute pancreatitis?
What are the common causes of acute pancreatitis?
A chronic alcoholic presents with repeated episodes of severe intractable abdominal pain. On evaluation, the pancreatic duct was found to be dilated and stones were noted in the tail of the pancreas. What is the most appropriate management?
A 30-year-old known alcoholic patient presented with severe abdominal pain. On examination, a rigid abdomen is noted. The patient has a history of multiple episodes of abdominal pain over the last 4-5 years and has lost 5 kg of weight in the past 6 months. Serum lipase and amylase levels are normal. CECT abdomen was performed. What is the most likely diagnosis?
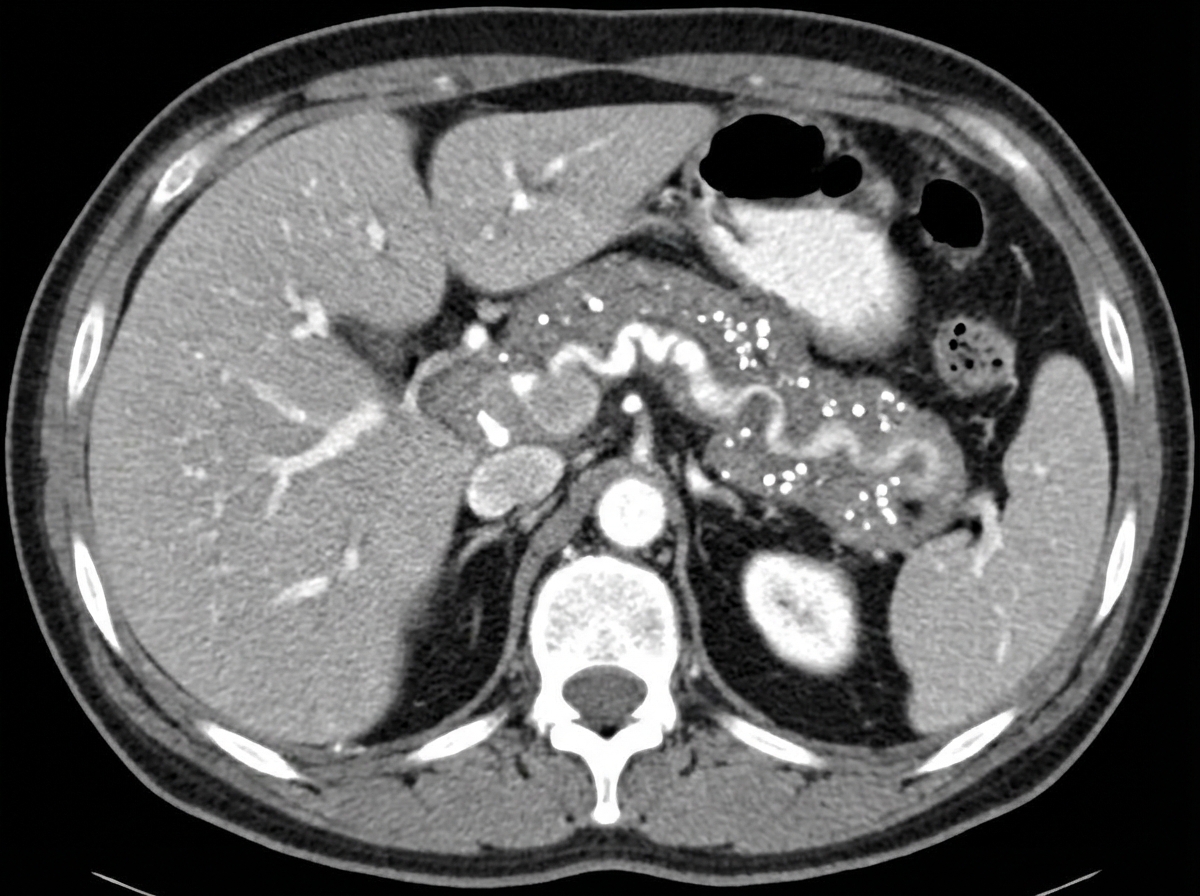
A patient presents with upper abdominal pain and vomiting. His pulse is 110/min and BP is 70/40 mm Hg. A diagnosis of pancreatitis is made. What is the next appropriate management?
A 41-year-old woman with a history of multiple endocrine neoplasia syndrome presents with severe diarrhea associated with low gastric acid secretion and a normal gastrin level. Her family history includes parathyroid, pancreatic, and/or pituitary adenomas. Which of the following serum assays would be best to evaluate the possible cause of the diarrhea?
What is the most common complication of chronic pancreatitis?
A 42-year-old man presents with recurrent right upper quadrant pain for 2 years. Sonography is negative for gallstones, and the common bile duct is normal. Upper GI endoscopy is also normal, and there is no peptic ulcer disease. Biliary dyskinesia is suspected, and the patient undergoes further evaluation. Which of the following stimulates gallbladder contraction?
Practice by Chapter
Pancreatic Anatomy and Physiology
Practice Questions
Acute Pancreatitis
Practice Questions
Chronic Pancreatitis
Practice Questions
Pancreatic Pseudocysts
Practice Questions
Pancreatic Adenocarcinoma
Practice Questions
Cystic Neoplasms of Pancreas
Practice Questions
Neuroendocrine Tumors of Pancreas
Practice Questions
Pancreatic Trauma
Practice Questions
Pancreatectomy Techniques
Practice Questions
Whipple Procedure
Practice Questions
Pancreatic Anastomosis
Practice Questions
Complications of Pancreatic Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
