Pancreatic Surgery — MCQs

On this page
What is the commonest cause of acute pancreatitis?
A 60-year-old chronic smoker presented with jaundice, anorexia, and weight loss. ERCP was performed. What is the most likely diagnosis based on ERCP findings?
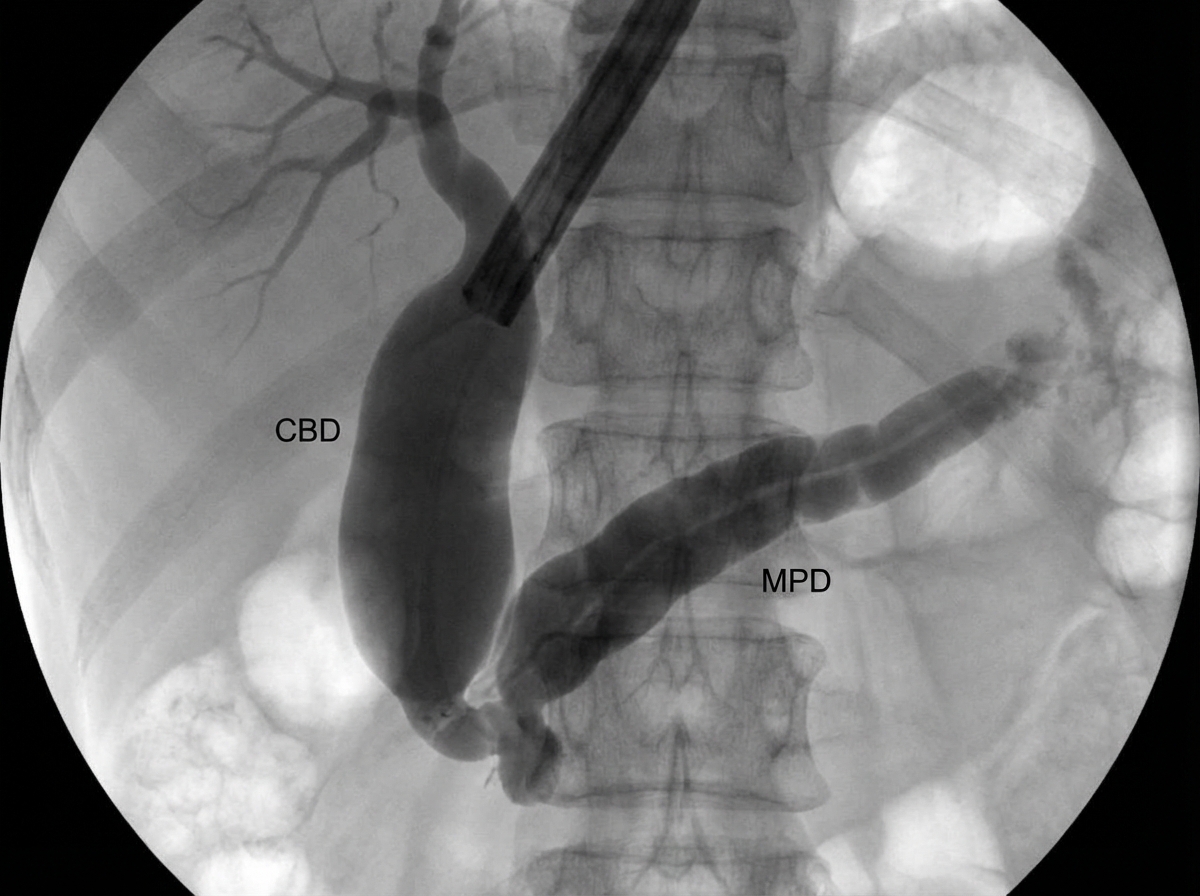
What is the best diagnostic modality for pancreatic cancer located in the head of the pancreas?
What is the treatment of choice for an asymptomatic pancreatic pseudocyst?
Which of the following is a poor prognostic factor in a patient with acute pancreatitis?
What is the most common functional neuroendocrine tumor of the pancreas?
The boundaries of the foramen of Winslow (epiploic foramen) include all of the following EXCEPT:
Which of the following is NOT a medical treatment for pancreatitis?
Which of the following types of pancreatitis has the best prognosis?
An adrenal biopsy should be considered after ruling out which of the following conditions?
Practice by Chapter
Pancreatic Anatomy and Physiology
Practice Questions
Acute Pancreatitis
Practice Questions
Chronic Pancreatitis
Practice Questions
Pancreatic Pseudocysts
Practice Questions
Pancreatic Adenocarcinoma
Practice Questions
Cystic Neoplasms of Pancreas
Practice Questions
Neuroendocrine Tumors of Pancreas
Practice Questions
Pancreatic Trauma
Practice Questions
Pancreatectomy Techniques
Practice Questions
Whipple Procedure
Practice Questions
Pancreatic Anastomosis
Practice Questions
Complications of Pancreatic Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
