Hepatobiliary Surgery — MCQs

On this page
"Limey bile" is:
Which of the following is NOT an indication for percutaneous aspiration in amoebic liver abscess?
Which artery should be preserved during the operation of a common bile duct stricture?
Which of the following is NOT true regarding cystic duct stump stones?
What is the surgery of choice for diffuse type of choledochal cyst?
Which of the following statements is true regarding cholangitis?
The 'Push, Pringle, Plug and Pack' technique is used for managing which organ's bleeding?
What is the best treatment for the given type of cholecystitis?
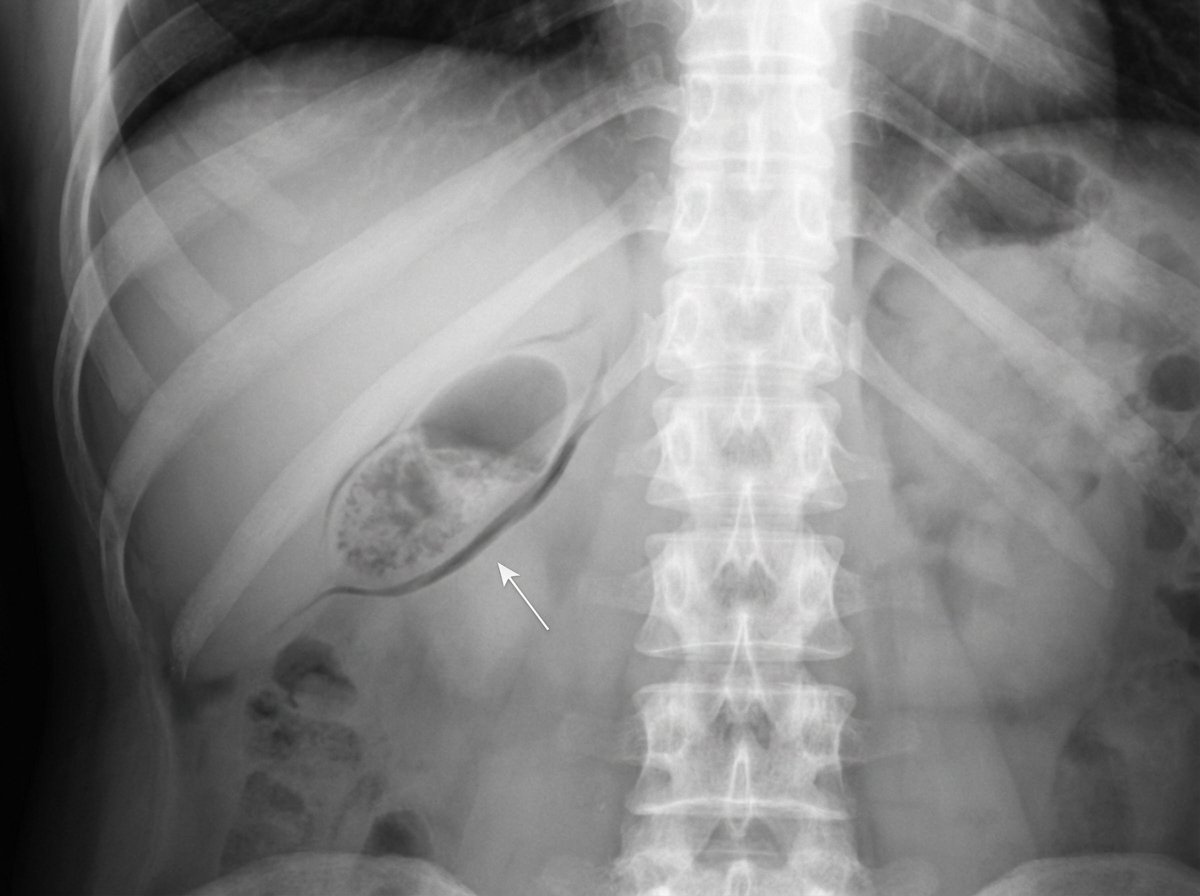
In gallbladder mucocele, where is the stone usually impacted?
80% of gallstones contain which of the following?
Practice by Chapter
Liver Anatomy and Physiology
Practice Questions
Benign Liver Lesions
Practice Questions
Liver Abscess
Practice Questions
Hepatocellular Carcinoma
Practice Questions
Metastatic Liver Disease
Practice Questions
Cirrhosis and Portal Hypertension
Practice Questions
Liver Trauma
Practice Questions
Cholelithiasis and Cholecystitis
Practice Questions
Choledocholithiasis
Practice Questions
Biliary Tract Tumors
Practice Questions
ERCP and Its Complications
Practice Questions
Liver Transplantation Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
