Hepatobiliary Surgery — MCQs

On this page
Most faceted gallstones are formed in which organ?
What is true about carcinoma of the gallbladder?
Which of the following statements about gall stones is TRUE?
A patient underwent laparoscopic cholecystectomy. Histopathology revealed T2 stage. What is the next line of treatment?
Intraoperative cholangiography is indicated in which of the following conditions?
Identify the type of gallstone shown below.
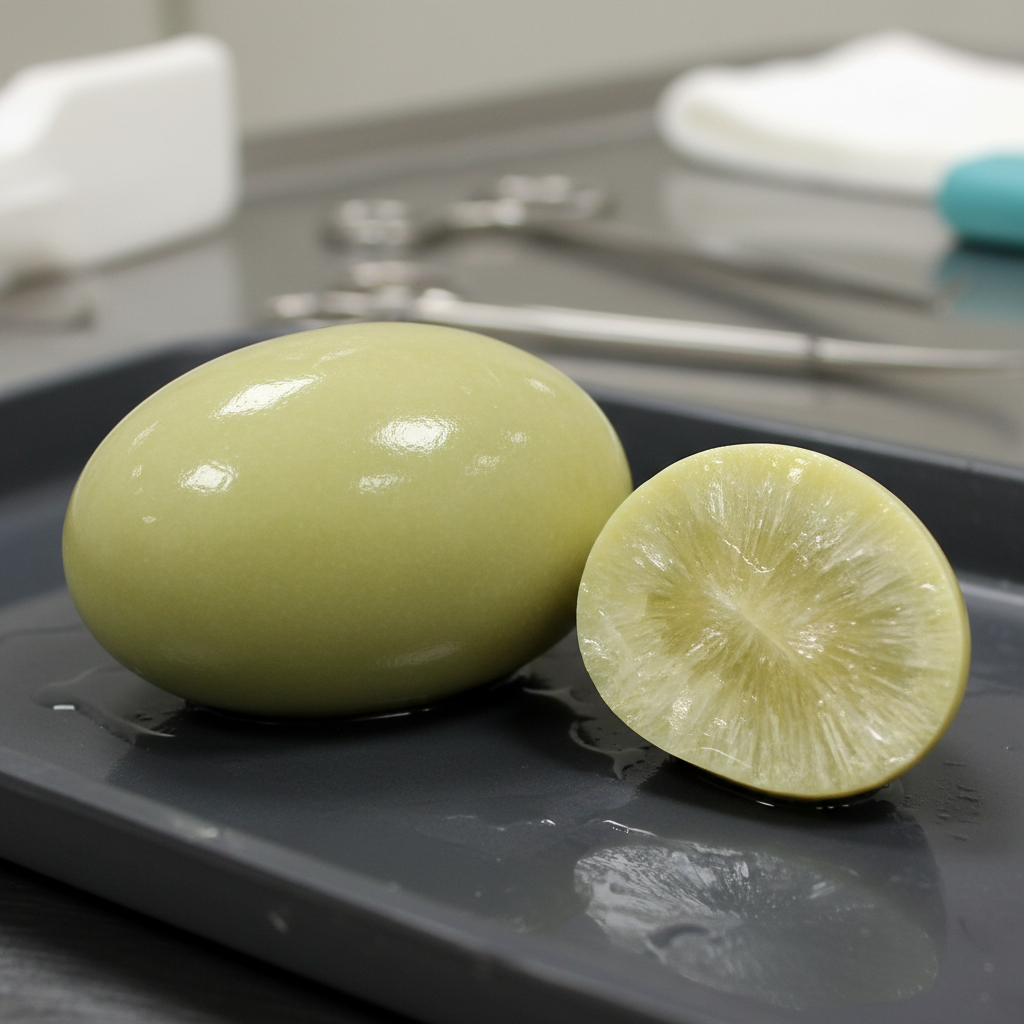
Which statement is true regarding hemobilia?
Surgical lobes of the liver are divided on the basis of which vascular structures?
Biliary stricture developing after laparoscopic cholecystectomy usually occurs at which part of the common bile duct?
What is Type II Mirizzi's syndrome characterized by?
Practice by Chapter
Liver Anatomy and Physiology
Practice Questions
Benign Liver Lesions
Practice Questions
Liver Abscess
Practice Questions
Hepatocellular Carcinoma
Practice Questions
Metastatic Liver Disease
Practice Questions
Cirrhosis and Portal Hypertension
Practice Questions
Liver Trauma
Practice Questions
Cholelithiasis and Cholecystitis
Practice Questions
Choledocholithiasis
Practice Questions
Biliary Tract Tumors
Practice Questions
ERCP and Its Complications
Practice Questions
Liver Transplantation Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
