Hepatobiliary Surgery — MCQs

On this page
Regarding choledochal cysts following features are true except:
In Pringle Manoeuvre, clamping includes which of the following? 1. Common Bile Duct 2. Hepatic artery 3. Portal vein 4. Inferior Vena Cava
A patient is found to have an asymptomatic common bile duct (CBD) stone two years after cholecystectomy on routine imaging. What is the most appropriate initial management?
The following procedure is performed for the management of?
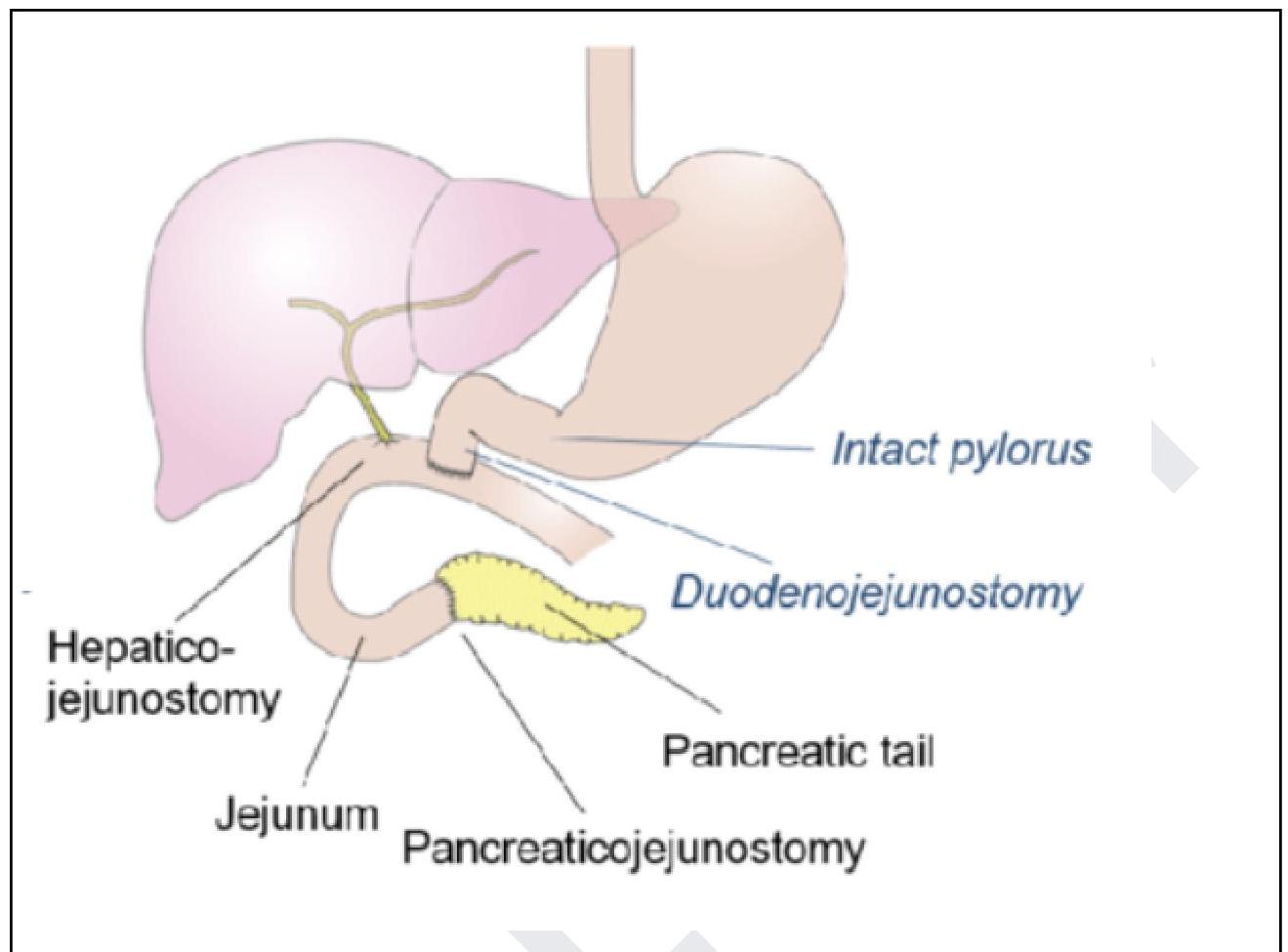
Most common type of choledochal cyst is:
A 52-year-old woman presents with jaundice, pale stools, and a palpable gallbladder. MRCP shows a dilated bile duct but no stones. What is the next best step?
A 45-year-old woman presents with right upper quadrant pain and fever. Ultrasound reveals gallstones with dilation of the bile ducts. What is the most appropriate next step?
What is the first-line diagnostic method for cholecystitis?
A 60-year-old male with a history of cirrhosis presents with a 4 cm hepatocellular carcinoma (HCC) located in segment VII of the liver. Considering the patient has Child-Pugh A liver function, which clinical factors are most critical in deciding between liver resection and radiofrequency ablation (RFA)?
Which anatomical division of the liver is typically used to describe the location of lesions for surgical planning?
Practice by Chapter
Liver Anatomy and Physiology
Practice Questions
Benign Liver Lesions
Practice Questions
Liver Abscess
Practice Questions
Hepatocellular Carcinoma
Practice Questions
Metastatic Liver Disease
Practice Questions
Cirrhosis and Portal Hypertension
Practice Questions
Liver Trauma
Practice Questions
Cholelithiasis and Cholecystitis
Practice Questions
Choledocholithiasis
Practice Questions
Biliary Tract Tumors
Practice Questions
ERCP and Its Complications
Practice Questions
Liver Transplantation Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
