Hepatobiliary Surgery — MCQs

On this page
A 20-year-old patient presents with fever and tenderness in RUQ. CT abdomen shows a lesion measuring 10 cm × 4 cm. Which is the preferred site for aspiration?
Which classification is used to evaluate the condition shown in the image below?
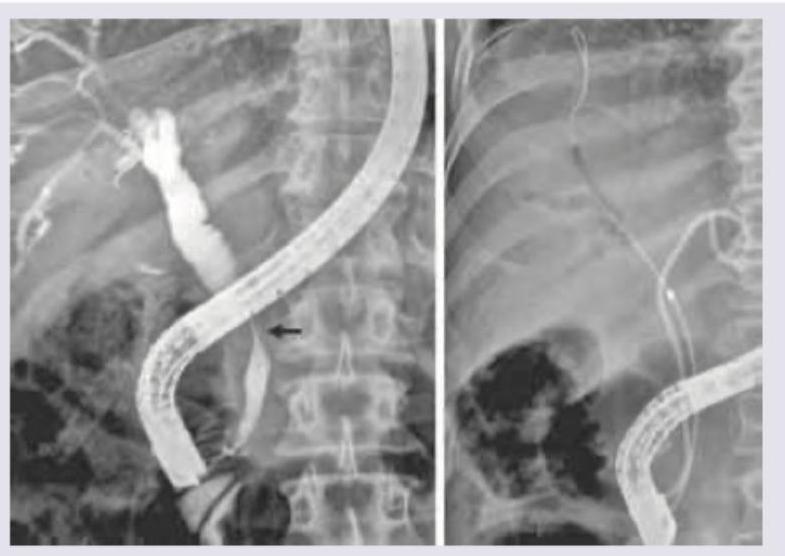
What type of choledochal cyst is shown in the image?
Which is correct about hematemesis (upper GI bleeding) in this patient?
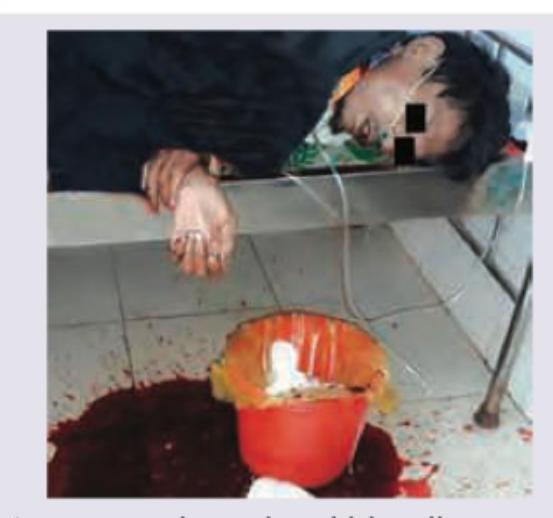
The image shows: (DNB Pattern 2018)
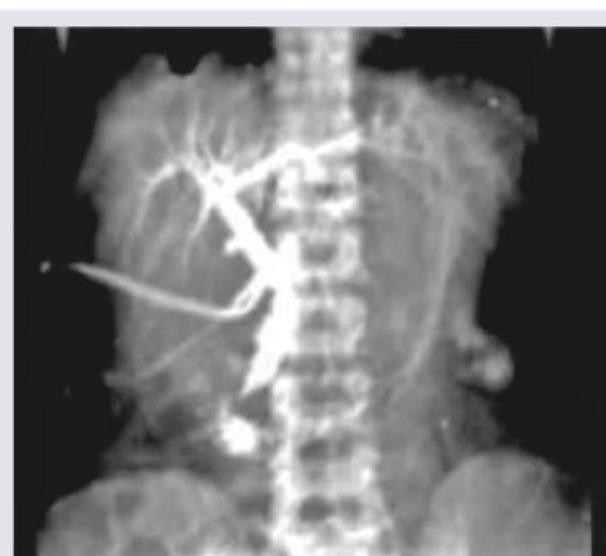
The following image shows: (DNB Pattern 2018)
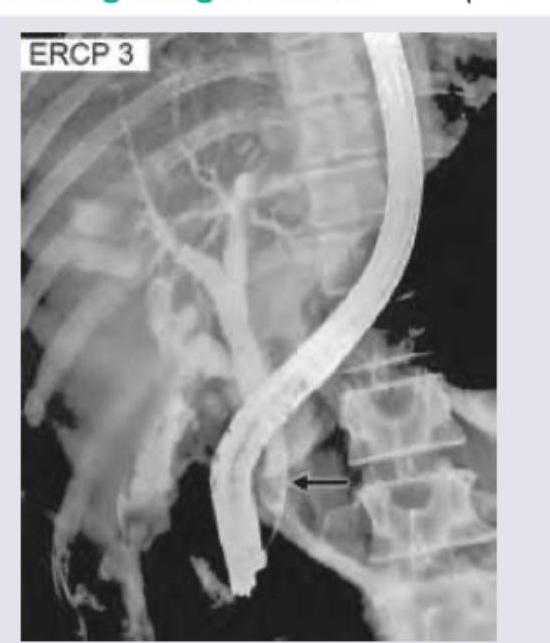
A young patient develops high grade fever with chills and rigors, mild jaundice and acute pain in the upper abdomen following cholecystectomy. On examination she was jaundiced, toxic, haemodynamically stable and having vague fullness upper abdomen. What is the most probable diagnosis ?
The percutaneous PAIR therapy used in the treatment of uncomplicated hepatic hydatid cyst can be associated with the following complications, except
Pringle's manoeuvre is done to stop bleeding at:
Regarding carcinoma gall bladder following features are true except:
Practice by Chapter
Liver Anatomy and Physiology
Practice Questions
Benign Liver Lesions
Practice Questions
Liver Abscess
Practice Questions
Hepatocellular Carcinoma
Practice Questions
Metastatic Liver Disease
Practice Questions
Cirrhosis and Portal Hypertension
Practice Questions
Liver Trauma
Practice Questions
Cholelithiasis and Cholecystitis
Practice Questions
Choledocholithiasis
Practice Questions
Biliary Tract Tumors
Practice Questions
ERCP and Its Complications
Practice Questions
Liver Transplantation Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
